 |
 |
| Korean J Intern Med > Volume 17(4); 2002 > Article |
|
Abstract
Background
Pulmonary inflammatory pseudotumor is an uncommon benign lesion of the lung. In Korea, most literature of the pulmonary inflammatory pseudotumor was case reports.
Methods:
We collected 28 cases of pulmonary inflammatory pseudotumor in Korea. This collective series included 4 cases from our hospital and 24 cases were reviewed from the literature since 1977. The analysis involved the age, sex, chief complaint, hematologic examination, size and location of the lesion, cavity formation, presence of calcification and treatment method.
Results:
Male was more prevalent (81.5%) than female and mean age was 37.9 years old (6–63 yrs). Chief complaints were cough (44.4%), chest pain (29.6%), fever (22.2%), hemoptysis (15%), sputum (15%) and dyspnea (11.1%). There were asymptomatic cases in 11.1%. Hematologic examination revealed normal finding (53.3%) and anemia (20%). The mean size of the lesion was 4.76 cm (1.5–14 cm) and the locations were parenchymal (85.7%), endobronchial (10.7%) and endotracheal (3.6%). Except the endotracheal case, the lesions were in the right (46.4%), the left (42.8%) and bilateral (7.1%). Calcifications (18.5%) and cavitations (11.1%) were present. Diagnostic methods were open thoracotomy (82.1%), bronchoscopy (3.6%), needle aspiration biopsy (7.1%) and core needle gun biopsy (7.1%). Treatments were surgery (85.2%), steroid therapy (7.4%), rigid bronchoscopic removal (3.7%) and observation (3.7%). Postoperative recurrence occurred in only 1 case (4.3%).
Pulmonary inflammatory pseudotumor is a relatively rare benign tumor located in the lungs but could occur in the mesentry, greater omentum, liver, bladder and upper respiratory tract. Most of the patients are under 40 years of age and complain mainly of non-specific symptoms. Lesions are shown as pulmonary nodules or masses in which the border can be characteristically well distinguished on X-ray. Diagnosis of this tumor is difficult without surgical biopsy or resection. It is principally treated with surgery. This tumor was reported as fibrous histiocytoma, plasma cell granuloma and inflammatory pseudotumor in Korea. A total of 27 cases of pulmonary inflammatory pseudotumor have been reported in Korea, including 3 cases reported from Severance Hospital, until January 2001. However, most of the cases were simple case reports so that comprehensive discussion on pulmonary inflammatory pseudotumor was not enough in those series. Thus, we conducted a review of the literature on pulmonary inflammatory pseudotumor, including a case that we recently experienced, to examine the clinical features, diagnosis and treatment of this disease.
We collected 28 cases of pulmonary inflammatory pseudotumor in Korea, including 4 cases that we experienced at the Severance Hospital, and supplemented from the literature reported as fibrous histiocytoma, plasma cell granuloma and inflammatory pseudotumor since 1977.
Through the review of the literature, we collected the patients’ data, including age, gender, chief complaint, hematologic examination, size and location of the lesion, cavity formation, presence of calcification and treatment method. Referring to the studies already published, some items were not available for each case2, 8, 10, 12, 14). Information for the gender of the patient could be confirmed in 27 cases, that for the age in 20 cases, and that for the clinical pattern in 27 cases. Hematologic findings were described in 15 cases. Size of the lesion could be determined in 21 cases. Radiographic or pathologic findings were described in 27 cases. Diagnostic method could be confirmed in 28 cases and treatment method in 27 cases.
The cases of pulmonary inflammatory pseudotumor reported in Korea are summarized in Table 1. Male was more prevalent than female in 22 out of 27 cases (81.5%) and the mean age was 37.9 years old (range: 6–63 yrs).
As for the clinical features, a majority of the patients, 12 cases (44.4%) out of 27 cases, complained of cough, followed by chest pain in 8 cases (29.6%), fever in 6 cases (22.2%), hemoptysis and sputum in 4 cases (15%), respectively, and dyspnea in 3 cases (11.1%). Other symptoms, including dyspnea on exertion, general weakness, headache, upper abdominal pain and blood tinged sputum, were present in one case, respectively. Respiratory symptoms were present in 22 cases (78.6%) out of 28 cases at the time of diagnosis. Three cases (11.1%) were asymptomatic.
Among those 15 cases in which the hematologic findings could be determined, there was normal finding in 8 cases (53.3%), anemia in 3 cases (20%) and neutropenia, thrombocytopenia, eosinophilia, leukocytosis, elevated ESR in one case, respectively (6.7%). Leukocytosis was observed together with anemia in one case13)
Based on the longest diameter, the average size of the lesion was 4.8 cm (1.5–14 cm). As for the location of the lesion in 28 cases, there was lung parenchymal lesion in 24 cases (85.7%), endobronchial lesion in 3 cases (10.7%) and endotracheal lesion in 1 case (3.6%). Other than the endotracheal lesion, the lesion was in the right side in 13 cases (46.4%), in the left side in 12 cases (42.8%) and bilateral in 2 cases (7.1%).
In 27 cases with radiographic or pathologic findings stated, calcification was seen in 5 cases (18.5%)7, 8, 13, 15, 16) and cavity formation was seen in 3 cases (11.1%)8, 14).
As for the diagnostic methods, the open thoracotomy was the most prevalent with 23 cases (82.1%) out of 28 cases; among these 23 cases, one case was diagnosed accidentally after the patient underwent left lower lobectomy due to bronchiectasis. Otherwise, the tumor was totally removed using a bronchoscope in 1 case (3.6%)3), and was diagnosed through percutaneous fine needle aspiration (FNA) biopsy in 2 cases (7.1%)11, 16) and core needle gun biopsy in 2 cases (7.1%)14).
As for treatment, thoracotomy was performed in 23 cases (85.2%) out of 27 cases. Rigid bronchoscopic removal was performed in 1 case (3.7%)3). Prednisolone therapy was done in 2 cases (7.4%) out of 27 cases; in one case, a daily dose of 15 mg was given for 45 days with tapering11). We used 20 mg of prednisolone on the first day and tapered it within the 6 month treatment period. One case (3.7%) showed improvement with the lesion being decreased and symptoms improved with conservative treatment16). Recurrence after surgery was reported in 1 case (4.3%)6) out of 23 cases.
