 |
 |
| Korean J Intern Med > Volume 35(1); 2020 > Article |
|
Abstract
Background/Aims
Methods
Results
Supplementary Materials
Supplementary Figure 1.
Supplementary Figure 2.
Acknowledgments
Figure 1.

Figure 2.
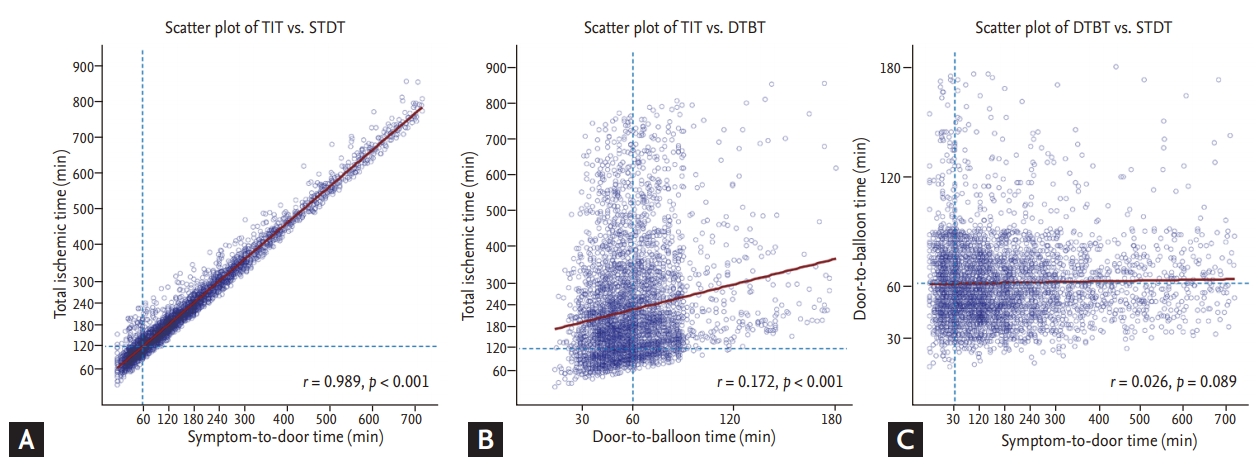
Figure 3.
