 |
 |
| Korean J Intern Med > Volume 8(2); 1993 > Article |
|
Abstract
Physical exertions are related to sudden cardiac death following acute myocardial infarction (AMI). Abnormalities in the autonomic modulation during exercise were noted in animals with AMI that were susceptible to potentially lethal arrhythmias. This study was done to evaluate the changes in the autonomic activity during exercise and recovery in AMI patients with good exercise capacity, using spectral analysis of R-R intervals of electrocardiogram (ECG). Symptom-limited treadmill exercise test was done on 17 patients of AMI with mild heart failure (in 7–10 days after the attack) and 21 healthy controls. The exercise was divided into 7 stages; rest, early exercise, mid-exercise, peak exercise, early recovery, mid-recovery, and late recovery. Power spectral analysis of R-R intervals of ECG was performed for each stage. Low frequency (0.04–0.15 Hz) and high frequency (0.15–0.40 Hz) powers, and their ratio were obtained. These parameters were observed throughout the stages in both groups. The trend of their changes during exercise and recovery was essentially the same for both groups; high and low frequency powers progressively decreased during exercise and abruptly increased during early recovery, but did not return to the values at those of rest until 9 minutes into the recovery. When the parameters were compared between the groups, there was a significantly greater decrease of high frequency power during the early exercise (p<0.05), and a higher ratio of low to high frequency power during the early recovery (p<0.05) in the patients.
These data suggest that, in AMI with low conventional risk profiles, there are abnormalities in the cardiac autonomic modulation during exercise and recovery; a greater decrease of the vagal activity during mild exercise and a greater magnitude of sympathetic predominance during the early recovery.
Spectral analysis of the heart rate provides a noninvasive clinical method for assessing the neural input to the cardiovascular system1–6). Fluctuations of the heart rate at low frequency (<0.15 Hz) can be mediated by both the vagus and the cardiac sympathetic nerves and may be related to baroreflex activity, temperature regulation, and/or maintenance of homeostasis during various cardiovascular stresses. Fluctuations at high frequency (0.15–0.40 Hz) are mediated almost entirely by the vagus and are usually directly associated with respiratory activity.
Acute myocardial infarction (AMI) is a critical manifestation of coronary artery disease. Sudden deaths frequently occur in AMI7). Actually, myocardial infarction is a major cause of sudden death7). Previous myocardial infarction could be identified in as many as 75% of sudden cardiac deaths7,8). Physical exertions were related to sudden cardiac deaths ensuing on AMI9–12). In experimental studies, abnormalities in autonomic activity were noted during exercises in animals with AMI that were known to be susceptible to ventricular fibrillation13,14). Therefore, an evaluation of the autonomic activity during exercise may have a prognostic significance in AMI.
Rapid changes in the autonomic activity during exercise have been little studied15). In the present study, we have assessed the rapid changes in autonomic nervous activity during and after exercise in AMI patients with a relatively good exercise capacity, using spectral analysis of R-R intervals of electrocardiogram (ECG).
The study population included 17 consecutive patients with AMI who could exercise for more than 9 minutes on a treadmill with the modified Bruce protocol in predischarge exercise test (7–10 days after the attack), and 21 healthy controls. The patients with AMI consisted of 15 males and 2 females. The controls were consecutively recruited from members of a local athletic club. To match their age with the patients, subjects older than 40 years of age were selected. They consisted of 11 males and 10 females. They appeared normal based on history, physical examination, routine chemistry, ECG and chest X-ray. AMI was diagnosed if 2 of the following 3 criteria were met16: (1) characteristic chest pain lasting longer than 20 minutes; (2) a sequential increase and decrease in plasma concentration of creatine phosphokinase-MB fraction; (3) development of new pathologic Q waves. Patients on digitalis and beta-blockers were not included in the study. Patients with pacemaker implantation and with arrhythmias unsuitable for the analysis of heart rate variability (HRV), such as atrial fibrillation and flutter, bundle branch block, and frequent ventricular premature contractions, also were not included.
