INTRODUCTION
Chronic obstructive pulmonary disease (COPD) is characterized by persistent airflow limitation that is usually progressive and associated with an enhanced chronic inflammatory response to noxious particles or gases in the airways and the lungs [
1]. COPD continues to be an important cause of morbidity, mortality, and healthcare costs worldwide [
2]. However, COPD is a highly underdiagnosed disease, with the diagnosis typically missed or delayed [
3]. The reported underdiagnosis rate of COPD has ranged from 72% to 93% [
4,
5,
6,
7].
The 4th Korean National Health and Nutrition Examination Survey (KNHANES), which was conducted from 2007 to 2009, reported that the prevalence of COPD, confirmed by spirometry, was 12.9%. According to the 4th KNHANES, 15.0% and 11.3% of subjects with severe airflow limitation (Global Initiative on Obstructive Lung Disease 3 and 4) were diagnosed with and treated for COPD, respectively [
8]. These data confirmed that COPD is also underdiagnosed and undertreated in Korea. Additionally, only 57% of currently treated COPD patients in Korea were aware of their precise current diagnostic status [
9]. Therefore, increased awareness about COPD is an important aspect of the diagnosis and treatment of this disease.
Cigarette smoking is the most common risk factor for COPD [
1], but few studies have been conducted about the attitudes toward COPD of smokers, the group at risk of developing COPD. The purpose of this study was to explore the awareness of and attitudes toward COPD among current smokers.
METHODS
Study design
This study used a cross-sectional design, and subjects were randomly selected from across Korea. Eligible subjects were current smokers aged 45 and older who smoked at least 10 packs per year. Telephone interviews were conducted by Gallup Korea, a specialized research company, with eligible subjects who agreed to participate in this survey.
Data collection and analysis
The telephone interviews were conducted using a structured questionnaire that addressed current health status, symptoms, awareness of COPD, and attitudes toward COPD. The average time to complete the full questionnaire was 20 minutes.
The questionnaire included five sections in addition to the section gathering demographic data. The first section addressed current health status and symptoms. The second focused on awareness of smoking-related respiratory diseases. The third examined being diagnosed with COPD by a physician or being treated for this condition. The fourth explored attitudes toward COPD after informing respondents about this disease. The last part addressed willingness to be treated for COPD.
All interview data were collected and managed anonymously. Descriptive statistics (e.g., frequencies and mean ┬▒ standard deviation were calculated for all qualitative and quantitative study variables, respectively.
DISCUSSION
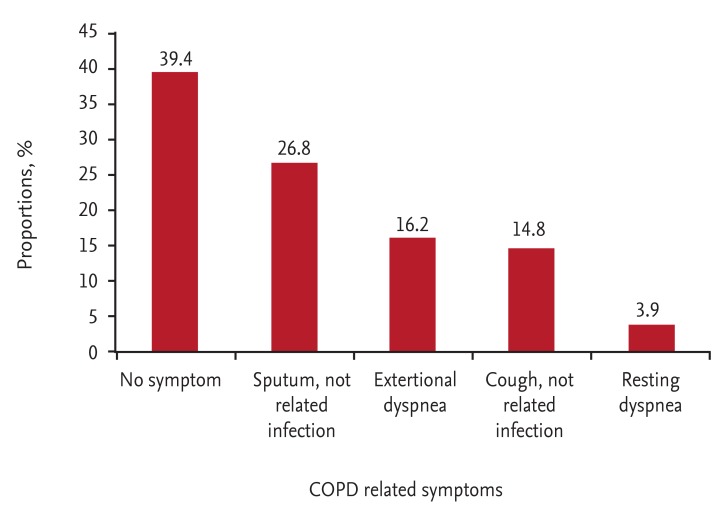
This study found that 60.6% of smokers had COPD-related symptoms and that about half of this group did not do anything about their symptoms. Only 13.5% of symptomatic subjects visited physicians due to their symptoms. Additionally, 45.4% of subjects perceived that they were in good health, and about 40% of heavy smokers endorsed this description of their health. This finding is consistent with previous results showing that COPD patients often regarded their disease as mild to moderate [
11] and that many COPD patients adapt their lifestyle to compensate for their deteriorating health [
12].
