 |
 |
| Korean J Intern Med > Volume 20(1); 2005 > Article |
|
Abstract
Background
Transforming growth factor-β (TGF-β) stimulates renal fibrosis in various renal diseases including IgA nephropathy.
Methods
We examined whether immunoglobulin A (IgA) stimulated TGF-β1 synthesis in human mesangial cells (MCs), and whether this effect was mediated through the protein kinase C (PKC) pathway. We measured the intraglomerular TGF-β1 mRNA expression by using competitive RT-PCR, and this was compared with various parameters in IgA nephropathy patients.
Results
The IgA aggregate increased the TGF-β1 mRNA expression in MCs, while this expression was not affected by the culture media or IgG aggregate. Phorbol 12-myristate 13-acetate and calphostin C did not influence the TGF-β1 mRNA expression that was increased by the IgA aggregate. Intraglomerular TGF-β1 mRNA expression was significantly correlated with creatinine clearance (r=-0.764, p=0.027), daily proteinuria (r=0.781, p=0.022), serum creatinine (r=0.884, p=0.004), and tubulointerstitial changes (r=0.809, p=0.015). Glomerular TGF-β1 mRNA expression was associated with an increased tendency for glomerulosclerosis (r=0.646, p=0.084). After 4 years, patients with a high expression of intraglomerular TGF-β1 mRNA showed a tendency for an decrease of their renal function.
Mesangial expansion and proliferation are the most common histologic findings in IgA nephropathy1). As this disease progresses, glomerulosclerosis, tubular atrophy and interstitial fibrosis develop. These fibrotic changes and the extracelluar matrix accumulation are known to be stimulated by TGF-β12, 3).
Induction of the extracellular matrix components by TGF-β is responsible for wound healing. However, the overexpression of TGF-β could result in the excessive tissue deposition of extracellular matrix proteins, and this ultimately leads to tissue fibrosis. The increased expression of TGF-β mRNA and production of TGF-β proteins are apparent for the various fibrotic kidney diseases, including IgA nephropathy.
TGF-β contributes to natural course of human IgA nephropathy4). TGF-β in the mesangium is especially related to the degree of extracellular matrix accumulation, and its increased gene expression from the circulating CD4+ T cells may also contribute to the glomerulosclerosis in patients with IgA nephropathy5, 6). Although TGF-β plays an important role in the pathogenesis of IgA nephropathy, it is not clear whether intraglomerular TGF-β mRNA expression is related to the clinical features and pathologic findings.
In the present study, we examined whether immunoglobulin A (IgA) stimulated the TGF-β1 expression in cultured mesangial cell, and whether this expression was mediated through the protein kinase C pathway. We also microdissected the glomeruli of patients with IgA nephropathy, and we quantified intraglomerular mRNA expression of TGF-β1 by using competitive RT-PCR. Then, the degree of the TGF-β1 mRNA expression was compared with various clinical parameters and pathologic changes to determine the role of TGF-β1 at the time of biopsy.
The normal renal cortex of human kidney was obtained immediately after nephrectomy. The glomeruli were treated with collagenase (Gibco BRL, Gaitherburg, USA), and they were plated onto culture dishes in Dulbecco's modified Eagle medium (DMEM, Gibco BRL) containing 10% heat inactivated fetal calf serum (Sigma Chemical, St. Louis, USA). Mesangial cells were cultured in DMEM supplemented with 17% fetal calf serum, 2% penicillin, 2% streptomycin, 1% HEPES, 2 g sodium bicarbonate and 2 mM L-glutamine at 37℃ in 5% CO2, 95% air. With the use of immunohistochemical staining, the mesangial cells were identified due to their large stellate shape, and the myosin and fibronectin were also stained, whereas the common leukocyte antigen and factor VIII were not stained.