As a relatively rare benign disease, the rate of inflammatory pseudotumor located in the lung is 0.7% of all tumors developing in the lung parenchyma and bronchus17) and the rate of tumor development within the bronchus is 6.6% of pulmonary inflammatory pseudotumor18) According to the study by Park et al.10) in 1992, only one case (3.3%) of inflammatory pseudotumor was seen out of 30 cases of benign lung tumors. No gender difference was known to be present and more than a half of the patients were under 40 years of age and 15% of those patients were between the ages of 1–10 years18, 19) In this study, 81.5% of the cases were male, 55% of them were under 40 years of age, and 1 case was a child under 6 years of age9).
Pulmonary inflammatory pseudotumor is considered as an inflammatory or reactive lesion rather than neoplasm, and about 30% of the patients had a past history of respiratory infection20, 21). Although the cause of this disease has not been determined accurately, inflammatory lesions are thought to occur locally as a result of excessive response to tissue damages22).
About 60 – 70% of the patients complained of cough, fever, dyspnea and chest pain23). The results of the present study showed that the symptoms were present in 24 cases (88.9%) out of 27 cases. The asymptomatic 3 cases were incidentally noted by chest X-ray abnormality14).
Laboratory findings were usually within the normal ranges and some could show thrombosytosis, elevated ESR and multiclonal hypergammaglobuminemia24).
Characteristic findings of chest X-ray revealed a solitary, peripheral, sharply circumscribed and lobulated mass25). Those cases with the lesions developed in the bronchus can show obstructive pneumonia or findings of atelectasis, can spread into the lung hilum or mediastinum and rarely accompany pleural effusion25). Calcification is seen with larger lesions20) and lesions are known to form a cavity rarely25). Although calcification was reported in 5 cases in Korea7, 8, 13, 15, 16), it was not related with the size of the lesion. Cavity formation could be seen in 3 cases8, 14).
On gross examination of pulmonary inflammatory pseudotumor, a single oval intrapulmonary mass can be demarcated well, it shows golden-brown or red-brown color with no capsule and it is hard in consistency. It can show hemorrhage, necrosis or micro-calcification deposit19, 25). Histologically, mature plasma cells are the major component of the mass, and fibroblasts, gelatinous substance and, characteristically, the Russel bodies are scattered in palisade or axel form within the hyaline material19). According to histological characteristic, it is distinguished into plasma cell granuloma and histiocytoma. The former form is composed of fibroblast, myofibroblast, collagen and inflammatory cells, and has spindle cells in long and short bundles20). In the latter form, collagen, spindle cells and macrophages are arranged in a whirlpool form and osteodysplasia and calcification can be present21). However, these two are considered to be the same disease since many pathologic findings are repeated and they are clinically very similar26).
Since the findings of inflammation and fibrosis seen in pulmonary inflammatory pseudotumor can be found around the lesion of lung cancer as a reactive response, FNA biopsy may not be an appropriate method of diagnosing inflammatory pseudotumor21). However, the diagnosis of pulmonary inflammatory pseudotumor may be suggested if the combination of a localized density on a chest X-ray and the FNA cytologic findings an taken into account27). Therefore, repeated FNA biopsy can be recommended for diagnosis28). It was reported that a higher accuracy rate can be obtained using core needle gun biopsy compared with FNA biopsy in chest lesions29). Other than pathologic diagnosis after surgery, the diagnosis was made with percutaneous FNA biopsy in 2 cases and with core needle gun biopsy in 2 cases in Korea. However, since the findings of pulmonary inflammatory pseudotumor are non-specific and the disease is not distinguished well from lung cancer or metastatic cancer, the diagnosis of this disease before surgery is rare. Pulmonary inflammatory pseudotumor needs to be distinguished from sclerosing hemangioma, pseudolymphoma and malignant sarcoma12).
Surgery is the treatment of choice in pulmonary inflammatory pseudotumor to distinguish between malignant tumors18, 19, 22, 23). Among 27 cases in which surgery was performed, thoracotomy was performed in 23 cases and removal of the tumor using a bronchoscope was performed in 1 case. Recurrence is reported to be rare18). Only one case of recurrence was reported in Korea from the authors’ affiliated hospital6). The inflammatory pseudotumor recurred in the meninges after 10 years and was treated with corticosteroids for 6 years. The follow-up periods were not long and the recurrence might be underestimated even in the world literature because the information from the review of the literature were collected at the time of the report. When lesions were impossible to remove surgically or not removed completely, steroid therapy11, 24, 30) or radiation therapy31) were also performed. There was a report that oral prednisolone at the dose of 2 mg/kg/d for 15 weeks reduced the size of lung infiltration24). Oral steroid could be administered in recurred cases after the surgery30). There was a complete disappearance of the mass on chest X-ray with 15 mg/d of prednisolone for 45 days in a Korean report11). We observed the disappearance of the mass on serial chest X-ray and symptomatic improvement with the administration of prednisolone started from 20 mg/d, then tapered for 6 months; no signs of recurrence were seen during the 12 month follow-up. There was a case in which the lesion was decreased and symptoms improved with no specific treatment.
In conclusion, pulmonary inflammatory pseudotumor was more prevalent in the male and patients presenting with the respiratory symptoms were common. It was necessary to do surgery in most cases for the diagnosis and/or treatment.
Figure 1.
52-year-old man with pulmonary inflammatory pseudotumor. The chest radiograph showed a huge mass-like density in the left upper and lower lung fields.