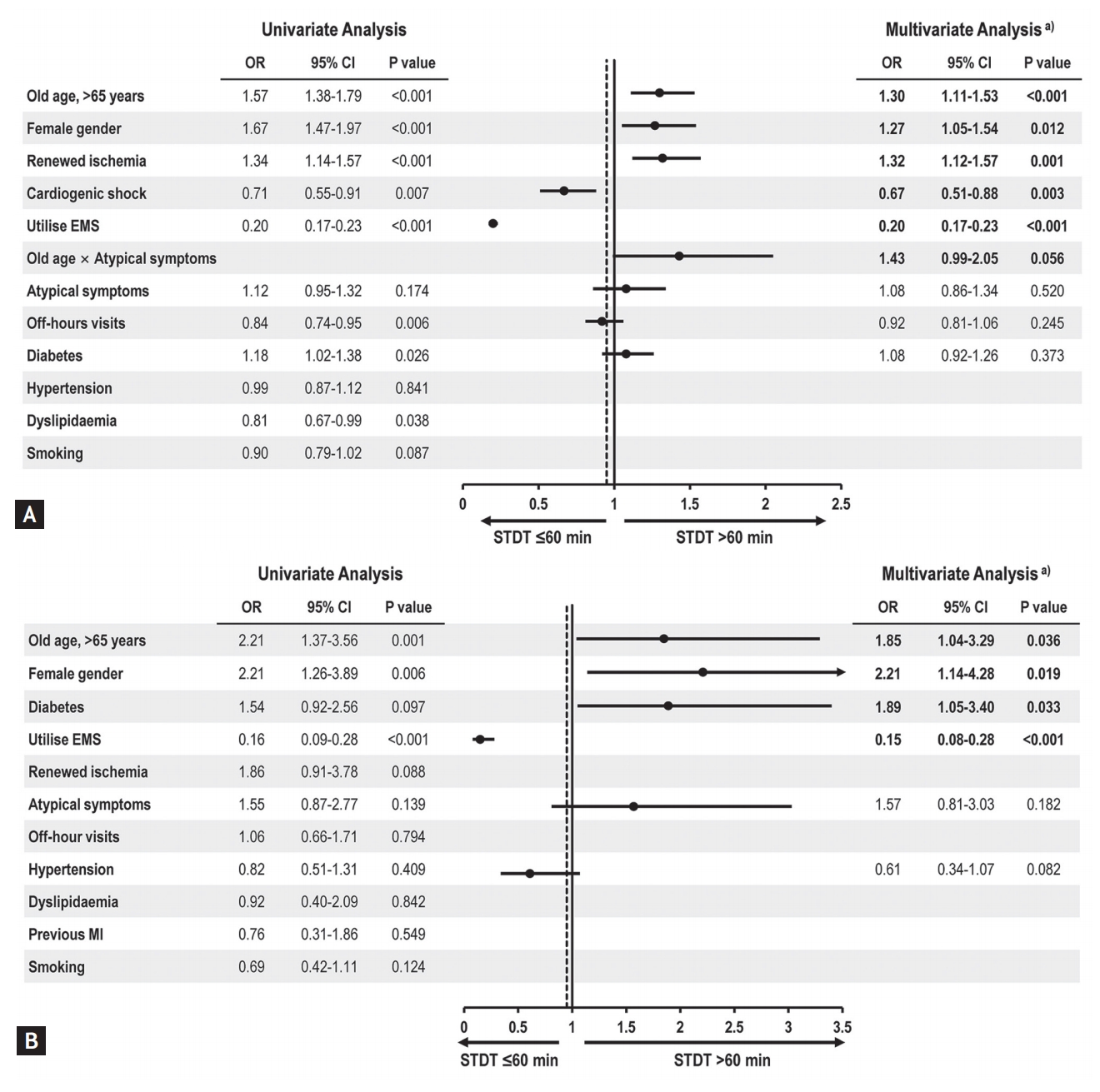
Figure 4.
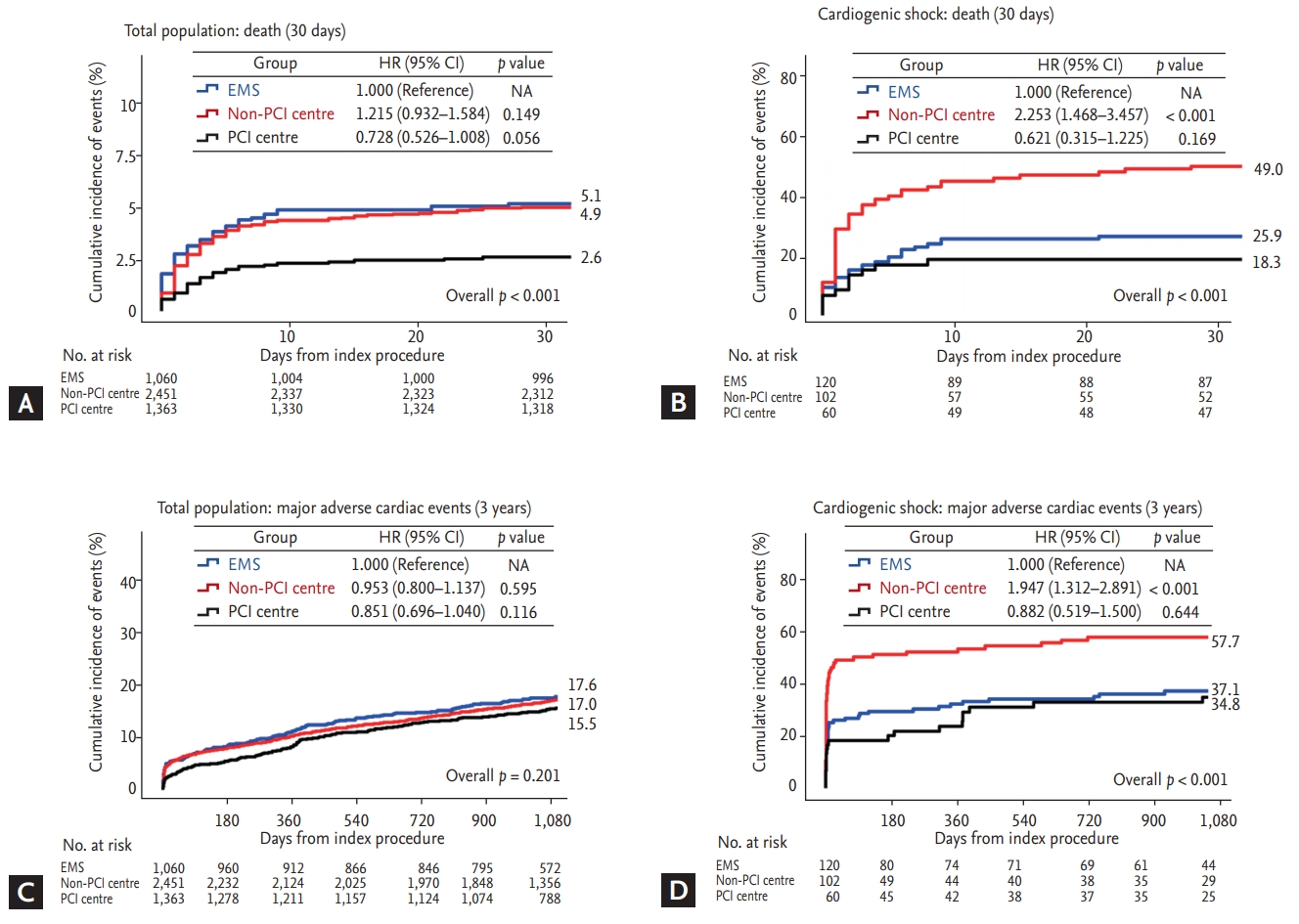
Figure 5.
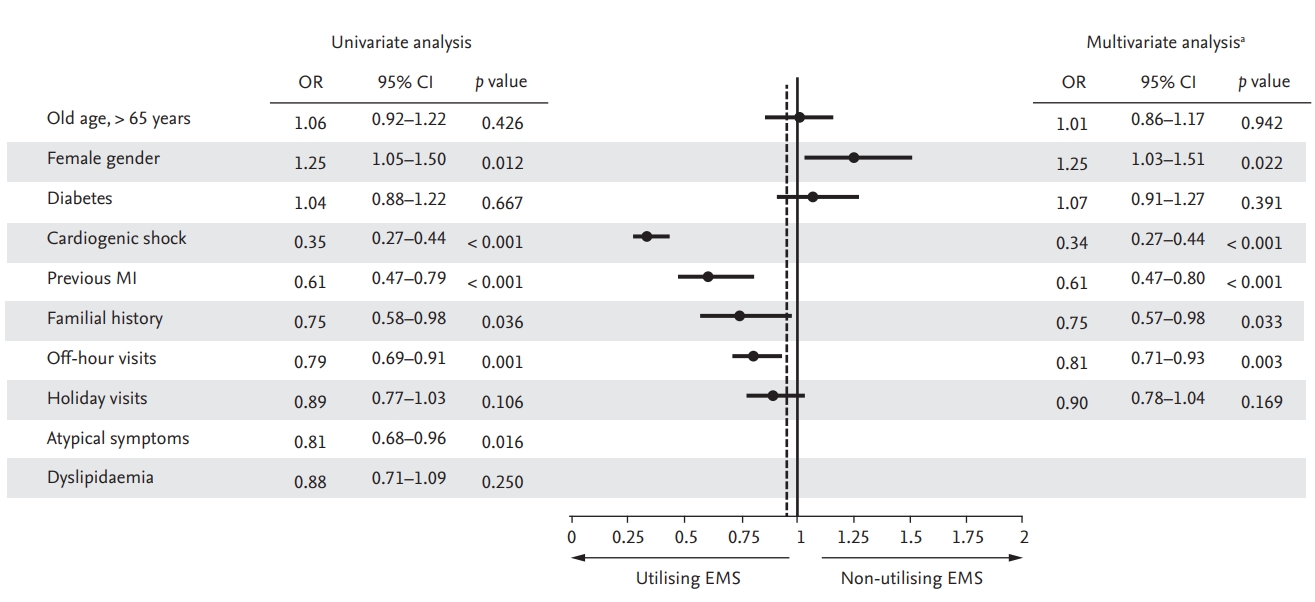
Table 1.