The mesangial cells were incubated for 24 hours in serum-free media, and then they were cultured in the media containing an IgA aggregate (n=4, 100 µg/mL), or an IgG aggregate (n=3, 100 µg/mL). The cell were pretreated with 100 nM of phorbol 12-myristate 13-acetate (PMA) for 24hrs in order to deplete their protein kinase C (PKC), and some of the cells were pretreated with 200 nM calphostin C (a PKC inhibitor).
Aggregation was brought about by heating the IgA or IgG for 30 minutes at 63℃. After cooling it in room temperature, the proteins were centrifuged at 11,000 g for 5 minutes to remove the insoluble aggregate. The supernatants were then used as the heat-aggregated IgA or IgG7).
Glomular microdissection was carried out within 30 minutes after biopsy in a cooled dish containing RNase inhibitor (10 mM of vanadyl ribonucleoside complex, Life technology, Gaithersburg, USA). The glomeruli were separated from the tubules, and they were washed with saline to remove tissue debris and VRC, and then they were pooled at 5 glomeuli per PCR tube with the tube containing 5 mM dithiothreitol and 1.2 U/µL of RNase inhibitor (Boehringer Mannheim Corp., Indianapolis, USA). The glomeruli were permeated immediately before reverse transcription (RT) with a mixture containing 0.9% Triton X-100, 1.2 U/µL of placental RNase inhibitor, and 5 mM dithiothreitol. The five glomeruli in the pools were reverse transcribed with oligo dT, and the products were then combined after RT to inhibit errors that could be derived from the variation in glomerular size. RT was performed using a cDNA synthesis kit (Boehringer Mannheim) as described previously8).
The mesangial cells were collected using a cell scraper, and they were resuspended in Trizol reagent (Invitrogen, Carlsbad, CA) containing RNase inhibitor. A cDNA synthesis kit was used for RT, and a random primer (6mer) was used to prime the mRNA RT. The RT reaction was set up in a 20 µL mixture containing 50 mM KCl, 10 mM Tris/HCl, 5 mM MgCl2, 1 mM of each dNTPs, 2.5 µM random hexamers, 20 U Rnase inhibitor and 50 U of M-MLV reverse transcriptase. The reaction mixture was incubated for 60 min at 42℃, and then it was heated for 7 minutes at 90℃ in a thermocycler (Crocodile III, Oncor Co., Japan).
After cDNA synthesis by RT, the incubation mixture was split into two portions in order to amplify the TGF-β1 cDNA and the GAPDH cDNA using specific primers: for the TGF-β1 DNA, the sense primer was 5' GGA GGG GAA ATT GAG GGG TTT CGC 3', and the anti-sense primer was 5' TTA TGC TGG TTG TAC AGG GC 3'; for the GAPDH DNA, the sense primer was 5' CCC CAG GCA CCA GGG CGT GAT 3', and the anti-sense primer was 5' GGT CAT CTT GCG GTT GGC CTT GGG GT 3'. A semi-quantitative measurement of mRNA expression was performed by optimizing the amount of cDNA and number of PCR cycles as described previously7).
PCR was done in a 50 µL volume containing 50 mM KCl, 10 mM Tris/HCl (pH 8.3), 200 µM of each dNTPs, 50 pmol of each primer, 2 U Taq DNA polymerase and 1.5 mM MgCl2. The mixture was first heated for 5 minutes at 95℃, and this was followed by 36 cycles: each cycle was 2.5 minutes at 95℃, 1.5 minutes at 55℃, 3 minutes at 72℃, and a final extension for 7 minutes at 72℃. For quantification of the PCR products and the house keeping gene, glyceraldehyde 3 phosphate dehydrogenase (GAPDH) PCR was performed in a parallel fashion in separate tubes.
