 |
 |
| Korean J Intern Med > Volume 14(1); 1999 > Article |
|
Abstract
Leiomyosarcoma is a rare tumor that originates in the smooth muscle, usually in the gastrointestinal tract, the retroperitoneum and the genitourinary tract. The omentum has been rarely reported as a primary site of occurrence with leiomyosarcoma. A 72 year-old woman, with palpable mass on the left upper quadrant of abdomen and weight loss, was admitted to St. Paul’s Hospital. Abdominal CT scan showed a 12×8×8 cm-sized cystic mass in the left upper quadrant of the abdomen. Endoscopic ultrasonography showed a large cystic mass between the stomach and the liver, which was 1.6 cm length in wall thickness. Laparotomy and resection of the mass was performed. A 12×8×8 cm-sized mass, originated from the lesser omentum, was discovered near the lesser curvature of the stomach. Microscopic examination revealed spindle-shaped cells with 7–8 mitoses per high power field. She was diagnosed as primary leiomyosarcoma originated from the lesser omentum.
Leiomyosarcomas are uncommon malignant tumors that originate in smooth muscle, usually in the gastrointestinal tract, the retroperitoneum and the genitourinary tract1). Metastatic tumors in the omentum are not uncommon, but primary omental tumors are reported to be rare and usually malignant2,3).
There were a few cases of primary omental leiomyosarcoma reported in the literature4). Mostly, these cases originated from the greater omentum. The case with leiomyosarcoma originated from the lesser omentum was extremely rare.
This report describes a rare case of primary leiomyosarcoma of the lesser omentum with a review of the literature.
A 72-year-old female was admitted to our hospital with palpable mass in the left upper quadrant of the abdomen and weight loss. The patient discovered the mass a month previously. She had no prior history of medical and surgical diseases. Her family was healthy with no genetic diseases. The patient denied any symptoms such as nausea, vomiting, diarrhea, constipation, melena, hematochezia, jaundice, hematemesis, flushing and palpitation.
On physical examination, blood pressure was 140/80 mmHg, pulse rate was 74/min, respiration rate was 20/min and the body temperature was 36°C. A hard, movable, man-fist-sized mass was palpated on the left upper quadrant of the abdomen.
The hemoglobin was 10.1 g/dl and the hematocrit was 31%. The white cell count was 8,600/mm3 with 60% polymorphonuclear cells. The platelet count was 220,000/mm3. The serum sodium was 141 mEq/L, potassium 4.3 mEq/L, and serum amylase was 121 IU/L. The protein was 6.7 g/dl, albumin 4.1 g/dl, cholesterol 189 mg/dl, total bilirubin 0.5 mg/dl, alkaline phosphatase 125 IU/L, AST 16 IU/L and ALT was 9 IU/L. Urinalysis did not reveal any evidence of abnormalities.
X-ray of the chest and simple abdomen showed normal. Abdominal CT scan revealed a 12×8×8 cm-sized heterogeneous cystic mass in the left upper quadrant of the abdomen that had irregularly enhanced the solid portion and the large area of the central cystic portion. There was marked displacement of the stomach and omental vessels to the posterior and inferior side, due to compression by the mass (Fig. 1).
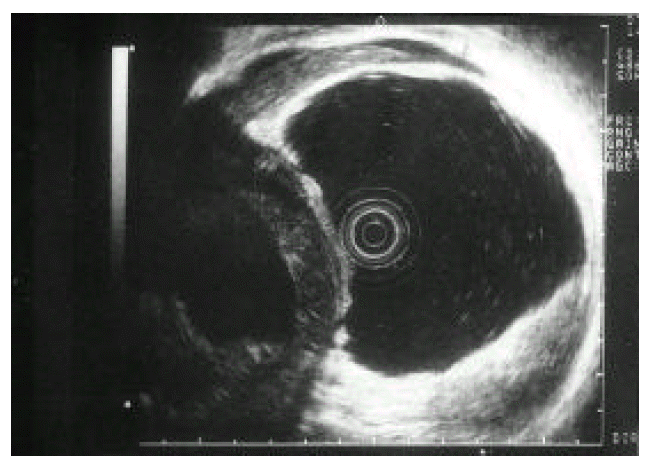
Endoscopic ultrasonography showed a large cystic mass near the stomach and liver, which was 1.6 cm length in wall thickness. The wall echo of the stomach was normal (Fig. 2).
Laparotomy and excision of the mass was performed. A pale gray-colored, lobulated 12×8×8 cm-sized mass, which originated from the lesser omentum, was discovered adjacent to the lesser curvature side of the high body of the stomach. The mass compressed the liver and displaced the stomach to the left lateral side. When the mass was bisected, it was mainly composed of cyst and hemorrhagic materials. But there was a small area of solid component, which was accompanied with focal hemorrhage and necrosis (Fig. 3 and 4).
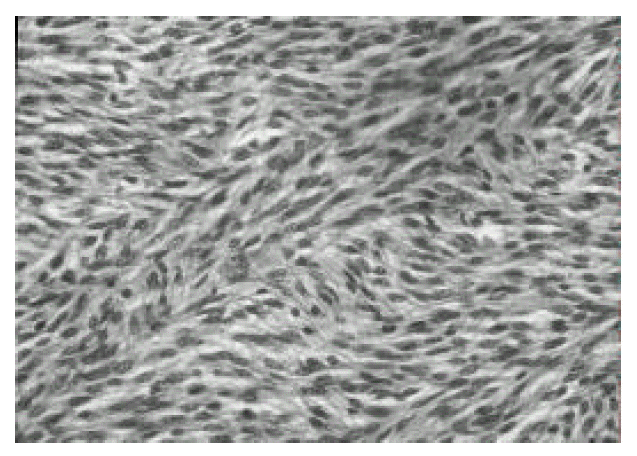
Microscopic examination showed spindle-shaped cells with 7–8 mitoses per 10 high power field(Fig. 5). She was diagnosed as rarely occurring leiomyosarcoma originating from the lesser omentum.
Even though the omentum is composed mostly of adipose tissue, tumors of smooth muscle origin are more common than those of adipose tissue origin. It is surmised that smooth muscle tumors arise from mesodermal elements present in the blood vessels, fibrous tissues and the nerves of the omentum5). We recently experienced this rarely occurring leiomyosarcoma originating from the lesser omentum in a 72-year-old woman.
In Dixon’s histologic diagnosis of omental tumors, nearly 33% were sarcomatous in nature, while only 18% were of adipose origin. They may affect any age group but occur most commonly in the middle-aged. The most common symptom of omental leiomyosarcoma is abdominal mass, distension or pain; ascites has also been reported4).
CT scan is useful in diagnosing the tumor. In McLeod’s study of leiomyosarcomas,6) 89 of 118 (75.4%) had abnormal findings on body CT scan, as most were large by the time of diagnosis. Barium enema may also be a useful diagnostic tool. A mass that displaces the stomach superiorly and posteriorly and the transverse colon inferiorly and anteriorly is pathognomonic6). Angiography may also be performed, although the hypervascularity of the tumor was the only identifying finding, as presented on Granmayeh’s series7).
Leiomyosarcomas of the omentum were reported to be mitotically active, showing one to four mitoses per 10 high power field in one series and a more higher rate in the other series8). The present case showed active mitoses, accounting for 7–8 mitoses per 10 high power fields.
Laparotomy is the procedure of choice for diagnosis, treatment and detection of possible metastases of the omental leiomyosarcoma. Especially, in the case with a primary omental tumor, a total omentectomy, including the mass, should be recommended because of the possible presence of microscopic metastases9). Before resection of the omental tumor, a careful search for any possible primary site in another organ is essential10). The long-term outcome of patients with omental leiomyosarcomas is unknown. Early reports, such as those by Sanes and Kenny11) and Levy and Pund,12) showed poor outcomes with a high post-operative death rate. No trials have been performed using chemotherapy or radiation therapy, but these do not seem to be efficacious based on other sarcomas’ durable response to these modalities13).
Fig. 1.
Abdominal CT scan showed a 12×8×8 cm-sized heterogeneous cystic mass in the left upper quadrant of the abdomen. There was marked displacement of the stomach to posterior and inferior side.