All subjects gave informed consent and underwent symptom-limited upright exercise treadmill test. For an effective comparison of the 2 groups with different exercise capacities, different protocols were used; the modified Bruce protocol for the patients and the Bruce protocol for the controls. This approach could give a long ECG for spectral analysis of each stage in the patients. A rest before, and a recovery after the exercise, were carried out in the supine position.
Medications for the patients were withheld on the morning of the test. Three-lead ECG was cotinuously monitored before, during and after the exercise, and at each minute during exercise and recovery a 12-lead ECG was also obtained. Blood pressures were measured at rest, at the end of each exercise stage, and every 3 minutes after the exercise by the indirect cuff method. The recovery period was observed for 9 minutes after the exercise.
The end-points of the exercise were defined as angina pectoris of at least moderate severity, S-T segment depression of ≥2 mm, hypotension, ventricular tachycardia, excessive fatigue, short-ness of breath or weakness. The exercise ECG was interpreted as positive, if there was ≥1 mm S-T segment depression of the flat or downsloping variety in at least three consecutive beats at 80 msec after the J point (in the absence of baseline S-T segment changes or changes during standing and hyperventilation), or if there was ≥ 1.5 mm upsloping S-T segment depression. In patients with baseline S-T abnormalities, the exercise ECG was considered positive if there was an additional 2 mm S-T segment depression in the leads showing baseline changes.
The exercise ECG was interpreted as negative if there were no ischemic changes during exercise, provided that the patient achieved ≥85% of the maximum predicted heart rate. In patients with baseline electrocardiographic abnormalities (and no additional changes as described above) or in patients who failed to achieve 85% of maximum predicted heart rate (and no S-T depression), the exercise ECGs were interpreted as nondiagnostic (or inconclusive). Maximum workloads achieved (ml/kg/min) were calculated by the formula by Bruce et al17). They were divided by 3.5 to give the workload in METs (metabolic equivalents).
The CM1 and CM5 leads of the ECG were recorded on magnetic tape with a Marquette Holter recorder. For the spectral analysis of R-R intervals, the exercise and recovery periods were divided into 3 equal portions; early, mid-, and peak for the exercise, and early, mid-, and late for the recovery. Therefore, there were 7 stages in relation to the beginning and end of the exercise as follows: 1) rest before exercise, 2) early exercise, 3) mid-exercise, 4) peak exercise, 5) early recovery, 6) mid-recovery, and 7) late recovery. Power spectral analysis was then performed on R-R intervals of normal QRS complex for 120 consecutive seconds, using the following algorithm: Tachogram was made of R-R intervals of normal QRS complexes. When artifacts or atrial or ventricular premature complexes were encountered, the preceding and succeeding R-R intervals were excluded and replaced with the values of the next normal-to-normal coupling interval. The R-R interval function was sampled every 469 msec. Then, the mean R-R interval was subtracted from the sampled R-R interval data, a Hanning window was applied and fast Fourier transformation was computed. The data were presented after a log-transformation of the spectral powers because of their skewed distribution toward large values. If there were more than one intact 120-second “unit period” for a stage, the data of that stage was presented as the average of all the unit data. We selected the spectra between 0.04 and 0.15 Hz for the low frequency component and between 0.15 and 0.40 Hz for the high frequency component. The ratio of low to high frequency power was also calculated due to the fact that, in the presence of marked change in variance of R-R intervals, the use of the ratio is more appropriate to detect the state of the sympathovagal balance18).