To quantify the cDNAs for TGF-β1 in the glomeruli, competitive PCR was performed by adding decreasing amounts of mutant templates to the glomerular cDNA. For the TGF-β1 and GAPDH, deletion cDNA mutant templates for each of these were developed to create 51 and 39 bp deletions in the middle of the molecules, and this resulted in mutant cDNAs of 339 and 559bp, respectively.
Human TGF-β1 cDNA was amplified with the following primers: 5' GGA GGG GAA ATT GAG GGG TTT CGC 3' as the sense primer and 5' TTA TGC TGG TTG TAC AGG GC 3' as the antisense primer. Human GAPDH cDNA was amplified with the following primers: 5' CCA CCC ATG GCA AAT TCC ATG GCA 3' as the sense primer and 5' TCT AGA CGG CAG GTC AGG TCC ACC 3' as the antisense primer.
Competitive PCR was performed with the sample DNA by applying serial dilutions of the mutant DNA in the same tubes under the condition of 1 minute at 94℃, 1 minute at 60℃, and 3 minutes at 72℃ for 36 cycles for the TGF-β1 and 32 cycles for the GAPDH. The PCR products were electrophoresed in 2% agarose gel; they were eluted using a Qiagen DNA extraction kit and then sequenced to confirm the PCR products by using an automatic sequencing system (ABI Genetic Analyzer 310; PRISM, Branchburg Park, USA).
The ratio of the mutant DNA band density to the test DNA band density was calculated for each lane, and the data was plotted as a function of the amount of mutant template that was added to the reaction. The quantity of cDNA in the test sample was the amount at which the mutant/test band density was equal to one10).
Among the patients with biopsy-proven IgA nephropathy, eight patients (3 men and 5 women) having more than 10 glomeruli from their biopsy tissue were included. All the patients received angiotensin converting enzyme inhibitors during the follow up period. The renal biopsy procedure was approved by the Korea University Research and Education Institute Investigational Review Board, and informed consents were obtained from each patient. Blood urea nitrogen, serum creatinine, IgA and C3 concentrations were measured by Nephelometry (Behring, Germany). Creatinine clearance and daily proteinuria were also measured by employing 24 hours urine collections.
The morphological findings from the biopsy material such as the degree of glomerulosclerosis, tubulointerstitial changes, IgA staining pattern and Haas subclassification9) were determined "blindly" by two different renal pathologists. A semiquantitative score from 0 to 4+ was used to evaluate the degree of glomerulosclerosis: a 1+ lesion represented involvement of 25% of the glomerulus; a 2+ lesion represented involvement of 25~50% of the glomeruli; a 3+ lesion represented involvement of 5 0~75% of the glomeruli; and a 4+ lesion represented involvement of more than 75% of the glomeruli. Tubulointerstitial changes, including tubular dilatation, atrophy, proteinous casts, interstitial edema and mononuclear cell infiltrates were graded from 0 to 4+ (0=no change; 1+=change affecting <25% of the sample; 2+=change affecting 25~50% of the sample; 3+=change affecting 50~75% of the sample; 4+=change affecting >75% of the sample).
The IgA aggregates directly stimulated TGF-β1 mRNA expression in the cultured mesangial cell. The expression of TGF-β1 mRNA was significantly higher under the condition of IgA, whereas its expression was not changed under the condition of IgG aggregates (Figure 1). The expression of TGF-β1 mRNA in the IgA-treated mesangial cells during the incubation with PMA for 24 hours was not significantly different from the control. Similarly, in the case of a one hour pretreatment with calphostin C, there was no significant decrease in the mRNA expression of TGF-β1 (Figure 2).
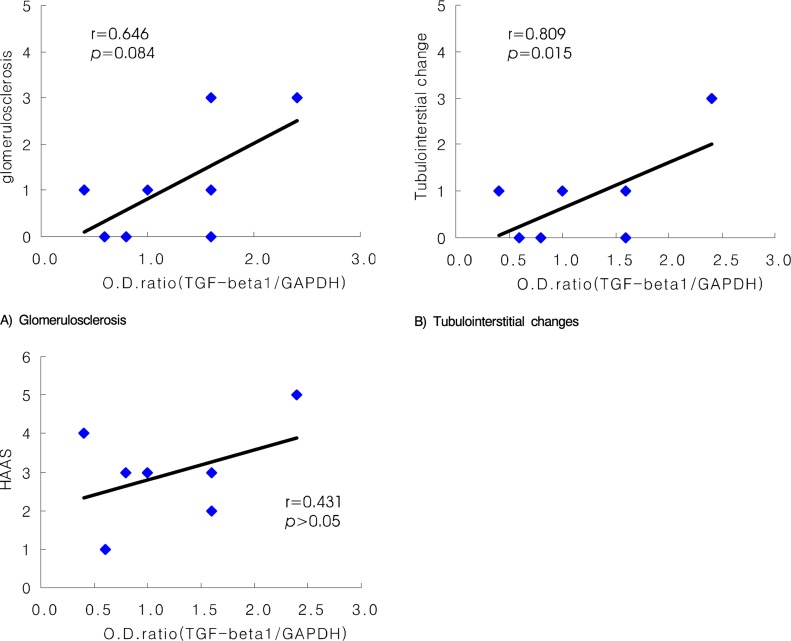
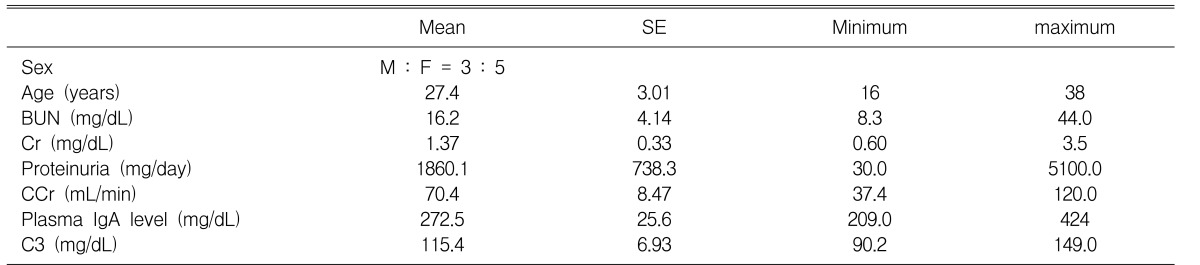
