 |
 |
| Korean J Intern Med > Volume 30(1); 2015 > Article |
|
Abstract
Background/Aims
Little is known about the efficacy of low-dose transdermal fentanyl (TDF) patches in opioid-naïve patients with moderate-to-severe cancer pain.
Methods
This study had an open-label, prospective design, and was conducted between April 2007 and February 2009 in seven tertiary cancer hospitals; 98 patients were enrolled. TDF was started using a low-dose formulation (12.5 ┬Ąg/hr), and the dose was adjusted according to the clinical situation of individual patients. Pain intensity, the TDF doses used, and adverse events (AEs) were monitored over 4 weeks. Data were analyzed using the intent-to-treat and per-protocol principles.
Results
Of the 98 patients enrolled, 64 (65%) completed the study. The median pain intensity decreased from 6.0 to 3.0 (p < 0.001) at the follow-up visit. The efficacy of low-dose TDF on pain relief was consistent across groups separated according to gender (p < 0.001), age (p < 0.001), metastasis (p < 0.001), previous treatment (p < 0.001), and baseline pain intensity (p < 0.001). The decrease in pain intensity was significantly greater in the severe group compared with the moderate group (mean ┬▒ SD, 5.10 ┬▒ 2.48 vs. 2.48 ┬▒ 1.56; p < 0.001). TDF dose (27.8 ┬Ąg/hr vs. 24.8 ┬Ąg/hr, p = 0.423) and the mean treatment time (7.5 days vs. 7.9 days, p = 0.740) required for pain control were not different between the two pain-intensity groups. Patients had AEs of only mild or moderate intensity; among these, nausea (38%) was the most common, followed by vomiting (22%) and somnolence (22%).
There is increasing evidence that pain control is related to not only the quality of life (QOL) but also the survival of cancer patients [1]. As such, appropriate pain management is essential to maximize patient outcomes. The World Health Organization (WHO) three-step treatment, from nonopioids, to weak and then strong opioids, has been considered the proper approach to cancer pain since its introduction [2]. Although this analgesic ladder approach has confirmed efficacy, a shift from weak to strong opioids is required in most patients [3,4]. However, there has been criticism that the WHO concept is oversimplified for cancer pain [5]. In other words, patients might suffer from unnecessary pain during the step-by-step opioid escalation. Therefore, various guidelines support the initial implementation of strong opioids including oxycodone, morphine, and fentanyl for significant cancer pain [6,7,8,9]. These guidelines recommend that patients with moderate-to-severe cancer pain should be managed using rapid titration and then converted to an equivalent dose of strong opioids in an extended-release formulation.