Figure 2.
The chest CT scan showed a huge mass in the posterior segment of left upper lobe and the superior segment of left lobe. It disclosed the multiple cavitary or cystic lesions and air bronchograms.
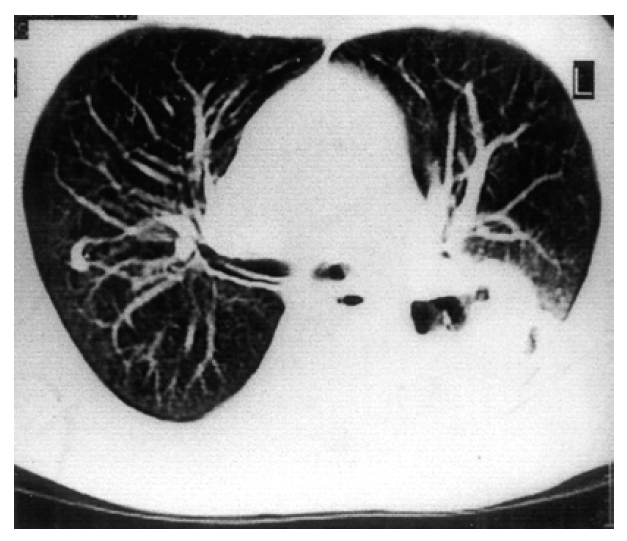
Figure 3.
The chest CT scan showed a huge mass in the posterior segment of left upper lobe and the superior segment of left lobe. It disclosed the multiple cavitary or cystic lesions and air bronchograms.