The mean age of the eight patients (3 men and 5 women) was 27.4±8.5 yrs. The other basic characteristics are summarized in Table 1. Figure 3 shows the representative result of competitive PCR with glomeruli that were obtained from patients with IgA nephropathy. The intraglomerular TGF-β1/GAPDH mRNA ratio was significantly correlated with the levels of 24-hr proteinuria (r=0.781, p=0.022), serum creatinine (r=0.884, p=0.004), and tubulointerstitial changes (r=0.809, p=0.015). In addition, the intraglomerular TGF-β1 mRNA expression showed a significant negative correlation with the creatinine clearance (r=-0.0764, p=0.027), and it also showed positive correlation with glomerulosclerosis (r=0.646, p=0.084), but this was statistically insignificant. However, the TGF-β1 mRNA expression was not correlated with such other parameters as the peripheral blood IgA concentration, the intraglomerular immunoreactivity for IgA, and the Haas pathologic subclassification (Figure 4, 5).
In the present study, the IgA aggregate was shown to directly stimulate TGF-β1 mRNA expression in the cultured mesangial cells, and this was independent of the PKC pathway. In addition, the glomerular TGF-β1 mRNA expression was closely correlated with several factors that were known to be prognostic markers, such as the tubulointerstitial fibrosis, creatinine clearance and daily proteinuria.
TGF-β stimulates the synthesis of the matrix protein and it downregulates protease, following the induction of the extracelluar matrix expansion10). In an animal model system, TGF-β1 gene transfer into the mesangium of normal rats via the renal artery led to glomerulosclerosis, and systemic treatment with TGF-β1 antagonists prevented glomerulosclerosis11, 12). In human studies, fibrosis in the extracellular matrix that was due to the overproduction of TGF-β has been reported in various renal diseases, including diabetic nephropathy and acute nephritis13, 14).
For IgA nephropathy, in situ hybridization and indirect immunofluorescence study were used to evaluate the increased intraglomerular expression of TGF-β13-16). Lai et al have also reported that the intraglomerular immunofluorescent reactivity with anti-TGF-β antibody in the mesangium correlated with the severity of the histologic grading, and there was an increase of TGF-β gene expression in the circulating CD4+ T cells of patients with IgA nephropathy6). Furthermore, Muda et al have also reported that glomerular immunoreactivity for the TGF-β isoform correlated with the severity of proliferative lesions observed for different kinds of glomerulonephritis including IgA nephropathy17). Although these studies have proved that TGF-β was related to glomerulosclerosis in IgA nephropathy, they did not compare the TGF-β with the clinical status, nor did the studies quantify the TGF-β.
In this study, we microdissected glomeruli and then quantified the glomerular TGF-β1 mRNA expression using competitive RT-PCR, and we compared this expression with both the clinical and pathological findings. As expected, intraglomerular TGF-β1 mRNA expression was correlated with tubulointerstitial fibrosis and it tended to correlate with glomerulosclerosis. These results suggested that the glomerular TGF-β1 mRNA expression might be a useful prognostic marker in this disease because it correlated with daily proteinuria, creatinine clearance and tubulointerstitial changes. However, its expression was not correlated with the Hass pathologic classification, nor was it correlated with the intensity of the intraglomerular IgA staining.