Fig. 2.
Endoscopic ultrasonography showed a large cystic mass near the stomach and liver. The wall echo of the stomach near the mass was normal.
REFERENCES
1. McLeod AJ, Zornoza J, Shirkhoda A. Leiomyosarcoma: Computed tomographic findings. Radiology 152:133–361984.


2. Ackerman LV. Atlas of Tumor Pathology; Sect VI, Facs 23 & 24. Washington, DC: Armed Forces Institute of Pathology, 1954.
3. Weinberger HA, Ahmed MS. Mesenchymal solid tumors of the omentum and mesentery: report of four cases. Surgery 82:754–591977.

4. Dixon AY, Reed JS, Dow N, Lee SH. Primary omental leiomyosarcoma masquerading as hemorrhagic ascites. Hum Pathol 15:233–371984.


5. Tanimura A, Cho T, Nohara M, et al. Primary leiomyosarcoma of the omentum. Kurume Med J 27:101–051980.


6. Huckman MS, Fisher MS. Roentgenographic signs of tumors of the greater omentum. Cancer 33:1526–301974.


7. Granmayeh M, Jonsson K, McFarland W, Wallace S. Angiography of abdominal leiomyosarcoma. AJR 130:725–301978.


8. Hashimoto H, Tsuneyoshi M, Enjoji M. Malignant smooth muscle tumors of the retroperitoneum and mesentery: A clinicopathologic analysis of 44 cases. J Surg Oncol 28:177–861985.


9. Stavorovsky M, Morag B, Starvorovsky H, Papo J. Smooth muscle tumors of the alimentary tract. J Surg Oncol 22:109–1141983.


10. Elfving G, Hastbacka J. Primary solid tumors of the greater omentum. Acta Chir Scand 130:603–101965.

11. Sanes S, Kenny SE. Primary sarcoma of great omentum. Am J Cancer 21:795–8041934.
12. Levy JH, Pund ER. Primary sarcoma of omentum: report of two cases. Am J Cancer 40:219–261940.
-
METRICS

- Related articles
-
A case of papillary fibroelastoma in the left ventricle2013 January;28(1)
A Case of Granular Cell Tumor of the Trachea2007 June;22(2)
A Case of Primary Plasmacytoma of Lymph Nodes2005 June;20(2)
A Case of Extramedullary Plasmacytoma Arising from the Posterior Mediastinum2005 June;20(2)





 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print


