INTRODUCTION
EDTA is commonly used as an anticoagulant for blood cell counts, but it may agglutinate the platelets in some patients. This EDTA-induced aggregation of platelets leads to pseudothrombocytopenia, so-called EDTA-dependent PTCP1). EDTA-dependent PTCP can be recognized by the presence of platelet clumps in the peripheral smear of blood anticoagulated with EDTA. The aggregation of platelets in EDTA-dependent PTCP usually is prevented by other anticoagulants, such as sodium citrate or heparin2). In addition, the collection and examination of blood at 37┬░C also prevent the aggregation of platelets3). But, in some cases, platelet aggregation is not completely prevented by these methods for counting the platelets3,4). Recently, it has been suggested that the supplementation of aminoglycosides to anticoagulant is a useful method for obtaining accurate platelet count in EDTA-dependent PTCP subject1,4). To the best of our knowledge, this is the first report in Korea of EDTA-dependent PTCP confirmed by the supplementation of kanamycin to anticoagulant in a healthy subject.
CASE
A 53-year-old woman was referred to our hospital because of thrombocytopenia detected incidentally. Findings from the general practitionerŌĆÖs laboratory were platelet 19,000/mm3, WBC 4,300/mm3, Hb 9.4 g/dL and Hct 28.6%. The patient did not use alcohol or any medication. She denied drug and food allergy. There was no family history of hemorrhagic disorders. There was no history of ecchymoses, recent melena, metrorrhagia or weight loss. Neither signs of hemorrhagic diathesis, such as bruises, nor lymphadenopathy were detected on the physical examination.
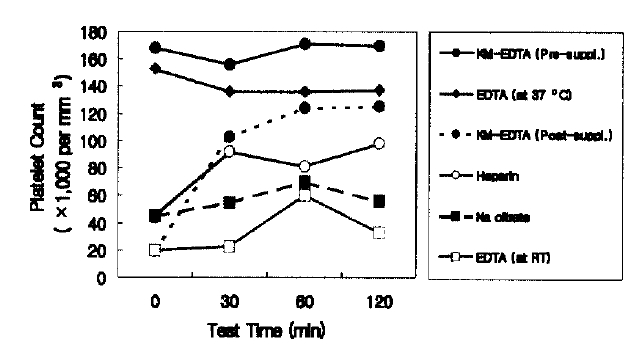
The patientŌĆÖs platelet count in our laboratory was 20,000/mm3 but the aggregation of platelets was recognized by microscopic examination of the peripheral blood smear. We suspected that this low platelet count was due to EDTA-induced aggregation of platelets. So, we measured the platelet count of the patientŌĆÖs blood samples anticoagulated with sodium citrate and heparin. However, the platelet count with sodium citrate and heparin was 45,000/mm3 and 44,000/mm3, respectively. In microscopic examination of the blood smears, the aggeregation of platelets was detected in both blood samples. Anti-platelet antibodies and anti- cardiolipin antibodies were not detectable. To confirm the diagnosis of EDTA-dependent PTCP, we measured the platelet count and examined the blood cell morphology with the EDTA blood supplemented with kanamycin. For the kanamycin-supplemented anticoagulation, 20 mg of kanamycin were added to 2 mg of potassium EDTA either before or 30 min after blood withdrawal. EDTA blood supplemented with kanamycin and blood samples anticoagulated with other anticoagulants, such as EDTA, sodium citrate and heparin, were collected and incubated at room temperature. EDTA-anticoagulated blood was collected and incubated also at 37┬░C. Then, we measured the platelet count and examined the blood cell morphology in all the above-mentioned samples immediately after blood withdrawal and after 30 min, 60 min and 120 min of incubation at room temperature or at 37┬░C (Figure 1). Sodium citrate and heparin failed in preventing the aggregation of platelets in this case. The collection and examination of a sample anticoagulated with EDTA at 37┬░C and the addition of kanamycin to anticoagulant after blood withdrawal only partially prevented the clumping anticoagulant before blood withdrawal resulted in a complete prevention of platelet aggregation (Figure 2A, 2B).