It is not clear whether these clinical parameters correlated with the glomerular and tubulointerstitial changes. Several prognostic factors, including severe proteinuria, elevated serum creatinine, the degree of glomerulosclosis and tubulointerstitial fibrosis, and the class III and IV lesions seen on biopsy tissue were reported for IgA nephropathy18). Therefore, we suspected that the daily proteinuria and creatinine clearance were related with glomerulosclerosis and tubulointerstitial changes. In our study, the Haas pathologic classification was not correlated with intraglomerular mRNA expression of TGF-β1, and this might have been due to the rather small number of samples. Since 4 of 8 patients had the class III Haas subclassification, further comparative studies of intraglomerular TGF-β1 mRNA expression within the same category of Haas classification are needed.
While the IgA aggregate enhanced TGF-β1 expression in vitro, the degree of intraglomerular IgA deposition was not significantly related with mRNA expression of TGF-β1. This result might be due to the fact that TGF-β1 gene expression in vivo is regulated by many stimuli such as local hormones and cytokines, in addition to the IgA antibody.
The intracellular signaling mechanism of IgA induced TGF-β1 expression is not clear. In our study, however, PKC depletion and PKC inhibition did not decrease TGF-β1 gene expression in the IgA-treated mesangial cell. These results were in agreement with the previous report that showed the stretch-induced TGF-β expression was not affected by both PKC inhibitor and activator19). Therefore, further investigation on the intracellular signaling mechanism of IgA-induced TGF-β1 gene activation is needed.
Since this experiment was a cross-sectional study on a small number of patients, it is difficult to conclude, at this time, whether the intraglomerular TGF-β1 gene expression is a useful molecular marker for the progression of IgA nephropathy. Four of the 8 patients were followed up for 4 years. Comparing the changes of reciprocal serum creatinine level between 2 groups that were formed based on the initial intraglomerular TGF-β1 mRNA expression, the reciprocal creatinine level declined more rapidly in the group with the high expression of intraglomerular TGF-β1 mRNA.
Although the mRNA level cannot represent the protein level, the close correlation between the TGF-β1 mRNA expression and glomerulosclerosis as well as tubulointerstitial changes suggest an important role for TGF-β1 in renal disease progression. The urinary concentration of TGF-β1 was recently reported as a reliable marker for the prognosis of IgA nephropathy patients20). Furthermore, latent TGF-binding protein, which is essential for TGF-β to interact with the extracellular matrix, was used as a marker for renal disease progression in adriamycin induced nephropathy21).
In conclusion, the IgA aggregate increased TGF-β1 mRNA expression in the cultured mesangial cells, and this was independent of the PKC pathway. Considering that intraglomerular TGF-β1 mRNA expression showed a significant correlation with several prognostic factors, the evaluation of intraglomerular TGF-β1 mRNA expression from biopsy tissue could be helpful in predicting the prognosis for IgA nephropathy. It will be necessary in the near future to perform a prospective study with a large number of patients to validate intraglomerular TGF-β1 gene expression in IgA nephropathy as a molecular marker for disease progression.
ACKNOWLEDGMENT
This work was supported by the Brain Korea 21 project in 2002. We are grateful for the excellent technical support of Kyung Hyun Chang, PhD.
References
1. Donadio JV Jr, Grande JP. Immunoglobulin A nephropathy: a clinical perspective. J Am Soc Nephrol 1997;8:1324–1332PMID : 9259362.