Transdermal fentanyl (TDF) is a widely used, popular opioid for cancer pain control. It is the first-line treatment for pain in many cancer patients due to its reduced metabolite formation [10] and usefulness in patients who have problems swallowing. The efficacy of TDF has been confirmed in varying intensities of cancer pain [11,12,13,14]. The commonly used formation of 25 ┬Ąg/hr TDF is a relatively high dose (a morphine equivalent daily dose [MEDD] of Ōēź 60 mg/day) in opioid-na├»ve patients; therefore, patients are likely to experience adverse events (AEs) [15]. Starting with low doses of TDF might be an alternative strategy to avoid this pitfall. However, limited data are available regarding low doses of TDF (12.5 ┬Ąg/hr) in opioid-na├»ve patients with cancer pain [16]. Because most advanced cancer patients experience moderate-to-severe pain [17], clinical trials using low doses of TDF in this population are needed urgently. Therefore, the aim of this study was to assess the efficacy and preference for low-dose formulations of TDF for the management of patients with cancer pain of moderate or severe intensity.
A multicenter, nonrandomized, open-label, prospective study was conducted between April 2007 and February 2009 in seven tertiary cancer hospitals. The inclusion criteria were age Ōēź 18 years and cancer pain of moderate-to-severe intensity (numeric rating scale [NRS] Ōēź 4). Mild cancer pain (NRS < 4) was excluded. Informed consent and institutional approval were obtained before the study was performed. The exclusion criteria were a history of strong or weak opioid use in the prior 1 month, receiving chemotherapy or radiotherapy, an expected survival of < 2 months, CO2 retention, a history of allergy to opioids, poor hepatic function (alanine transaminase or aspartate transaminase Ōēź 2 ├Ś the upper normal limit or bilirubin Ōēź 2.0 mg/dL), or renal dysfunction (serum creatinine Ōēź 2.0 mg/dL). Patients were also excluded if their TDF had been detached for > 48 hours or not used in the 24 hours before the second visit.
The initial dose of TDF was 12.5 ┬Ąg/hr (Janssen, Seoul, Korea). Patients received phone calls every 3 days to monitor their pain. The dose of TDF was adjusted every 3 days depending on pain intensity until analgesic efficacy was attained or dose-limiting toxicity occurred. An immediate-release form of any strong opioid equivalent to 10% to 20% MEDD was allowed for breakthrough pain. Adjuvant symptomatic medications such asonsteroidal anti-inflammatory drugs, acetaminophen, antiemetics, and steroids were permitted according to clinical need. Antidepressants, anxiolytics, and sleeping pills were allowed only at a stable dose if patients had used the medications before enrollment.