Data are presented as mean±standard error. Blood pressures were not entered into the analysis because accurate measurement of blood pressure by the indirect method is difficult during the treadmill exercise. For a comparison of the heart rate, averaged heart rates for 15 seconds of each stage were used. The heart beats for the average were sampled at the end of the rest for the “rest”, at 3 minutes after the exercise for the early exercise, at mid-portion of the exercise for the mid-exercise, at the end of the exercise for the peak exercise and at the end of each recovery stage for the respective recovery stage. All the data were compared between the stages in both groups, between the control and AMI and between anterior and inferior infarctions, using the Wilcoxon signed-ranks test for the paired samples and the Mann-Witney U test for the unpaired ones. SPSS/PC+ version 4.0 was used for the analysis19). For an effective comparison of the trends between the patient group and the control, the spectral data were standardized into percentages based on the rest value (100%) since the rest values had a wide range but did not differ significantly between the 2 groups. A probability value of <0.05 was considered statistically significant.
The clinical data of both groups are listed in Table 1. There were 11 males and 10 females in the control and 15 male and 2 female patients in the AMI group. The patients consisted of 15 Q-wave and 2 non-Q wave infarctions and were divided into 8 anterior and 9 inferior infarctions. Their mean age was similar in both groups (control 52±1.5 versus AMI 53±2.4). Height and weight were also not significantly different.
The exercise test was positive in 3 of the patients. It was negative in all cases of the control. The exercise duration was similar between the 2 groups (Control 777±30.2 sec versus AMI 839±41.8 sec) even though the subjects were on different protocols-the modified Bruce protocol for the AMI and the Bruce protocol for the control. Maximum workloads achieved were much higher in the control than in the AMI, as expected (13.1±0.52 METs versus 8.7±0.68 METs, p<0.0005). The patients had a good exercise capacity with maximum work-loads being 5 to 13 METs. There was no significant difference in the resting heart rate between both groups and the changes in heart rate, during the exercise and recovery, followed the same pattern in both groups. The heart rate progressively increased during exercise (p<0.001 for control and p<0.01 for AMI, between each consecutive stage). During the early recovery, the heart rate decreased abruptly compared to that of the peak exercise (p<0.001 for both groups). Thereafter, it progressively decreased until the end of data collection (p<0.05 between early and late recoveries in both groups), but the heart rate during the late recovery was still higher than the resting value in both groups (p<0.001).
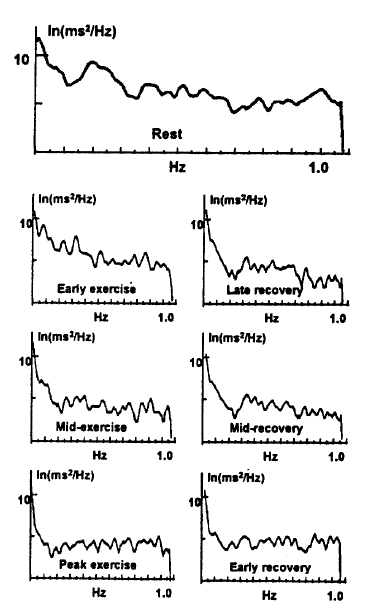
Changes in the spectral indices during exercise and recovery are presented in Table 2 and Fig. 1. During rest, there were no differences in both low and high frequency powers and their ratio between the control and AMI. As the exercise progressed, both low and high frequency powers progressively decreased until the mid-exercise in both groups, but there was no significant difference between the mid- and peak exercises in both groups. During the early recovery, the power increased abruptly compared to the peak exercise (low frequency, p<0.001 for control, p<0.01 for AMI; high frequency, p<0.05 for both groups) although it remained significantly below the resting values (low frequency, p<0.001 for control, p<0.05 for the AMI; high frequency, p<0.01 for control, p<0.05 for AMI). As the recovery progressed, the power did not increase further until the end of recovery (except for a minor increase of low frequency power during the mid-recovery in the control). There were no statistically significant differences in raw data of both spectral indices throughout all the stages between the 2 groups, with an exception of a greater low frequency power during the early recovery in the patient (p<0.05). To compare the trends of the changes between the control and the AMI groups, the data were standardized, as mentioned above (Fig. 2). The result was essentially the same as with the raw data. However, high frequency power during the early exercise decreased to a greater extent in the AMI group than in the control (p<0.05). As the exercise progressed, the indices decreased further, but the difference between the 2 groups became statistically insignificant. There was an increased low frequency power in the patients during the early recovery as compared with the control, even though it was statistically not significant (p=0.15). When the spectral indices were compared between patients with anterior and inferior infarctions, there were no differences throughout all the stages. The ratio of low to high frequency power progressively decreased during the exercise in the control (p<0.01 for the rest versus the early exercise and the early exercise versus the mid-exercise, and p<0.05 for the mid-exercise versus the peak exercise). In the AMI, the ratio decreased significantly only at the peak exercise (p<0.01). During the recovery, the ratio increased abruptly to the level at the rest in both groups. When the ratio was compared between the 2 groups, the patients had a higher value during the peak exercise (p<0.01) and the early recovery (p<0.05).