Figure 4.
Microscopic findings of the biopsy specimen showed dense lymphoplasmacytic infiltration within fibrotic stroma. (H&E stain, ×40)
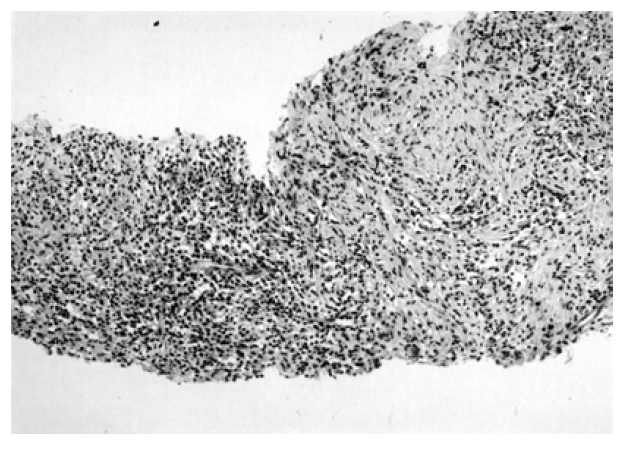
Figure 5.
Microscopic findings of the biopsy specimen showed dense lymphoplasmacytic infiltration within fibrotic stroma. (H&E stain, ×200)