Information regarding patient demographic information and current medical history, including diagnosis, metastatic organs, and stage of illness, was obtained at baseline (day 1). The following data were obtained at baseline and the final study visit (29 ┬▒ 3 days): mean pain intensity (last 24 hours, as measured by NRS), patient and investigator satisfaction, detailed reasons for the satisfaction, the administered dose of TDF, and concomitant medications.
Pain intensity and AEs were determined using phone inquiries to patients every 3 days during the study period (days 4, 7, 10, 13, 16, 19, 22, and 25). Patients and investigators were asked about their subjective satisfaction with TDF at the final visit. A modified five-point Likert scale was used to evaluate the investigator satisfaction [18]. Patient satisfaction was evaluated using a simple "satisfied" or "unsatisfied" question. Investigators used mild, moderate, and severe to describe the intensity of the AEs [19]. A decrease of two points on the NRS was defined as the response to medication based on a previous report that a cutoff of a two-point difference provides an appropriate surrogate measure of a clinically important difference [20].
Descriptive statistics (mean, median, frequency, and percentage) were used to summarize the demographic characteristics of the patients. All data were analyzed using modified intent-to-treat (ITT) and per-protocol (PP) principles. Of the entire subject group, individuals who did not meet the inclusion criteria, who had not received the investigational medicinal product even once, and those with pain that could not be evaluated on the day of the first telephone inquiry were excluded from the ITT population. The PP population included only patients who completed the clinical study without any protocol violation. The patient cohort was divided into two groups: the moderate and severe pain groups. Subgroup analyses were performed to assess whether differences in the treatment time or TDF dose required for appropriate pain management occurred. Paired t tests, chi-square tests, and logistic regression analysis were used for data comparisons, as appropriate. A p-value < 0.05 was considered to indicate statistical significance.
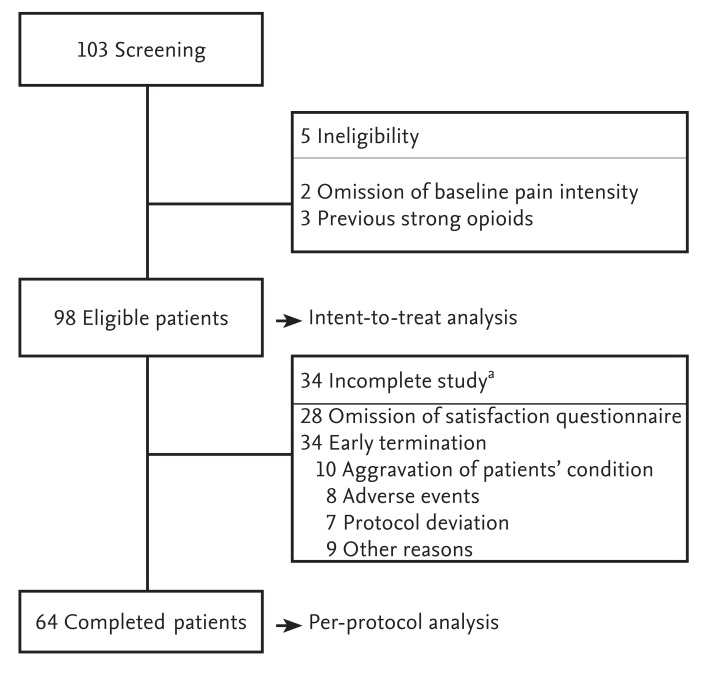
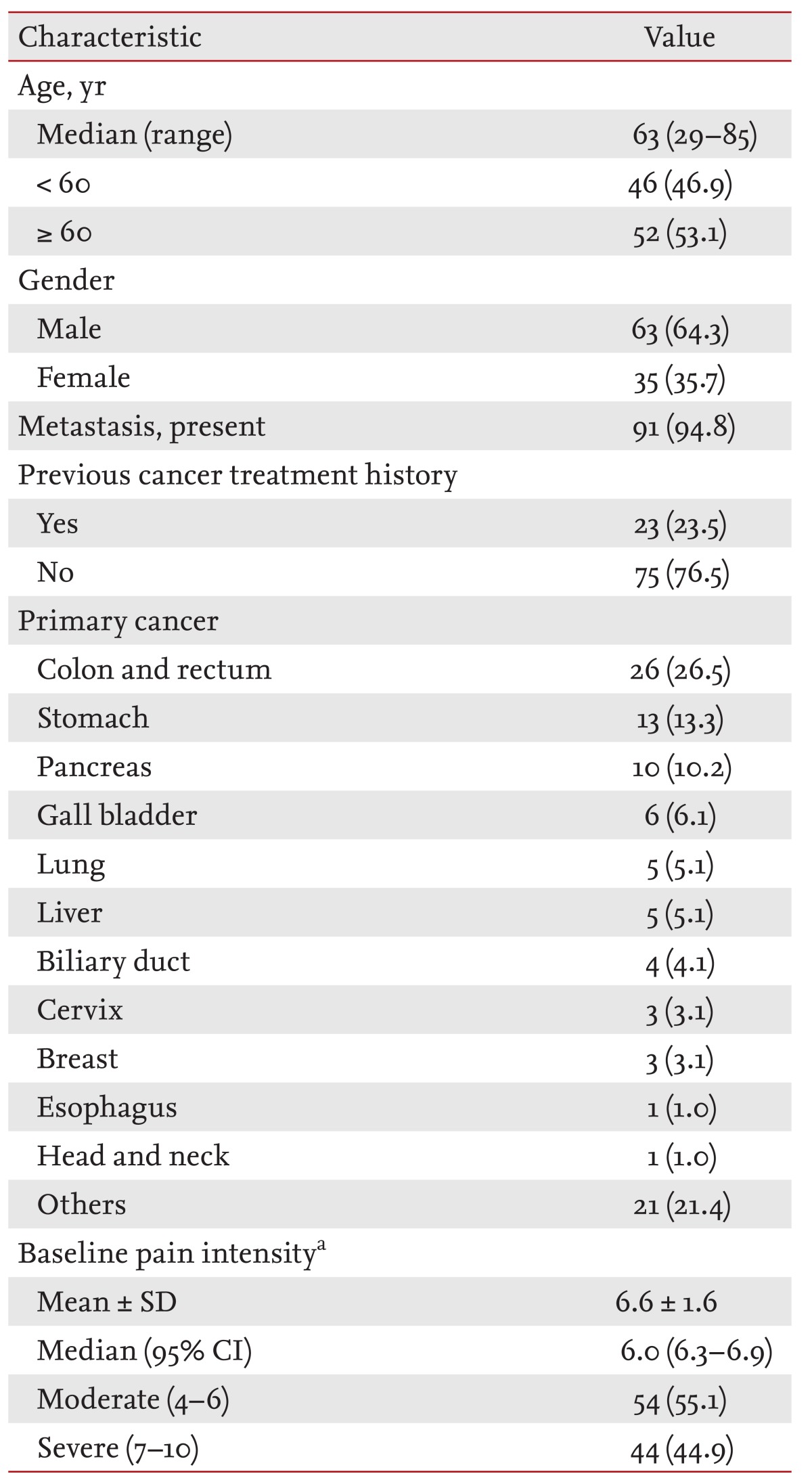