Arrhythmia is a major cause of death after myocardial infarction20). Abnormalities of the autonomic nervous system are intimately related to the genesis of the arrhythmias21,22). Factors that increase the sympathetic activity enhance the likelihood of ventricular arrhythmias, while those that decrease sympathetic nervous system decrease the likelihood. On the contrary, an increase in the parasympathetic nervous system activity tends to prevent ventricular arrhythmias, and its decrease tends to promote them. Therefore, the evaluation of the autonomic activity in patients with AMI would have a prognostic value. Recently, it has been possible to assess the cardiac modulation of autonomic nervous system noninvasively by the analysis of HRV1–6). The assessment of HRV has been used for risk stratification after AMI23–27). Low HRV is related to increased risks of cardiac events. The analysis of these HRV data would give pertinent information on the pathophysiologic role of the autonomic nervous system in cardiac arrhythmias occuring after myocardial infarction.
Exercise capacity is one of the most important predictors for subsequent cardiac events following AMI28). Since exercise capacity of more than 9 minutes on the modified Bruce protocol is roughly equivalent to more than 5 METs, it can be said that most of our patients had a good exercise capacity17). Therefore, our patients group seemed to have a good prognosis, i.e., lower risk of sudden death29,30). We evaluated the autonomic activity during exercise in these patients with low risk profile as compared with the control. Response of the autonomic nervous system during exercise were not extensively studied, especially in the patients with AMI15,31–33). Robinson et al. and Savin et al. used autonomic blocking drugs to deduce the relative roles of the sympathetic and parasympathetic activities31,32). They concluded that the principal cardiac autonomic activity during mild exercise, increased heart rate, was primarily due to a withdrawal of the vagal activity, whereas with more strenuous exercise, the increase in the heart rate was due to an increased sympathetic tone. During recovery from the exercise, the sympathetic activity decreased gradually while the vagal tone returned gradually. However they did not give any information regarding the rapid changes in the autonomic activity during physical activity and recovery. The spectral analysis of heart rate was used to assess these rapid changes in the autonomic nervous activity during and after exercise15,33). Rimoldi et al. observed the changes in HRV during exercise in young champion swimmers33). Their findings suggested that there was a marked sympathetic predominance during mild levels of exercise and an elevated sympathetic activity during recovery. The elevated sympathetic activity seemed to outlast the cessation of the exercise. Arai et al. analyzed rapid modulation of cardiac autonomic activity during exercise by the spectral analysis of heart rate, in normal subjects, in patients with severe heart failure (NYHA class III, IV), and in patients with cardiac transplantation15). The vagal activity progressively decreased during exercise and gradually increased during recovery in normal subjects, whereas there was a marked reduction of the autonomic modulation of heart rate in patients with heart failure.
The spectral analysis of heart rate could provide quantitative information about the progressive changes in the sympathovagal balance controlling heart rate from rest to moderate exercise and after its cessation33). However, there might be limitations on its application to maximal exercise due to technical uncertainties of the method during the maximal exercise33). During the maximal exercise, several factors, such as markedly reduced R-R intervals, marked rise of blood pressure, markedly increased ventilation, etc, might modify the spectral distribution of R-R intervals. As the autonomic activity of maximal exercise might not be reflected in the spectral data in our subjects, we did not attempt to assess the data of maximal exercise in terms of the autonomic