2. Yang CW, Hsueh S, Wu MS, Lai PC, Huang JY, Wu CH, Hu SA, Chen JF, Huang CC. Glomerular transforming growth factor-β1 mRNA as a marker of glomerulosclerosis-application in renal biopsies. Nephron 1997;77:290–297PMID : 9375822.


3. Iwano M, Akai Y, Fujii Y, Dohi Y, Matsumura N, Dohi K. Intraglomerular expression of transforming growth factor-beta 1 (TGF-beta 1) mRNA in patients with glomerulonephritis: quantitative analysis by competitive polymerase chain reaction. Clin Exp Immunol 1994;97:309–314PMID : 8050182.



4. Niemir ZI, Stein H, Noronha IL, Kruger C, Andrassy K, Ritz E, Waldherr R. PDGF and TGF-β contribute to the natural course of human IgA glomerulonephritis. Kidney Int 1995;48:1530–1541PMID : 8544410.


5. Wada T, Hamakawa S, Hori Y, Kaname S, Shimizu S, Kurokawa K, Katoh T. Immunohistochemical localization of latent transforming growth factor-β binding protein in IgA nephropathy. Kidney Int Suppl 1997;63:S182–S184PMID : 9407453.

6. Lai KN, Ho RT, Leung JC, Lai FM, Li PK. Increases mRNA encoding for transforming growth factor-β in CD4+ cells from patients with IgA nephropathy. Kidney Int 1994;46:862–868PMID : 7996808.


7. Ihm CG, Park JK, Lee TW, Kim MJ, Cha DR. IgA aggregates stimulate monocyte chemotactic peptide-1 expression in human mesangial cells. Nephrology 2000;5:99–103.

8. Adler SG, Kang SW, Feld S, Cha DR, Barba L, Striker L, Striker G, Riser BL, LaPage J, Nast CC. Glomerular mRNAs in human type 1 diabetes: biochemical evidence for microalbuminuria as a manifestation of diabetic nephropathy. Kidney Int 2001;60:2330–2336PMID : 11737607.


9. Haas M. Histologic subclassification of IgA nephropathy: a clinicopathologic study of 244 cases. Am J Kidney Dis 1997;29:829–842PMID : 9186068.


10. Mo W, Brecklin C, Garber SL, Song RH, Pegoraro AA, Au J, Arruda JA, Dunea G, Singh AK. Changes in collagenases and TGF-β precede structural alterarions in a model of chronic renal fibrosis. Kidney Int 1999;56:145–153PMID : 10411687.


11. Isaka Y, Fujiwara Y, Ueda N, Kaneda Y, Kamada T, Imai E. Glomerulosclerosis induced by in vivo transfection of transforming growth factor-beta or platelet-derived growth factor gene into the rat kidney. J Clin Invest 1993;92:2597–2601PMID : 8254017.



12. Border WA, Noble NA, Yamamoto T, Harper JR, Yamaguchi Y, Pierschbacher MD, Ruoslahti E. Natural inhibitor of transforming growth factor-beta protects against scarring in experimental kidney disease. Nature 1992;360:361–364PMID : 1280332.


13. Yamamoto T, Nakamura T, Noble NA, Ruoslahti E, Border WA. Expression of transforming growth factor beta is elevated in human and experimental diabetic nephropathy. Proc Natl Acad Sci U S A 1993;90:1814–1818PMID : 7680480.



14. Mezzano S, Burgos ME, Olavarria F, Caorsi I. Immunohistochemical localization of IL-8 and TGF-beta in streptococcal glomerulonephritis. J Am Soc Nephrol 1997;8:234–241PMID : 9048342.