Figure 6.
Twelve months later, the follow-up chest radiograph with the use of prednisolone revealed a marked-size reduction of the mass.

Table 1.
Summary of Features of Pulmonary Inflammatory Pseudotumors in Korea
| Authors | Sex | Age (yr) | Chief complaint | Hematologic exam | Size, location of mass | Cavitation | Calcification | Treatment |
|---|---|---|---|---|---|---|---|---|
| Lee et al1) | M | 29 | dyspnea, chest pain | neutropenia |
4×2.5 cm, RUL* 7×6 cm, RML |
no | no | bilobectomy |
| Kwak et al2) | F | 31 | general weakness, headache | anemia | 6.5×7.5 cm, LML | no | no | lobectomy |
| Kim et al3) | M | 17 | hemoptysis, dyspnea | not described | 1.5×1.5×1.2 cm, trachea | no | no | bronchoscopic removal |
| Yoo et al4) | M | 33 | dyspnea on exertion, cough | normal | 1.5 cm, endobronchus of left main | no | no | pneumonectomy |
| Chong et al5) | F | 44 | chest pain | anemia | not described, RML and RLL | no | no | pneumonectomy |
| M | 30 | dry cough | normal | diameter 2.5 cm, LLL | no | no | lobectomy | |
| Lee et al6) | F | 24 | cough, fever | normal | 4×4 cm, RLL | no | no | lobectomy |
| F | 46 | hemoptysis | normal | not described, LUL | no | no | lobectomy, recurred | |
| Ryoo et al7) | M | 17 | chest discomfort, cough | normal | 5.5×6.0 cm, RUL | no | yes | lobectomy |
| Kim et al8) | M | 55 | hemoptysis, cough, chest pain | not described | 5×5 cm, RML | no | yes | lobectomy |
| M | 31 | fever, chill, chest pain | not described | 5×4 cm, LLL | yes | no | lobectomy | |
| M | 58 | cough, sputum | not described | 5×7 cm, RUL | no | no | lobectomy | |
| Park et al9) | M | 6 | cough, fever | thrombocytopenia | not described, RML | no | no | lobectomy |
| Park et al10) | - | - | bronchiectasis | not described | not described, LLL | - | - | lobectomy |
| Bang et al11) | M | 58 | sputum | eosinophilia | 6.0×3.3 cm, 3.0×2.5 cm, LLL, 2.8×2.4 cm, LUL, 3.2×2.5 cm, 1.6×1.2 cm, RLL | no | no | steroid therapy |
| Chae et al12) | M | 37 | fever, chill, cough | not described | 2×1.5×0.5 cm, endobronchus of LLL | no | no | segmentectomy |
| Jeon et al13) | M | 61 | dyspnea on exertion, chest pain | leukocytosis, anemia | not described, left lung | no | yes | pneumonectomy |
| Kim et al14) | M | - | right lower chest pain | not described | 5 cm, RLL | no | no | wedge resection |
| M | - | incidentally discovered | not described | 2 cm, RML | no | no | wedge resection | |
| M | - | incidentally discovered | not described | 3 cm, RUL | no | no | wedge resection | |
| M | - | incidentally discovered | not described | 3 cm, RUL | no | no | lobectomy | |
| M | - | intermittent chest pain | not described | 4 cm, LLL | no | no | lobectomy | |
| M | - | blood tinged sputum productive cough | not described | 6 cm, LUL | no | no | lobectomy | |
| M | - | cough, purulent sputum | not described | not described, RUL, RLL, and LLL | yes | no | not described | |
| Kim et al15) | M | 46 | right upper quadrant pain | normal | 5.0×4.0 cm, RUL | no | no | wedge resection |
| F | 20 | dyspnea, cough, sputum | normal | not described, endobronchus of right main | no | yes | lobectomy | |
| Choi et al16) | M | 63 | intermittent fever | elevated ESR | 3 cm, LUL | no | yes | spontaneous regression |
| Kim et al** | M | 52 | fever, cough, hemoptysis | normal | 7×7×14 cm, LUL and LLL | yes | no | steroid therapy |
REFERENCES
1. Lee KS, Kim CW, Kim KH, Kim KH. A case of primary fibrous histiocytoma of the lung. Kor J Pathol 11:141–1461977.
2. Kwak YT, Park JC, Yoo SY. Plasma cell granuloma - one case report. Kor J Thorac Cardiovasc Surg 14:225–2271981.
3. Kim SK, Choi KH, Kim KH, Kang MS, Hong PW, Yang WI, Park CI. Fibrous histiocytoma of the trachea. Kor J Med 26:308–3111983.
4. Yoo SH, Kook SP, Suh SK, Kim HM, Choi CS. Inflammatory pseudotumor (histiocytoma) of the left main bronchus. Kor J Med 27:1520–15231984.
5. Chong DY, Han BS, Jang DC, Lim SP, Hong JS, Lee Y. Plasma cell granuloma of the lung - a report of 2 cases. Kor J Thorac Cardiovasc Surg 18:487–4911985.
6. Lee H, Sohn HY, Ahn CM, Kim SK, Kim KH. Two cases of inflammatory pseudotumors of the lung. Tuberc Respir Dis 33:252–2571986.


7. Ryoo JY, Woo JS, Cho KH. Plasma cell granuloma of the lung - a report of one case. Kor J Thorac Cardiovasc Surg 20:821–8241987.
8. Kim HS, Hur B, Chang HK, Huh MH. Inflammatory pseudotumor of the lung - three cases reported. Kor J Pathol 22:317–3231988.
9. Park SH, Choe GY, Kim CW, Chi JG, Sung SH. Inflammatory pseudotumor of the lung in a child with mycoplasma pneumonia. J Kor Med Sci 5:213–2231990.