activity. Although we used the fast Fourier transformation method for the spectral analysis, the changes in HRV of our normal subjects were essentially the same as others who used autoregressive method15,33). Low and high frequency powers decreased during the early exercise. During the early recovery, there were relatively abrupt increases in both frequency powers and the ratio of low to high frequency power. This reflects the predominant sympathetic activity immediately after exercise. The short-term high and low frequency powers of the patients during rest were not different from those of the control, suggesting a relatively normal pattern of cardiac autonomic activity at rest, although this short-term data may not be representative of long-term data. This is quite a contrast to the results of the study by Arai et al. on patients with severe heart failure15). There was a several decreased autonomic modulation at rest in those patients with severe heart failure. The trend of changes in HRV during exercise in our patients was also similar to that of the normal subjects. This might also be attributed to a relatively good exercise capacity of our patients. During the recovery, the trend was also similar to the control, except for low frequency power during the early recovery, with the raw data being higher in the patients. This suggests that the sympathetic predominance during this period is more intense in patients. When the standardized data were compared between the groups, the high frequency power, reflecting the vagal activity, decreased significantly more during the early exercise and the ratio of low to high frequency power was higher during the peak exercise and early recovery in AMI patients. The difference in the high frequency power was higher during the peak exercise and early recovery in AMI patients. The difference in the high frequency power during the early, mild exercise might be more evident if the fact is taken into consideration that the early exercise on the modified Bruce protocol is much milder than that on the Bruce protocol.
In conclusion, our data suggest that there are some abnormalities of cardiac autonomic modulation in patients of AMI with a good exercise capacity; a greater decrease of the vagal activity at low level exercise and a greater magnitude of sympathetic predominance during early recovery. This may be a good substrate for cardiac arrhythmias following AMI. However, the prognostic significance of this finding should be further studied.
Fig. 2.
Comparison of standardized data of low and high frequency powers, and their ratio between the patients with acute myocardial infarction (AMI) and the control. Note a greater decrease in high frequency power during the early exercise and a higher ratio of low to high frequency powers during the peak exercise and the early recovery in the patients. E-EX=early exercise; E-RE=early recovery; L-RE=late recovery; M-EX=mid-exercise; M-RE=mid-recovery; P-EX=Peak exercise. *p<0.05 versus control; **p<0.01 versus control.
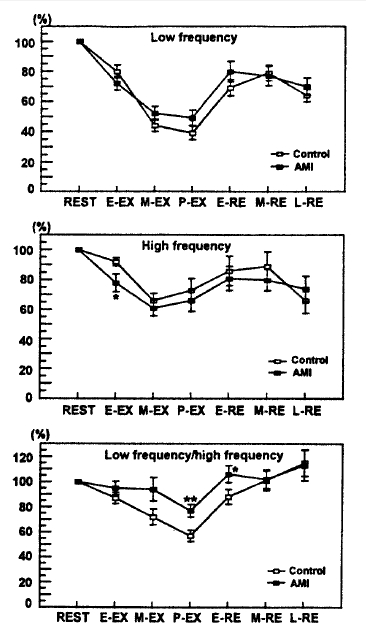
Table 1.
Clinical Data of the Control and the AMI
| Control (n=21) | AMI (n=17) | |
|---|---|---|
| Age (Years) | 52±1.5 | 53±2.4 |
| Sex (male/female) | 11/10 | 15/2 |
| Height (cm) | 163±1.7 | 166±1.7 |
| Weight (kg) | 63±1.7 | 65±1.8 |
| Ex duration (sec) | 777±30.2 | 839±41.8 |
| Max workload (METs) | 13.1±0.52 | 8.7±0.68* |
Table 2.
Heart rate and power spectral data in the control (n=21) and AMI (n=17)
|
Heart rate
|
Low frequency (LF)
|
High frequency (HF)
|
LF/HF
|
|||||
|---|---|---|---|---|---|---|---|---|
| Control | AMI | Control | AMI | Control | AMI | Control | AMI | |
| Rest | 71±1.5 | 67±3.7 | 4.77±0.25 | 5.21±0.32 | 3.85±0.28 | 4.02±0.31 | 1.32±0.07 | 1.32±0.06 |
| Exercise | ||||||||
| Early | 99±3.93 | 97±3.63 | 3.78±0.293 | 3.75±0.322 | 3.49±0.262 | 3.11±0.282 | 1.10±0.052 | 1.22±0.06 |
| Mid | 122±3.73 | 104±3.63 | 2.07±0.193 | 2.68±0.252 | 2.35±0.163 | 2.28±0.192 | 0.89±0.072 | 1.20±0.10 |
| Peak | 173±2.33 | 143±4.93 | 1.80 ±0.18 | 2.45±0.27 | 2.47±0.17 | 2.45±0.23 | 0.71±0.0441 | 0.99±0.061 |
| Recovery | ||||||||
| Early | 102±2.73 | 88±4.43 | 3.13±0.193 | 4.05±0.382 | 2.96±0.211 | 3.04±0.301 | 1.10±0.053 | 1.36±0.073 |
| Mid | 94±2.1+ | 83±3.9+ | 3.63±0.19+ | 3.96±0.38# | 3.03±0.21* | 3.05±0.29* | 1.26±0.07 | 1.32±0.08 |
| Late | 93±1.9+ | 81±3.6+ | 3.02±0.21+ | 3.59±0.33# | 2.26±0.23+ | 2.70±0.28# | 1.44 ±0.11 | 1.45±0.13 |
REFERENCES
1. Katona PG, Jih F. Respiratory sinus arrhythmia: noninvasive measure of parasympathetic cardiac control. J appl Physiol 39:801. 1975.