| Characteristic | Total (n = 4,874) |
All patients (n = 4,874) |
Cardiogenic shock (n = 282) |
||||
|---|---|---|---|---|---|---|---|
| STDT ≤ 60 min (n = 1,386) | STDT > 60 min (n = 3,488) | p value | STDT ≤ 60 min (n = 130) | STDT > 60 min (n = 152) | p value | ||
| Age, yr | 62.1 ± 12.6 | 59.9 ± 12.3 | 63.0 ± 12.7 | < 0.001 | 63.0 ± 12.5 | 68.3 ± 13.0 | 0.001 |
| Age > 65 yr | 1,983 (40.7) | 458 (33.0) | 1,525 (43.7) | < 0.001 | 55 (42.3) | 94 (61.8) | 0.002 |
| Male sex | 3,900 (80.0) | 1,184 (85.4) | 2,716 (77.9) | < 0.001 | 107 (82.3) | 103 (67.8) | 0.008 |
| Holiday visits | 1,542 (31.6) | 449 (32.4) | 1,093 (31.3) | 0.494 | 47 (36.2) | 48 (31.6) | 0.494 |
| Off-hour visitsa | 1,951 (40.0) | 597 (43.1) | 1,354 (38.8) | 0.007 | 57 (43.8) | 69 (45.4) | 0.888 |
| Atypical symptoms | 888 (18.2) | 236 (17.0) | 652 (18.7) | 0.008 | 23 (17.7) | 38 (25.0) | 0.180 |
| Renewed ischemia | 1,012 (20.8) | 242 (17.5) | 720 (22.1) | < 0.001 | 13 (10.0) | 26 (17.1) | 0.121 |
| Utilised EMS | 1,060 (21.7) | 555 (44.0) | 505 (14.5) | < 0.001 | 79 (60.8) | 41 (27.0) | < 0.001 |
| Non-PCI centre | 2,451 (50.3) | 327 (23.6) | 2,124 (60.9) | < 0.001 | 20 (15.4) | 82 (53.9) | < 0.001 |
| STDT, min | 164.4 ± 146.8 (120 [60–220]) | 39.3 ± 16.4 (39 [29–56]) | 214.1 ± 146.0 (169 [111–273]) | < 0.001 | 36.1 ± 16.8 (35 [24–52]) | 205.5 ± 146.5 (151 [105–247]) | < 0.001 |
| DTBT, min | 60.8 ± 22.9 (58 [45–71]) | 62.9 ± 24.3 (60 [46–74]) | 59.9 ± 22.2 (57 [45–70]) | < 0.001 | 64.9 ± 27.3 (61 [47–78]) | 64.3 ± 28.0 (59 [46–76]) | 0.865 |
| ≤ 60 | 2,755 (56.5) | 719 (51.9) | 2,036 (58.4) | < 0.001 | 63 (48.5) | 83 (54.6) | 0.363 |
| ≤ 90 | 4,573 (93.8) | 1,279 (92.3) | 3,294 (94.4) | 0.006 | 117 (90.0) | 135 (88.8) | 0.898 |
| TIT, min | 225.1 ± 149.1 (178 [120–282]) | 102.2 ± 29.3 (100 [83–118]) | 274.0 ± 149.5 (224 [167–335]) | < 0.001 | 101.0 ± 32.4 (95 [80–117]) | 269.8 ± 152.7 (218 [165–313]) | < 0.001 |
| ≤ 120 | 1,242 (25.5) | 1,078 (77.8) | 164 (4.7) | < 0.001 | 100 (76.9) | 10 (6.6) | < 0.001 |
| ≤ 180 | 2,487 (51.0) | 1,358 (98.0) | 1,129 (32.4) | < 0.001 | 125 (96.2) | 51 (33.6) | < 0.001 |
| SBP, mmHg | 125.1 ± 32.7 | 121.3 ± 36.6 | 126.6 ± 30.9 | < 0.001 | 55.0 ± 34.5 | 60.1 ± 30.6 | 0.197 |
| Heart rate, /min | 75.7 ± 20.5 | 73.9 ± 22.9 | 76.5 ± 19.4 | < 0.001 | 57.9 ± 37.0 | 66.3 ± 34.7 | 0.051 |
| GRACE score | 123 ([98–149]) | 118 ([94–146]) | 124 ([100–151]) | < 0.001 | 157 ([139–177]) | 163 ([144–190]) | 0.020 |
| Cardiogenic shock | 282 (5.8) | 130 (9.4) | 152 (4.4) | < 0.001 | - | - | - |
| Hypertension | 2,229 (45.7) | 637 (46.0) | 1,592 (45.6) | 0.866 | 68 (52.3) | 72 (47.4) | 0.479 |