15. Sakai H, Naka R, Suzuki D, Nomoto Y, Miyazaki M, Nikolic-Paterson DJ, Atkins RC. In situ hybridization analysis of TGF-β in glomeruli from patients with IgA nephropathy. Contrib Nephrol 1995;111:107–115PMID : 7758331.


16. Yoshioka K, Takemura T, Murakami K, Okada M, Hino S, Miyamoto H, Maki S. Transforming growth factor-β protein and mRNA in glomeruli in normal and diseased human kidneys. Lab Invest 1993;68:154–163PMID : 8441250.

17. Onetti Muda A, Feriozzi S, Rahimi S, Faraggiana T. Expression of TGF-beta receptors type I and II in human glomerulonephritis. Nephrol Dial Transplant 1998;13:279–284PMID : 9509435.


18. D'Amico G. Natural history of idiopathic IgA nephropathy: role of clinical and histological prognostic factors. Am J Kidney Dis 2000;36:227–237PMID : 10922300.


19. Hirakata M, Kaname S, Chung UG, Joki N, Hori Y, Noda M, Takuwa Y, Okazaki T, Fujita T, Katoh T, Kurokawa K. Tyrosine kinase dependent expression of TGF-β induced by stretch in mesangial cells. Kidney Int 1997;51:1028–1036PMID : 9083267.


Figure 1
The effect of immune aggregates on TGF-β1 mRNA expression. TGF-β1 mRNA expression was significantly higher under the condition of IgA aggregate for 24 hrs than the control (*p<0.05).
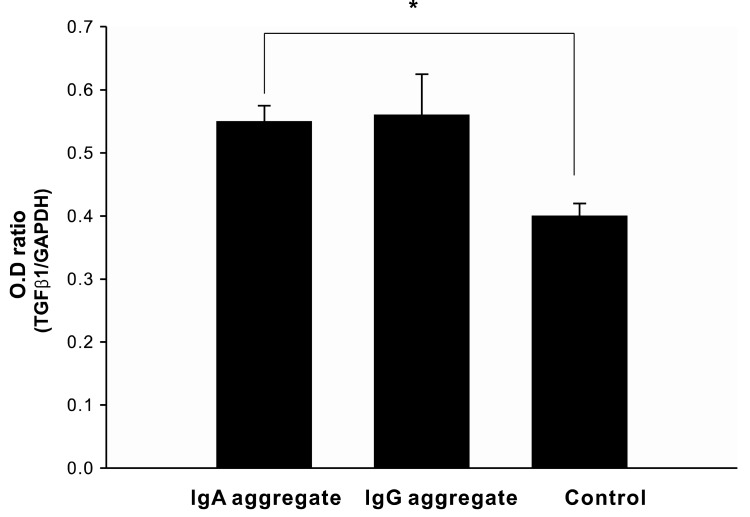
Figure 2
Effect of protein kinase C inhibition on TGF-β1 mRNA expression. (A) TGF-β1 mRNA expression was not different between the PMA treatment group and the control group. PMA pre-treatment was done for 24 hrs before each condition. (B) Calphostin C treatment did not influence on TGF-β1 mRNA expression in the IgA-treated group and IgG-treated group (black bar: without Calphostin C, gray bar: with Calphostin C).
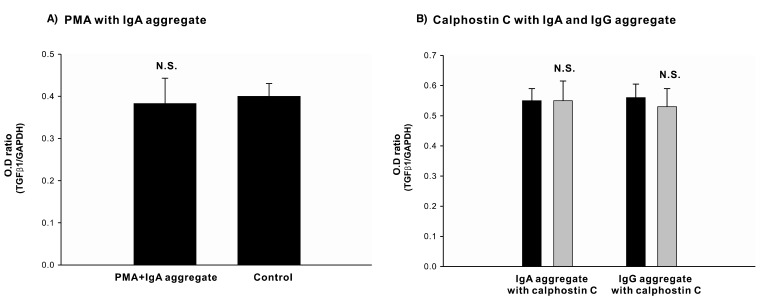
Figure 3
Quantitative analysis of TGF-β1 (A), GAPDH (B) mRNA with 1/10th of a glomerulus in patients with IgA nephropathy. Competitive PCR assays were performed by adding decreasing amount of the mutant TGF-β1 cDNA and mutant GAPDH cDNA to a series of six tubes containing a constant amount of the wild type test cDNA. The wild and mutant bands were analyzed by their size difference by the presence of a 51 and 39 bp deletion in the mutant cDNA, respectively. TGF-β1 and GAPDH PCR amplification resulted in 390 and 598 bps, respectively. PCR amplification of the mutant DNA showed 339 and 559 bps, respectively.