Of the 103 patients screened, five were excluded because of ineligibility. ITT analysis was performed in 98 patients (Fig. 1). Of these, 34 patients (34.7%) did not complete the study: 10 because of a deteriorated condition due to cancer progression, eight because of AE, seven for protocol violation, and nine for other reasons. Satisfaction questionnaires were omitted in 28 patients. The demographic characteristics of the patients are described in Table 1. Males accounted for 64.3% (n = 63) of patient cohort. The most common type of cancer was colorectal (n = 26, 26.5%). The median intensity of the baseline pain was 6.0 (quartile 1 to 3, 5.0 to 8.0). The proportion of moderate (NRS score 4 to 6) and severe (NRS score 7 to 10) pain intensity was 55.1% and 44.9%, respectively.
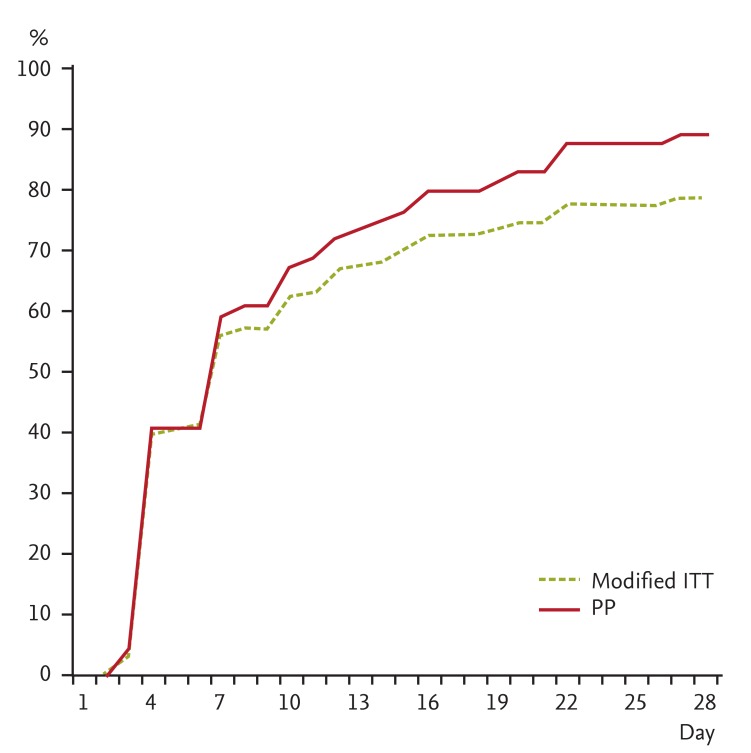
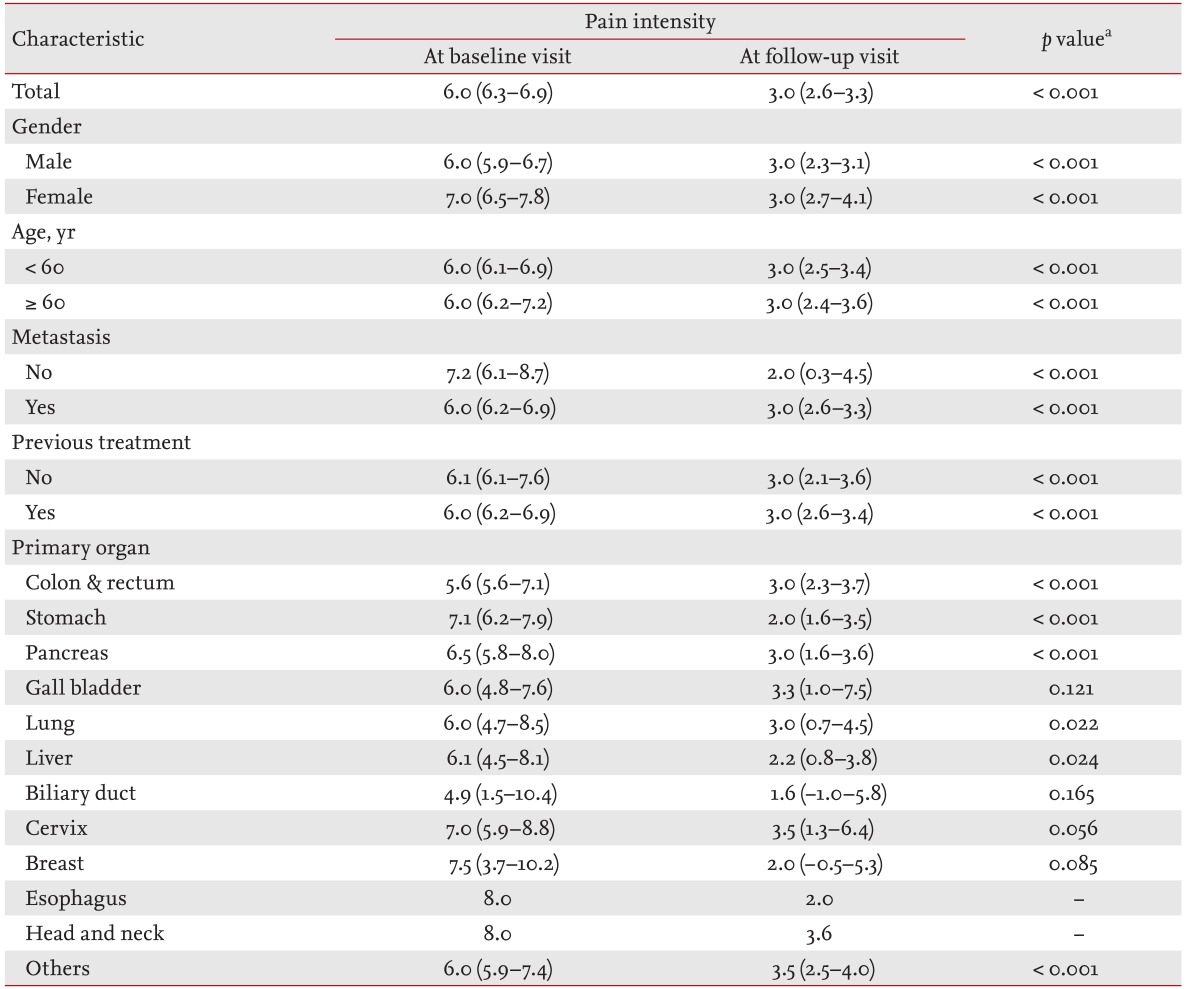
The median pain intensity was improved from 6.0 at baseline to 3.0 (p < 0.001) at follow-up (Table 2). Of the 98 total patients, pain was alleviated to an NRS < 3 in 77 patients (78.6%). In PP analysis, 57 of 64 patients (89.1%) achieved pain relief (NRS Ōēż 3) (Fig. 2). The median time to NRS Ōēż 3 was 4 days in the moderate pain group, and 7 days in the severe pain group. Seventy-five patients (76.5%) met the criteria for a response, with median change of 3.2.
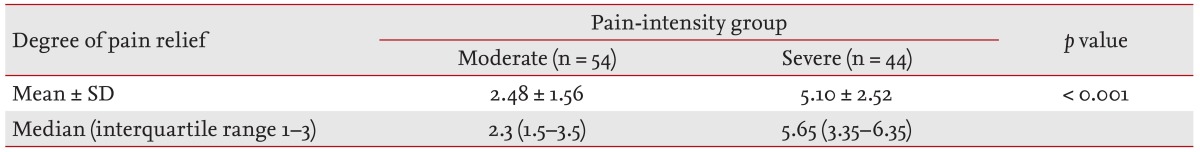
The efficacy of a starting low dose of TDF for pain relief was consistent across groups stratified according to gender, age, metastasis, and previous treatment (Table 2). The mean decrease in pain intensity was significantly greater in the severe pain group compared with the moderate pain group (5.10 ┬▒ 2.48 vs. 2.48 ┬▒ 1.56, p < 0.001) (Table 3). ITT analysis revealed that TDF dose (mean 27.8 ┬Ąg/hr vs. 24.8 ┬Ąg/hr, p = 0.423) and the mean treatment time (7.5 days vs. 7.9 days, p = 0.740) required for appropriate pain control (NRS Ōēż 3) were not different between the two pain-intensity groups. There were also no differences in time to pain control and required TDF dose between the two groups according to PP analysis.
Questionnaires for satisfaction were obtained from patients and investigators at the follow-up visit. Of the 64 PP cohort patients, 53 (82.8%) were satisfied with their pain management overall. A similar proportion of investigators reported a satisfactory response to starting pain treatment with low-dose TDF (very satisfied 25%, satisfied 62%). In patient questionnaires asking for the detailed reasons for satisfaction, the most common answer was "excellent analgesic effect (30 patients, 56.6%)," followed by "convenient administration (23 patients, 43.4%)."
Most of the AEs (62%) were mild in intensity, and no severe-intensity AEs were observed. Of the reported AEs, gastrointestinal symptoms including nausea (38%) and vomiting (22%) were most common (Table 4). Of the eight patients who dropped out of the study due to AE, nausea and/or vomiting were also the most common reasons (five patients), followed by constipation (one patient), drowsiness (one patient), and dyspnea (one patient).