| Diabetes | 1,160 (23.8) | 300 (21.6) | 860 (24.7) | 0.029 | 35 (26.9) | 55 (36.2) | 0.125 |
| Dyslipidaemia | 523 (10.7) | 169 (12.2) | 354 (10.1) | 0.042 | 12 (9.2) | 13 (8.6) | 1.000 |
| Smoking | 2,223 (45.6) | 659 (47.5) | 1,564 (44.8) | 0.093 | 57 (43.8) | 53 (34.9) | 0.156 |
| Familial history | 309 (6.3) | 108 (7.8) | 201 (5.8) | 0.011 | 7 (5.4) | 4 (2.6) | 0.378 |
| Previous MI | 283 (5.8) | 97 (7.0) | 186 (5.3) | 0.140 | 11 (8.5) | 10 (6.6) | 0.709 |
| History of stroke | 220 (4.5) | 53 (3.8) | 167 (4.8) | 0.166 | 5 (3.8) | 7 (4.6) | 0.985 |
| LVEF, % | 50.7 ± 10.2 | 52.4 ± 9.9 | 50.0 ± 10.2 | < 0.001 | 50.0 ± 11.9 | 43.7 ± 11.9 | < 0.001 |
| CK-MB, ng/mL | 174.0 ± 185.4 | 157.0 ± 162.0 | 180.7 ± 193.6 | < 0.001 | 215.2 ± 250.9 | 232.1 ± 311.5 | 0.615 |
| Troponin-I, ng/mL | 77.7 ± 127.0 | 69.6 ± 152.3 | 80.9 ± 115.4 | 0.023 | 82.9 ± 166.8 | 109.5 ± 148.6 | 0.207 |
| Creatinine, g/dL | 1.0 ± 0.7 | 1.1 ± 0.8 | 1.0 ± 0.7 | 0.049 | 1.2 ± 0.4 | 1.3 ± 0.6 | 0.008 |
Values are presented as mean ± SD, number (%), or median (interquartile range).
STDT, symptom-to-door time; EMS, emergency medical service; PCI, percutaneous coronary intervention; DTBT, door-toballoon time; TIT, total ischemic time; SBP, systolic blood pressure; GRACE, Global Registry of Acute Coronary Events; MI, myocardial infarction; LVEF, left ventricular ejection fraction; CK-MB, creatine kinase-myocardial band.
Table 2.
| Characteristic | Total (n = 4,874) |
All population (n = 4,874) |
Cardiogenic shock (n = 282) |
||||
|---|---|---|---|---|---|---|---|
| STDT ≤ 60 min (n = 1,386) | STDT > 60 min (n = 3,488) | p value | STDT ≤ 60 min (n = 130) | STDT > 60 min (n = 152) | p value | ||
| Aspirin | 4,861 (99.7) | 1,379 (99.5) | 3,482 (99.8) | 0.084 | 124 (95.4) | 149 (98.0) | 0.358 |
| Clopidogrel | 3,074 (63.1) | 834 (60.2) | 2,240 (64.2) | 0.009 | 70 (53.8) | 85 (55.9) | 0.819 |
| Ticagrelor | 1,043 (21.4) | 325 (23.4) | 718 (20.6) | 0.031 | 25 (19.2) | 25 (16.4) | 0.650 |
| Prasugrel | 607 (12.5) | 182 (13.1) | 425 (12.2) | 0.393 | 15 (11.5) | 10 (6.6) | 0.211 |
| Beta-blockers | 4,155 (85.2) | 1,197 (86.4) | 2,958 (84.8) | 0.180 | 82 (63.1) | 73 (48.0) | 0.016 |
| ACE inhibitors | 2,571 (52.7) | 733 (52.9) | 1,838 (52.7) | 0.929 | 52 (40.0) | 45 (29.6) | 0.088 |
| ARBs | 1,305 (26.8) | 348 (25.1) | 957 (27.4) | 0.105 | 23 (17.7) | 26 (17.1) | 1.000 |
| Statins | 4,464 (91.6) | 1,272 (91.8) | 3,192 (91.5) | 0.811 | 86 (66.2) | 89 (58.6) | 0.235 |
| GP IIb/IIIa inhibitor | 1,076 (22.1) | 309 (22.3) | 767 (22.0) | 0.847 | 42 (32.3) | 44 (28.9) | 0.630 |
