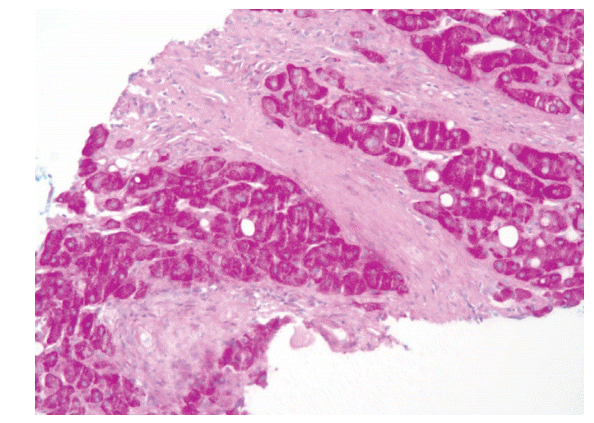
A 67-year-old man was referred to our emergency room for evaluation of exertional dyspnea and pretibial pitting edema of recent origin. At admission, neck vein engorgement was evident. Electrocardiography revealed a typical atrial flutter with 2:1 conduction; the serum cardiac enzyme levels were within normal limits. The laboratory findings were as follows: white blood cell 3,800/mm3 , hemoglobin 13.2 g/dL, platelets 89,000/mm3 , aspartate aminotransferase/alanine aminotransferase 68/48 U/L, protein/albumin 6.3/2.9 g/dL, bilirubin 2.4 mg/dL, prothrombin time 13.8 seconds, ferritin 250 ng/mL, ceruloplasmin 29 ng/dL, and α1-antitrypsin 115 mg/dL. Other serological markers, hepatitis B surface antigen, anti-hepatitis C virus, antinuclear antibody, anti-mitochondrial antibody, anti-smooth muscle antibody, and anti-liver kidney microsomal antibody, were all negative. Chest radiography revealed mild cardiomegaly with bilateral transudate pleural effusions. Chest computed tomography (CT) revealed pericardial calcification with eccentric wall thickening (Fig. 1A). Liver CT revealed a nodular hepatic contour with variable low-attenuation patterns often called a “nutmeg liver”, accompanied by regurgitation of contrast material into the intrahepatic veins, via the inferior vena cava (IVC), from the right atrium (Fig. 1B); and marked dilatation of the hepatic veins and IVC (Fig. 1C). Transthoracic echocardiography revealed moderate tricuspid regurgitation; the left ventricular ejection fraction was 40%. Liver histology (ultrasound-guided needle biopsy) revealed extensive bridging fibrosis, with minimal hepatic necroinflammation and steatosis (Fig. 2). Cardiac cirrhosis was confirmed based on the histological, radiological, and serological findings. After symptomatic improvement following conservative management that included dietary sodium restriction and diuretics, the patient is being followed regularly. Cardiac cirrhosis, an uncommon disease associated with chronic liver injury, is usually caused by long-standing right-sided heart failure associated with transmission of an elevated venous pressure, via the IVC and hepatic vein, to the liver sinusoids. Long-term hepatic congestion with relative ischemia can induce centrilobular necrosis and pericentral fibrosis, triggering extensive hepatic fibrosis and the formation of regenerative nodules.
 |
 |




 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print