We confirmed EDTA-dependent PTCP because the aggregation of platelets on microscopic evaluation was found in EDTA-anticoagulated blood samples without the addition of kanamycin, whereas thrombocytopenia and platelet clumping was not revealed in the sample supplemented with kanamycin.
DISCUSSION
EDTA-dependent PTCP is the phenomenon of a spurious low platelet count due to the appearance of antiplatelet autoantibodies that cause platelet clumping in blood anticoagulated with EDTA5,6). These antiplatelet antibodies, usually IgG or IgM, and rarely IgA, recognize platelet antigens on the platelet membrane modified by EDTA1,3,4,7). The platelet membrane glycoprotein complex IIb/IIIa might be involved in EDTA-dependent antibody reaction3). The GP lib fraction is normally hidden in GP IIb/IIIa complex, but becomes accessible to the cold antibody after dissociation of the glycoprotein complex due to the chelating effect of EDTA on calcium ions, which are associated with alterations in protein conformation caused by low temperature3,8,9).
A spurious low platelet count due to platelet aggregation in EDTA-dependent PTCP is of practical importance because the lack of recognition of this clinical entity may result in erroneous diagnosis and subsequent mismanagement of the patient1,10). So, the first step in any case of newly diagnosed thrombocytopenia is to rule out falsely low platelet counts resulting from cold reactive, EDTA-dependent antiplatelet autoantibodies6,11). The EDTA-dependent PTCP can be confirmed by microscopic evaluation of a peripheral blood smear for aggregation of platelets and difference in platelet counts between EDTA and other anticoagulants5,9,11). Anticoagulants, such as heparin and sodium citrate, are usually used for obtaining accurate platelet counts in EDTA-dependent PTCP patients2,12). But, as in this case, platelet clumpings may be observed also in a blood sample anticoagulated with sodium citrate and heparin3,13,14). Therefore, various methods for obtaining accurate platelet count in such PTCP patients have been suggested.
It has been suggested that the best and most rapid technique for obtaining accurate platelet counts in EDTA-dependent PTCP patients was to collect and examine EDTA-anticoagulated blood at 37┬░C3). However, as in this case, platelet clumpings will still be present in about 20% of these patients. In the cases that show clumping also at 37┬░C, the examination of blood anticoagulated with ammonium oxalate in a Bucker chamber was recommended for proving PTCP3). It has been demonstrated that platelets could be counted correctly by the addition of a high concentration of sodium fluoride (NaF) in EDTA-anticoagulated blood in the patients with EDTA- dependent PTCP13).
Sakurai et al. reported that the prior addition of aminoglycosides to anticoagulants completely prevented the aggregation of platelets in EDTA-dependent PTCP subjects although the mode of action is not known1). In addition, the supplementation of aminoglycosides to EDTA-anticoagulated samples after blood withdrawal induced dissociation of aggregated platelets in blood samples from patients with EDTA-dependent PTCP1,5,6). So, it has been suggested that the supplementation of aminoglycosides to samples from EDTA-dependent PTCP patients, either before or after blood withdrawal, is an easy and effective way to diagnose EDTA-dependent PTCP and accuratley evaluate the platelet count of PTCP patients1).
In this case, we examined whether platelet clumping was prevented by the use of sodium citrate and heparin as a anticoagulant, by the addition of kanamycin to EDTA-anticoagulated sample before and after blood withdrawal and by the collection and examination of EDTA-anticoagulated blood at 37┬░C. While sodium citrate and heparin failed in preventing pseudothrombocytopenia, the addition of kanamycin to EDTA-anticoagulated sample after blood withdrawal and the collection and examination of samples at 37┬░C only partially prevented the aggregation of platelets. But, pre-supplementation of kanamycin to EDTA before blood sampling resulted in a complete prevention of platelet aggregation and pseudothrombocytopenia.
The findings in this case are most consistent with those of Sakurai et al. that the prior addition of aminoglycosides to EDTA completely prevented the aggregation of platelets1). In conclusion, although the precise mechanism by which aminoglycosides prevent the aggregation of platelets is unknown, the pre-supplementation of aminoglycoside antibiotics such as kanamycin to EDTA before the sample withdrawal is an easy and effective method for obtaining accurate platelet counts in patients with EDTA-dependent PTCP.



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print