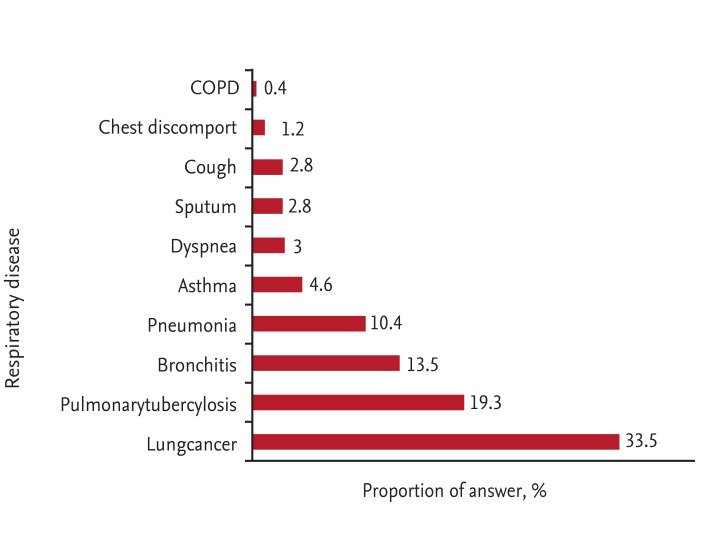
Most subjects in this study did not know that COPD is a respiratory disease, and only 0.4% of smokers were aware of this fact. This figure is considerably lower than that found by the CONOCEPOC study conducted in Spain, which reported that 17.0% of subjects spontaneously mentioned COPD as a respiratory disease [
13]. When a list of respiratory diseases, including COPD, was shown to subjects, this figure increased to 26.5%; however, more than 70% of smokers were unaware of COPD. Indeed, only 27.6% of symptomatic smokers were aware of COPD. Although spontaneous mentions of COPD tended to decrease with age in the CONOCEPOC study [
13], this study found no such difference according to age.
This study identified television as the most common source of information about COPD. A total of 66.2% of subjects received information about COPD from television, and only 18.0% received such information from physicians. These results differ from those of a previous study that found that physicians provided sufficient information about COPD to 88.0% of COPD patients [
9]. Thus, new strategies to provide information about COPD to the general population are needed.
COPD is a substantially underdiagnosed disorder, with the diagnosis typically missed or delayed until it is advanced [
3]. In this study, we found that 1.2% of current smokers had been diagnosed with and treated for COPD. Thus, the undiagnosed rate found in this study was higher than that of a previous study in Korea [
8] and other countries [
4,
5,
6,
7]. Although we did not ask if spirometry was used to diagnose COPD, these data reconfirmed that COPD is underdiagnosed and undertreated in Korea.
the current medications for COPD cannot change the natural course of this disease, patient education is an important aspect of COPD management. The most important topics for patient education are smoking cessation and basic information about COPD [
1]. It has also been recently reported that smoking cessation before 40 years of age reduces the risk of smoking-related death by about 90% [
14]. Therefore, smoking-cessation advice should be offered repeatedly, irrespective of the presence of COPD. Only 45.0% of subjects in this study reported an increased willingness to stop smoking after being informed of COPD, although 75.5% of this group were aware that COPD is caused by smoking. This low rate of increased willingness to stop smoking may also reflect the low level of awareness of COPD among smokers. It has also been reported that patients with less knowledge about COPD were more likely to have poor adherence to treatment [
15]. A personalized educational program is needed to enhance smoking-cessation willingness and clarify the relationship between COPD and smoking.