Although TDF demonstrated a similar effectiveness to oral strong opioids in cancer patients under various conditions [15,21,22,23,24], little data were available regarding treatment with low-dose TDF in cancer patients with moderate-to-severe pain intensity [16]. The current study demonstrates that a low-dose of starting TDF could be effective in the opioid-na├»ve patients suffering from significant cancer pain. These results were consistent in both ITT and PP analyses. Regarding time to pain control, most patients achieved appropriate pain relief (NRS Ōēż 3) within a week, even those with a severe pain intensity. The European Society of Medical Oncology guidelines recommend a differential approach according to pain intensity [7]. Specifically, they advocate an oral administration route in most patients, and reserve transdermal formulations for patients whose opioid requirements are stable. However, the current results suggest that the initial implementation of low-dose TDF in opioid-na├»ve cancer patients might be an effective alternative for the management of moderate-to-severe cancer pain. Mercadante et al. [16] performed a study in a similar setting, and reported a comparable treatment outcome. However, they did not obtain treatment outcomes in patients with severe pain. Because physicians might hesitate to apply TDF as the initial treatment for severe cancer pain because of its slow onset of action, the current study analyzed data according to pain intensity. Data revealed that TDF was equally effective in the severe- and moderate-intensity pain groups.
Although strong opioids are recommended as the first-line medication in patients with moderate-to-severe cancer pain, there is no consensus regarding the appropriate starting doses in opioid-naïve patients. Previous studies reported that moderate-to-severe pain in cancer patients could be controlled effectively using low doses of opioids (range, 45 to 80 mg MEDD) [16,25,26,27]. The median MEDD for appropriate pain control was 60 mg in the current study.
Of the previous studies of TDF for cancer pain [12], most used 25 ┬Ąg/hr as starting dose, which is equiva lent to 60 mg MEDD. However, the abrupt introduction of this dose to opioid-na├»ve patients might expose the subjects to a high-risk of adverse effects and subsequently decreased compliance [13,15,28]. A cancer pain study in opioid-na├»ve patients who started strong opioids at the ranges of 50 to 60-mg MEDD reported that as many of 36% of patients prematurely discontinued the trial due to AE [28]. Although the current study had a considerable rate of AE (33.7%) during the course of treatment, the proportion (8.3%) of discontinued cases due to AE was acceptable. Furthermore, the discontinued patients did not have severe AE, although the severity was rated by the investigators. Previous studies using fentanyl patches in opioid-na├»ve patients reported dropout rates of 4% to 10% due to AE [28,29]. Meanwhile, Hui et al. [30] reported that attrition rates reached 26% for the primary endpoint and 44% at the end of the study, respectively, in a palliative care trial.