10. Park K, Cho DG, Park JK, Jo GH, Wang YP, Kwack MS, Kim SW, Lee HK. Surgical treatment of benign lung tumor. Kor J Thorac Cardiovasc Surg 25:258–2701992.
11. Bang SH, Kim CH, Kwon SS, Kim YK, Kim KH, Moon HS, Song JS, Park SH. A case of inflammatory pseudotumor completely resolved by steroid therapy. Tuberc Respir Dis 40:709–7131993.


12. Chae SW, Choi YH, Ahn HK, Park YE. Endobronchial inflammatory pseudotumor - a case report. Kor J Pathol 28:213–2151994.
13. Jeon YB, Lee JH, Yang SH, Kim H, Jung WS, Lee CB, Kang JH. Inflammatory pseudotumor of the entire left lung - 1 operative case report. Kor J Thorac Cardiovasc Surg 30:437–4401997.
14. Kim HS, Jung GS, Baek KH, Lee SR, Huh JD, Joh YD, Jang HK. Inflammatory pseudotumor of the lung: CT findings and pathologic correlation. J Kor Radiol Soc 38:75–821998.

15. Choi SY, Cho YK, Bai IK, Hong SS, Lee MS, Chung DR, Wo JH, Ryu JS. Pulmonary inflammatory pseudotumor presenting as fever of unknown origin. Kor J Infect Dis 31:435–4381999.
16. Kim JG, Jeong NY, Kim KH, Kim HS, Lee WY, Yong SJ, Shin KC, Yang SW, Jeong SH. Two cases of inflammatory pseudotumor in respiratory system. Tuberc Respir Dis 46:394–4011999.

18. Berardi RS, Lee SS, Chen HP, Stines GJ. Inflammatory pseudotumors of the lung. Surg Gynecol Obstet 156:89–961983.

21. Matsubara O, Tan-Liu NS, Kenney RM, Mark EJ. Inflammatory pseudotumors of the lung: progression from organizing pneumonia to fibrous histiocytoma or to plasma cell granuloma in 32 cases. Hum Pathol 19:807–8141988.


22. Coffin CM, Dehner LP, Meis-Kindblom JM. Inflammatory myofibroblastic tumor, inflammatory fibrosarcoma and related lesions: an historical review with differential diagnostic considerations. Semin Diagn Pathol 15:102–1101998.

23. Copin MC, Gosselin BH, Ribet ME. Plasma cell granuloma of the lung: difficulties in diagnosis and prognosis. Ann Thorac Surg 61:1477–14821996.


24. Doski JJ, Priebe CJ Jr, Driessnack M, Smith T, Kane P, Romero J. Corticosteroids in the management of unresected plasma cell granuloma (inflammatory pseudotumor) of the lung. J Pediatr Surg 26:1064–10661991.


25. Agrons GA, Rosado-de-Christenson ML, Kirejczyk WM, Conran RM, Stocker JT. Pulmonary inflammatory pseudotumor: radiologic features. Radiology 206:511–5181998.


26. Pettinato G, Manivel JC, De Rosa N, Dehner LP. Inflammatory myofibroblastic tumor (plasma cell granuloma): clinicopathologic study of 20 cases with immunohistochemical and ultrastructural observations. Am J Clin Pathol 94:538–5461990.


27. Thunnissen FB, Arends JW, Buchholtz RT, ten Velde G. Fine needle aspiration cytology of inflammatory pseudotumor of the lung (plasma cell granuloma). Report of four cases. Acta Cytol 33:917–9211989.

28. Ishida T, Oka T, Nishino T, Tateishi M, Mitsudomi T, Sugimachi K. Inflammatory pseudotumor of the lung in adults: radiographic and clinicopathological analysis. Ann Thorac Surg 48:90–951989.


29. Arakawa H, Nakajima Y, Kurihara Y, Niimi H, Ishikawa T. CT-guided transthoracic needle biopsy: a comparison between automated biopsy gun and fine needle aspiration. Clin Radiol 51:503–5061996.





 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print