2. Akselrod S, Gordon D, Ubel FA, Shannon DC, Barger AC, Cohen RJ. Power spectrum analysis of heart rate fluctuation: a quantitative probe of beat-to-beat cardiovascular control. Science 213:220. 1981.


3. Fouad FM, Tarazi RC, Ferrario CM, Fighaly S, Alicandri C. Assessment of parasympathetic control of heart rate by a non-invasive method. Am J Physiol 246:H838. 1984.


4. Pomeranz B, Macaulay RJB, Caudill MA, Kutz I, Adam D, Gordon D, Kilborn KM, Barger AC, Shannon DC, Cohen RJ, Benson H. Assessment of autonomic function in humans by heart rate spectral analysis. Am J Physiol 248:H151. 1985.


5. Akselrod S, Gordon D, Madwed JB, Snidman NC, Shannon DC, Cohen RJ. Hemodynamic regulation: investigation by spectral analysis. Am J Physiol 249:H867. 1985.


6. Pagani M, Lombardi F, Guzzetti S, Rimoldi O, Furlan R, Pizzinelli P, Sandrone G, Malfatto G, Dell'Orto S, Piccaluga E, Turiel M, Baselli G, Cerutti S, Malliani A. Power spectral analysis of heart rate and arterial pressure variabilities as a marker of sympatho-vagal interaction in man and conscious dog. Circ Res 59:178. 1986.


7. Kannel WB, Doyle JT, McNamara PM, Quickenton P, Gordon T. Precursors of sudden coronary death: factors related to the incidence of sudden death. Circulation 51:606. 1975.


8. Goldstein S. The necessity of a uniform definition of sudden coronary death: Witnessed death within 1 hour of the onset of acute symptoms. Am Heart J 103:156. 1982.


9. Paffenbarger RS Jr, Hale WE, Brand RJ, Hyde RT. Work-energy level, personal characteristics, and fatal heart attack: A birth-cohort effect. Am J Epidemiol 105:200. 1977.


11. Weaver WD, Cobb LA, Hallstrom AP. Characteristics of survivors of exertion- and nonexertion-related cardiac arrest: Value of subsequent exercise testing. Am J Cardiol 50:671. 1982.


12. Ciampricotti R, Taverne R, Gamal ME. Clinical and angiographic observations on resuscitated victims of exercise-related sudden ischemic death. Am J Cardiol 68:47. 1991.


13. Billman GE, Schwartz PJ, Gagnol JP, Stone HL. Cardiac response to submaximal exercise in dogs susceptible to sudden cardiac death. J Appl Physiol 59:890. 1985.