Large patient-to-patient variations in the pharmacokinetic parameters of fentanyl patches exist, which could cause unexpectedly high serum concentrations of opioids [31]. Considering the dose-dependency of opioid-induced AEs [32] and the large interpersonal pharmacokinetic diversity, starting with low-dose TDF could be a safe and effective alternative for moderate-to-severe cancer pain.
The dose required for pain control (median 25 ┬Ąg/hr) was not high in the current study. Therefore, we assumed that the response to opioid therapy might be more dependent on interindividual differences in pharmacological characteristics rather than a simple increase in the opioid dose. Because large individual variations exist in response to opioid analgesics [33], no single opioid can address all cancer pain sufficiently. Opioid rotation is based on this concept, and is a well-established interventional approach for opioid nonrespondents [34]. Riley et al. [35] reported that most morphine nonrespondents with cancer pain (MEDD of 73.7 mg) were controlled successfully by rotating to another opioid agent. Unfortunately, no randomized trials or studies have reported data regarding continued dose escalation versus opioid rotation in patients with chronic cancer pain. Therefore, future studies assessing this issue are warranted.
Patients receiving chemotherapy or radiotherapy were excluded from the current study to ensure patient homogeneity. The period of the current study was 4 weeks from enrollment to final assessment. This would be sufficient to observe an effect on the cancer itself if patients were being treated accordingly. Therefore, it would be unclear whether the pain relief arose from the TDF medication or improved cancer characteristics.
The current study has a limitation in that questionnaires regarding QOL were not collected. In addition, the study had an open and uncontrolled design.
In conclusion, low-dose TDF was an effective treatment in patients with cancer pain of moderate-to-severe intensity. Future randomized trials assessing the efficacy of TDF in patients with severe pain and/or optimal starting doses are warranted.
References
1. Temel JS, Greer JA, Muzikansky A, et al. Early palliative care for patients with metastatic non-small-cell lung cancer. N Engl J Med 2010;363:733ŌĆō742PMID : 20818875.