| Multi-vessel diseasedz. | 2,265 (46.5) | 638 (46.0) | 1,627 (46.6) | 0.722 | 76 (58.5) | 95 (62.5) | 0.569 |
| LAD related diseasedz. | 2,456 (50.4) | 713 (51.4) | 1,743 (50.0) | 0.371 | 40 (30.8) | 55 (36.2) | 0.405 |
| Lesion type B1/B2 | 2,224 (45.6) | 612 (44.2) | 1,612 (46.2) | 0.204 | 58 (44.6) | 62 (40.8) | 0.598 |
| Lesion type C | 2,609 (53.5) | 754 (54.4) | 1,855 (53.2) | 0.461 | 69 (53.1) | 89 (58.6) | 0.422 |
| Thrombus aspiration | 1,854 (38.0) | 515 (37.2) | 1,339 (38.4) | 0.444 | 41 (31.5) | 56 (36.8) | 0.419 |
| Using BMS | 131 (2.7) | 38 (2.7) | 93 (2.7) | 0.961 | 9 (6.9) | 11 (7.2) | 1.000 |
| IABP | 242 (5.0) | 71 (5.1) | 171 (4.9) | 0.806 | 27 (20.8) | 47 (30.9) | 0.073 |
| ECMO | 75 (1.5) | 27 (1.9) | 48 (1.4) | 0.182 | 18 (13.8) | 19 (12.5) | 0.875 |
| Complete revascularisationa | 4,809 (98.7) | 1,369 (98.8) | 3,440 (98.6) | 0.568 | 123 (94.6) | 144 (94.7) | 0.748 |
| Hospital death | 207 (4.2) | 58 (4.2) | 149 (4.3) | 0.954 | 33 (25.4) | 60 (39.5) | 0.017 |
| Cardiac death | 187 (3.8) | 54 (3.9) | 133 (3.8) | 0.957 | 32 (24.6) | 55 (36.2) | 0.049 |
| Non-cardiac death | 20 (0.4) | 4 (0.3) | 16 (0.5) | 0.555 | 1 (0.8) | 5 (3.3) | 0.295 |
| Newly developed HF | 172 (3.5) | 47 (3.4) | 125 (3.6) | 0.808 | 9 (6.9) | 21 (13.8) | 0.093 |
| VT/VF | 395 (8.1) | 134 (9.7) | 261 (7.5) | 0.014 | 41 (31.5) | 54 (35.5) | 0.562 |
| TIMI major bleeding | 100 (2.1) | 30 (2.2) | 70 (2.0) | 0.812 | 15 (11.5) | 14 (9.2) | 0.656 |
| TIMI minor bleeding | 150 (3.1) | 38 (2.7) | 112 (3.2) | 0.445 | 9 (6.9) | 10 (6.6) | 1.000 |
Values are presented as number (%).
STDT, symptom-to-door time; ACE, angiotensin-converting enzyme; ARB, angiotensin II receptor blocker; GP, glycoprotein; dz, disease; LAD, left anterior descending artery; BMS, bare metal stent; IABP, intra-aortic balloon pump; ECMO, extracorporeal membrane oxygenation; HF, heart failure; VT/VF, ventricular tachycardia/ventricular fibrillation; TIMI, thrombolysis in myocardial infarction.
Table 3.
Values are presented as number (%), mean ± SD, or median (interquartile range).
EMS, emergency medical service; PCI, percutaneous coronary intervention; ANOVA, analysis of variance; STDT, symptom-to-door time; DTBT, door-to-balloon time; TIT, total ischemic time; SBP, systolic blood pressure; GRACE, Global Registry of Acute Coronary Events; MI, myocardial infarction.
REFERENCES
- TOOLS
-
METRICS

- Related articles
-
Current status of acute myocardial infarction in Korea2019 January;34(1)



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Supplement 1
Supplement 1 Print
Print