14. Billman GE, Hoskins RS. Time-series analysis of heart rate variability during submaximal exercise. Evidence for reduced cardiac vagal tone in animals susceptible to ventricular fibrillation. Circulation 80:146. 1989.


15. Arai Y, Saul JP, Albrecht P, Hartley LH, Lilly LS, Cohen RJ, Colucci WS. Modulation of cardiac autonomic activity during and immediately after exercise. Am J Physiol 256:H132. 1989.


16. Goldberg RJ, Gore JM, Alpert JS, Dalen JE. Recent changes in attack and survival rates of acute myocardial infarction (1975 through 1981). The Worcester Heart Attack Study. JAMA 255:2774. 1986.


17. Bruce RA, Kusumi F, Hosmer D. Maximal oxygen intake and nomographic assement of functional aerobic impairment in cardiovascular disease. Am Heat J 85:546. 1973.

18. Malliani A, Pagani M, Lombardi F, Cerutti S. Cardiovascular neural regulation explored in the frequency domain. Circulation 84:482. 1991.


19. Norusis MJ. SPSS/PC+Statistics 4.0. B49–B66Chicago: SPSS Inc, 1990.
20. Marcus FI, Cobb LA, Edwards JE, Kuller L, Moss AJ, Bigger JT Jr, Fleiss JL, Rolnitzky L, Serokman R, Multicenter Post Infarction Research Group. Mechanism of death and prevalence of myocardial ischemic symptoms in the terminal event after acute myocardial infarction. Am J Cardiol 61:8. 1988.


22. Schwartz PJ, La Rovere MT, Vanoli E. Autonomic nervous system and sudden cardiac death. Circulation 85:177. 1992.

23. Kleiger RE, Miller JP, bigger JT Jr, Moss AJ, the Multicenter Post-Infarction Research Group. Decreased heart rate variability and its association with increased mortality after acute myocardial infarction. Am J Cardiol 59:256. 1987.


24. Lombardi F, Sandrone G, Pernpruner S, Sala R, Garimoldi M, Cerutti S, Baselli G, Pagani M, Malliani A. Heart rate variability as an index of sympathovagal interaction after acute myocardial infarction. Am J Cardiol 60:1239. 1987.


25. Rich MW, Saini JS, Kleiger RE, Carney RM, teVelde A, Freedland KE. Correlation of heart rate variability with clinical and angiographic variables and late mortality after coronary angiography. Am J Cardiol 62:714. 1988.


26. Casolo GC, Stroder P, Signorini C, Calzolari F, Zucchini M, Balli E, Sulla A, Lazzerini S. Heart rate variability during the acute phase of myocardial infarction. Circulation 85:2073. 1992.


27. Bigger JT Jr, Fleiss JL, Steiman RC, Rolnitzky LM, Kleiger RE, Rottman JN. Correlations among time and frequency domain measures of heart period variability two weeks after acute myocardial infarction. Am J Cardiol 69:891. 1992.


28. Hamm LF, Crow RS, Stull GA, Hannan P. Safety and characteristics of exercise testing early after acute myocardial infarction. Am J Cardiol 63:1193. 1989.


29. Weld FM, Chu KL, Bigger TJ Jr, Rolnitzky LM. Risk stratification with low level exercise testing 2 weeks after acute myocardial infarction. Circulation 64:306. 1981.


30. DeBusk RF, Blomqvist CG, Kouchoukos NT, Luepker RV, Miller HS, Moss AJ, Pollock ML, Reeves TJ, Selvester RH, Stason WB, Wagner GS, Willman VL. Identification and treatment of low-risk patients after acute myocardial infarction and coronary-artery bypass graft surgery. New Engl J Med 314:161. 1986.


31. Robinson BF, Epstein SE, Beiser GD, Braunwald E. Control of heart rate by the autonomic nervous system. Studies in man on the interrelation between baroreceptor mechanisms and exercise. Circ Res 19:400. 1966.


-
METRICS

-
- 0 Crossref
- 2 Scopus
- 8,926 View
- 28 Download
- Related articles



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print