Figure 4
Correlation between intraglomerular TGF-β1 mRNA expression and the clinical parameters. Intraglomerular TGF-β1 mRNA expression was strongly correlated with creatinine clearance (r=-0.764, p=0.027), the amount of daily proteinuria (r=0.781, p=0.022), and the serum creatinine concentration (r=0.884, p=0.004).
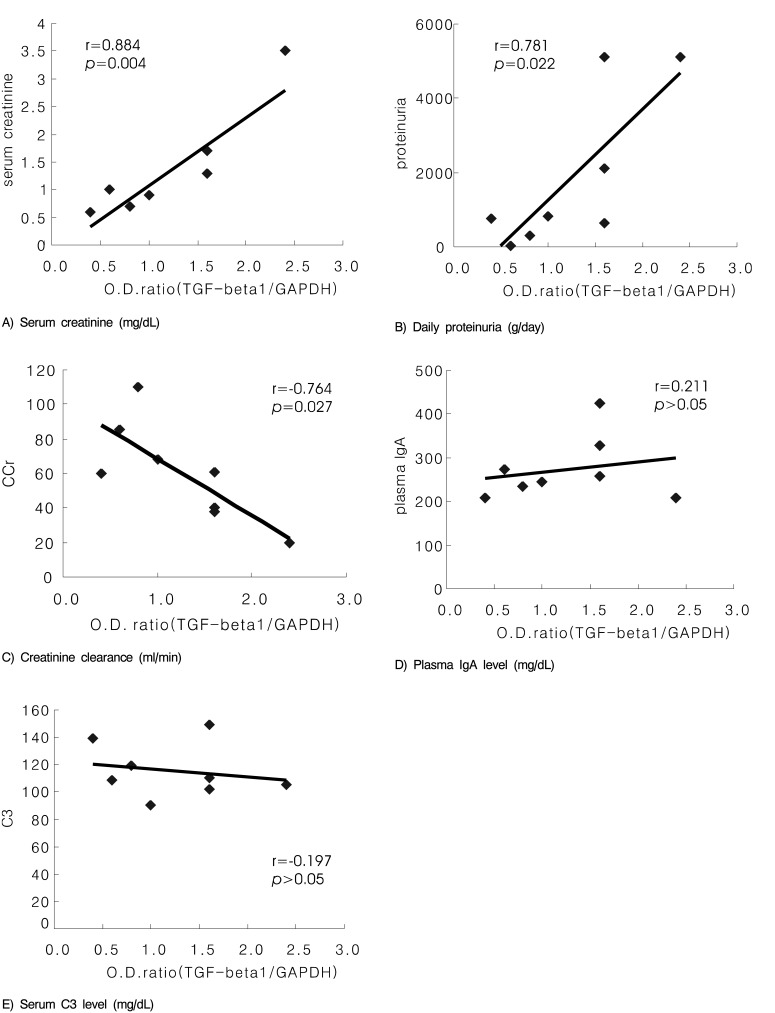
Figure 5
Correlation between the intraglomerular TGF-β1 mRNA expression and the pathologic findings. Intraglomerular TGF-β1 mRNA expression was positively correlated with the degree of tubulointerstitial changes (r=0.809, p=0.015). The degree of glomerulosclerosis showed an increased tendency for intraglomerular TGF-β1 mRNA expression, but this was statistically insignificant (r=0.646, p=0.084).



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print