2. Cancer pain relief and palliative care: report of a WHO Expert Committee. World Health Organ Tech Rep Ser 1990;804:1ŌĆō75PMID : 1702248.


3. Ventafridda V, Tamburini M, Caraceni A, De Conno F, Naldi F. A validation study of the WHO method for cancer pain relief. Cancer 1987;59:850ŌĆō856PMID : 3802043.


4. Meuser T, Pietruck C, Radbruch L, Stute P, Lehmann KA, Grond S. Symptoms during cancer pain treatment following WHO-guidelines: a longitudinal follow-up study of symptom prevalence, severity and etiology. Pain 2001;93:247ŌĆō257PMID : 11514084.


5. Burton AW, Hamid B. Current challenges in cancer pain management: does the WHO ladder approach still have relevance? Expert Rev Anticancer Ther 2007;7:1501ŌĆō1502PMID : 18020918.


6. Swarm R, Abernethy AP, Anghelescu DL, et al. Adult cancer pain. J Natl Compr Canc Netw 2010;8:1046ŌĆō1086PMID : 20876544.



7. Ripamonti CI, Santini D, Maranzano E, Berti M, Roila F. ESMO Guidelines Working Group. Management of cancer pain: ESMO Clinical Practice Guidelines. Ann Oncol 2012;23(Suppl 7):vii139ŌĆōvii154PMID : 22997447.


8. Jacox A, Carr DB, Payne R. New clinical-practice guidelines for the management of pain in patients with cancer. N Engl J Med 1994;330:651ŌĆō655PMID : 7508094.


9. Hanks GW, Conno F, Cherny N, et al. Morphine and alternative opioids in cancer pain: the EAPC recommendations. Br J Cancer 2001;84:587ŌĆō593PMID : 11237376.



10. Coller JK, Christrup LL, Somogyi AA. Role of active metabolites in the use of opioids. Eur J Clin Pharmacol 2009;65:121ŌĆō139PMID : 18958460.


11. Prommer E. The role of fentanyl in cancer-related pain. J Palliat Med 2009;12:947ŌĆō954PMID : 19807240.


12. Komurcu S, Turhal S, Altundag K, et al. Safety and efficacy of transdermal fentanyl in patients with cancer pain: phase IV, Turkish oncology group trial. Eur J Cancer Care (Engl) 2007;16:67ŌĆō73PMID : 17227355.


13. Hoya Y, Okamoto T, Yanaga K. Evaluation of analgesic effect and safety of fentanyl transdermal patch for cancer pain as the first line. Support Care Cancer 2010;18:761ŌĆō764PMID : 20354734.


14. Yang Q, Xie DR, Jiang ZM, et al. Efficacy and adverse effects of transdermal fentanyl and sustained-release oral morphine in treating moderate-severe cancer pain in Chinese population: a systematic review and meta-analysis. J Exp Clin Cancer Res 2010;29:67. PMID : 20529380.



15. Vielvoye-Kerkmeer AP, Mattern C, Uitendaal MP. Transdermal fentanyl in opioid-naive cancer pain patients: an open trial using transdermal fentanyl for the treatment of chronic cancer pain in opioid-naive patients and a group using codeine. J Pain Symptom Manage 2000;19:185ŌĆō192PMID : 10760623.


16. Mercadante S, Porzio G, Ferrera P, Aielli F, Adile C, Ficorella C. Low doses of transdermal fentanyl in opioid-naive patients with cancer pain. Curr Med Res Opin 2010;26:2765ŌĆō2768PMID : 21034376.