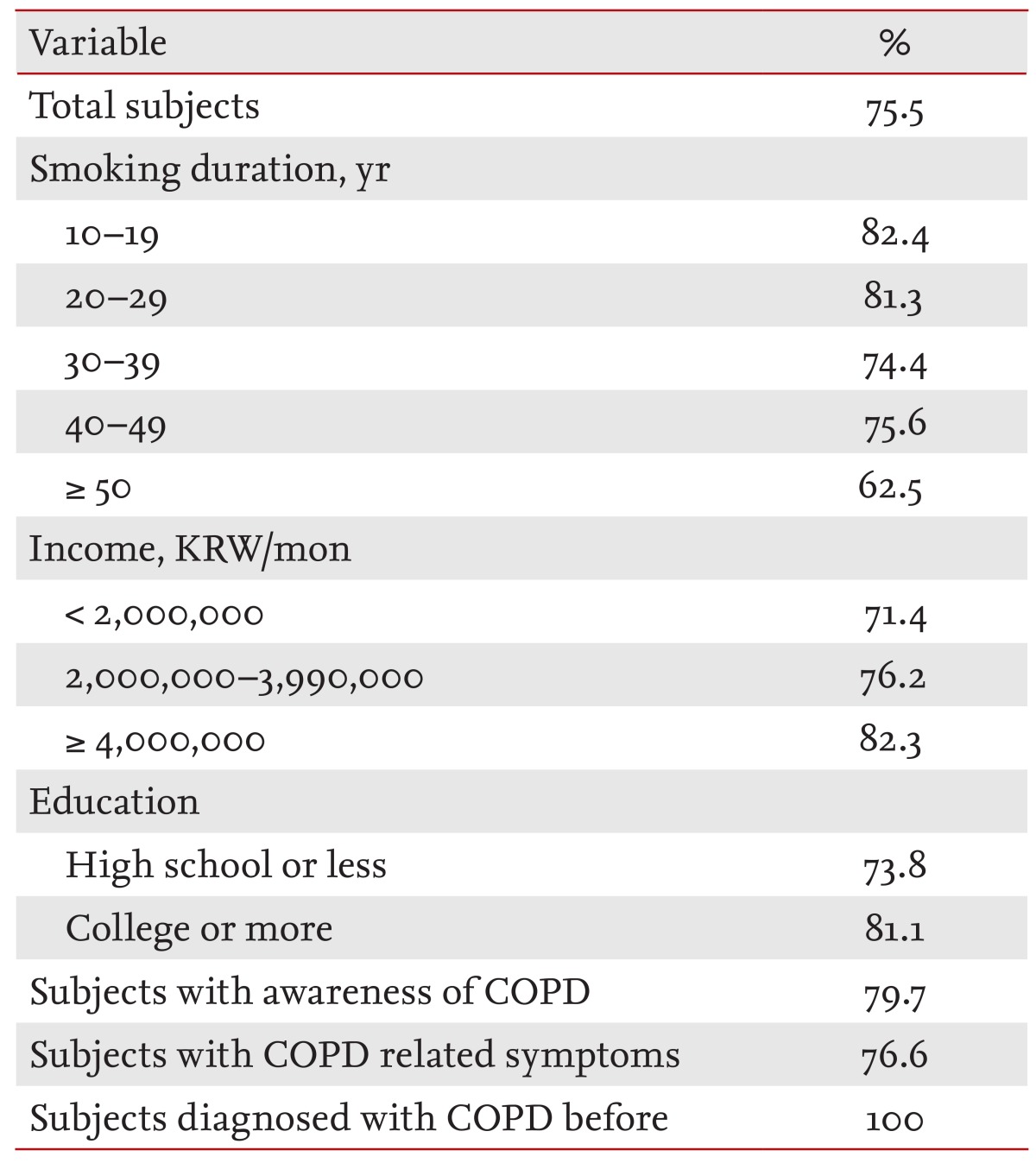
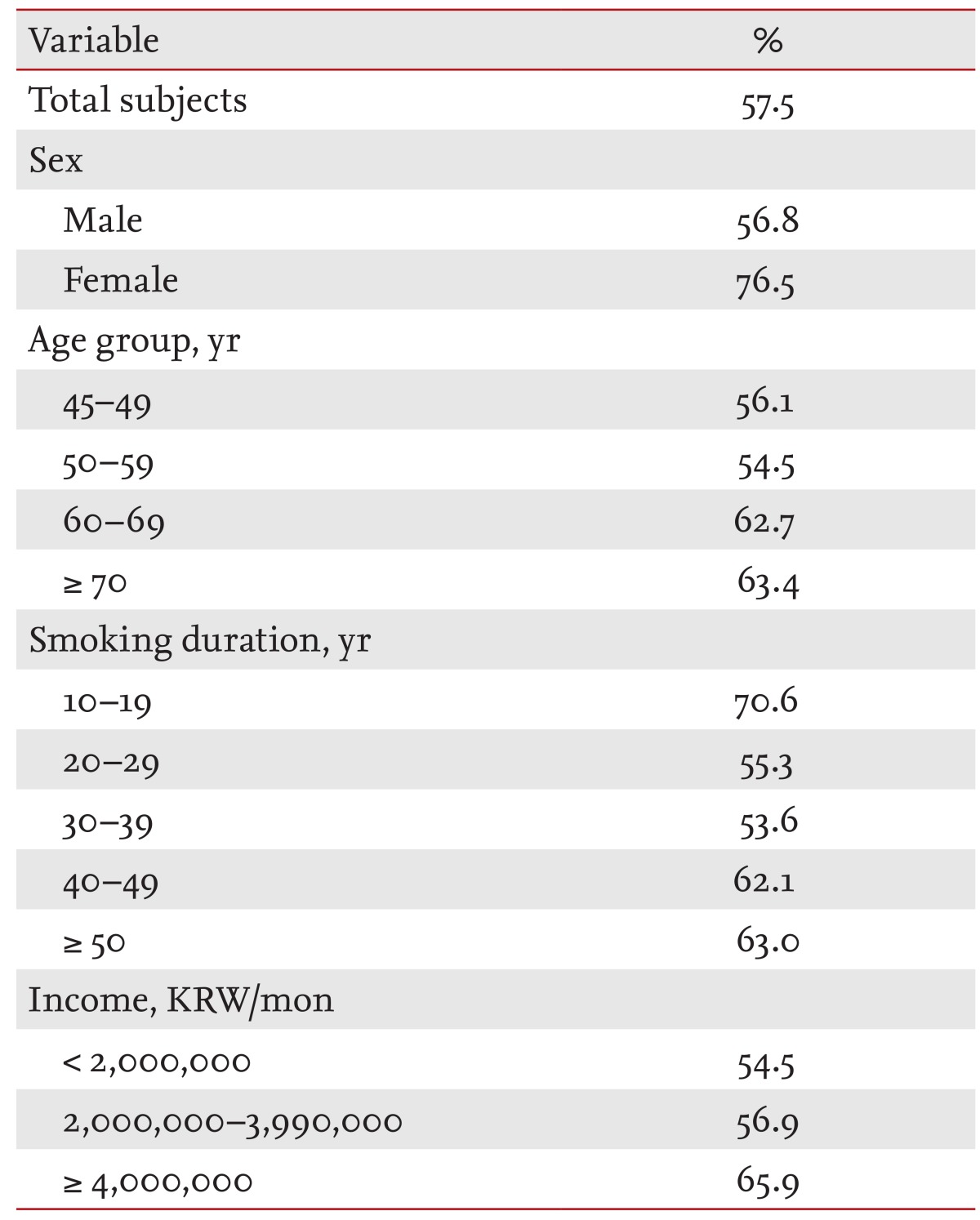
Only 57.5% of subjects responded that they would see a physician for medical treatment if they were diagnosed with COPD. Subjects who had smoked for 20 to 39 years expressed a more negative attitude toward COPD treatment. Thus, undertreatment continues to be a major problem in COPD management even though early diagnosis of COPD is possible. This may be another reason to enhance awareness of COPD. Although smoking is known to be the cause of COPD, only 75.5% of the subjects in this study knew that smoking caused COPD, and this figure varied according to group. A total of 81.1% and 82.3% of those with the most education and the highest income, respectively, were aware that smoking is the cause of COPD. However, these figures decreased to 73.8% and 71.4% among those with the least education and lowest income, respectively (
Table 3). This finding may explain why COPD is more common among those with low socioeconomic status [
16]. Thus, additional efforts will be needed to increase the awareness of COPD of this population.
In conclusion, we found that COPD is underdiagnosed and undertreated in smokers. Additionally, Korean smokers have low levels of awareness of COPD, and many smokers perceived their health to be good despite the presence of COPD-related symptoms. Smokers' attitudes toward COPD and smoking cessation varied according to their socioeconomic status. Additionally, television was the top source of information about COPD among smokers. As the subjects of this study were recruited from across Korea, we believe our results may represent the actual situation in this country. Therefore, continuous efforts to increase the awareness of COPD among smokers and to develop strategies fashioned according to socioeconomic status will be needed.





 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print