17. Yennurajalingam S, Kang JH, Hui D, Kang DH, Kim SH, Bruera E. Clinical response to an outpatient palliative care consultation in patients with advanced cancer and cancer pain. J Pain Symptom Manage 2012;44:340ŌĆō350PMID : 22699092.


18. Likert R. A technique for the measurement of attitudes. Arch Psychol 1932;22:1ŌĆō55.
19. Goldfarb NM. Adverse event terminology. J Clin Res Best Pract 2012;8:1ŌĆō17.
20. Farrar JT, Young JP Jr, LaMoreaux L, Werth JL, Poole RM. Clinical importance of changes in chronic pain intensity measured on an 11-point numerical pain rating scale. Pain 2001;94:149ŌĆō158PMID : 11690728.


21. Mercadante S, Porzio G, Ferrera P, et al. Sustained-release oral morphine versus transdermal fentanyl and oral methadone in cancer pain management. Eur J Pain 2008;12:1040ŌĆō1046PMID : 18353696.


22. Kress HG, Von der Laage D, Hoerauf KH, et al. A randomized, open, parallel group, multicenter trial to investigate analgesic efficacy and safety of a new transdermal fentanyl patch compared to standard opioid treatment in cancer pain. J Pain Symptom Manage 2008;36:268ŌĆō279PMID : 18538974.


23. Mystakidou K, Tsilika E, Parpa E, et al. Long-term cancer pain management in morphine pre-treated and opioid naive patients with transdermal fentanyl. Int J Cancer 2003;107:486ŌĆō492PMID : 14506751.


24. Iconomou G, Viha A, Vagenakis AG, Kalofonos HP. Transdermal fentanyl in cancer patients with moderate-to-severe pain: a prospective examination. Anticancer Res 2000;20(6C):4821ŌĆō4824PMID : 11205226.

25. Mercadante S, Porzio G, Ferrera P, et al. Low morphine doses in opioid-naive cancer patients with pain. J Pain Symptom Manage 2006;31:242ŌĆō247PMID : 16563318.


26. Drexel H, Dzien A, Spiegel RW, et al. Treatment of severe cancer pain by low-dose continuous subcutaneous morphine. Pain 1989;36:169ŌĆō176PMID : 2465533.


27. Mercadante S, Porzio G, Ferrera P, et al. Low doses of transdermal buprenorphine in opioid-naive patients with cancer pain: a 4-week, nonrandomized, open-label, uncontrolled observational study. Clin Ther 2009;31:2134ŌĆō2138PMID : 19922884.


28. van Seventer R, Smit JM, Schipper RM, Wicks MA, Zuurmond WW. Comparison of TTS-fentanyl with sustained-release oral morphine in the treatment of patients not using opioids for mild-to-moderate pain. Curr Med Res Opin 2003;19:457ŌĆō469PMID : 14594516.


29. Allan L, Richarz U, Simpson K, Slappendel R. Transdermal fentanyl versus sustained release oral morphine in strong-opioid naive patients with chronic low back pain. Spine (Phila Pa 1976) 2005;30:2484ŌĆō2490PMID : 16284584.


30. Hui D, Glitza I, Chisholm G, Yennu S, Bruera E. Attrition rates, reasons, and predictive factors in supportive care and palliative oncology clinical trials. Cancer 2013;119:1098ŌĆō1105PMID : 23132290.



31. Solassol I, Bressolle F, Caumette L, et al. Inter- and intraindividual variabilities in pharmacokinetics of fentanyl after repeated 72-hour transdermal applications in cancer pain patients. Ther Drug Monit 2005;27:491ŌĆō498PMID : 16044107.


32. Barber A, Gottschlich R. Novel developments with selective, non-peptidic kappa-opioid receptor agonists. Expert Opin Investig Drugs 1997;6:1351ŌĆō1368.


33. Dahan A. The importance of individual differences in response to opioid therapy. Therapy 2009;6:633ŌĆō635.

Figure┬Ā2
Time to pain control (numeric rating scale Ōēż 3). ITT, intent-to-treat group (n = 98); PP, per-protocol group (n = 64).
Table┬Ā2
Change in pain intensity from baseline characteristics after low-dose transdermal fentanyl treatment (n = 98)
-
METRICS

- Related articles
-
The efficacy of denosumab in Korean male patients with osteoporosis2022 September;37(5)




 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print


