 |
 |
| Korean J Intern Med > Volume 16(1); 2001 > Article |
|
Abstract
Systemic lupus erythematosus(SLE) is a prototypic autoimmune disease affecting various organ systems. Hypothermia is a rare manifestation of SLE. We experienced a case of SLE combined with hypothermia.
A 36-year-old woman, who had been diagnosed as SLE 3 days before admission, admitted complaining of mental confusion. After admission, her body temperature, initially 36.1°C, became 32.6°C. Her core body temperature was less than 35.0°C. Despite of warming with heating lamp and blankets, her core temperature did not reach 35.0°C during 18 hours. Ten days later, her temperature exceeded 36.0°C.
Systemic lupus erythematosus(SLE) is a prototypic autoimmune disease involving pathogenic autoantibody formation and immune complex deposits in various organ systems, including kidney, lung, pleura, skin, joints, heart, blood vessel and nervous system1–2). Constitutional symptoms, such as malaise, fatigue, fever, anorexia and weight loss are common presenting features of SLE. Hypothermia is a very rare symptom associated with SLE. We experienced a case of hypothermia during a flare of SLE.
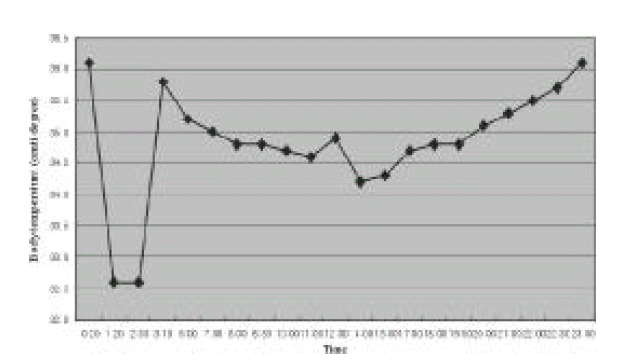
A 36-year-old woman was admitted complaining of mental confusion. Her past medical history was not remarkable. Her niece had been diagnosed as SLE 3 years ago. Three months before admission, she had mild fever, arthralgia and myalgia. Three days before admission, therapy with methylprednisolone, 125 mg BID intravenous injection, was initiated at another hospital under the diagnosis of SLE manifesting high fever reaching 40.0°C, myalgia, arthralgia, oral ulcer and facial rash. At admission, she presented personal and time disorientation and generalized edema. Her vital signs were as follows: blood pressure 90/70 mmHg, pulse rate 60/minute, respiration rate 20/minute. At the emergency room, her initial temperature was 36.1°C. One hour later, her body temperature became 32.6°C by electronic thermometer on the axilla. By mercurial thermometer, she was less than 35.0°C. Rectal temperature was also less than 35.0°C. Despite active external rewarming using heat lamp and heating blankets, her body temperature maintained less than 35°C for nearly 18 hours (Figure 1). From the third to 10th hospital day, her core temperature was between 35.0°C and 36.0°C. Thereafter, her body temperature maintained between 35.0°C and 38.3°C.
Laboratory results were as follows: total leukocyte count 800/mm3 (differential count 64.7% neutrophils, 28.5% lymphocytes, 5.6% monocytes), hemoglobin 6.1 gm/dL, platelet count 62,000/mm3, erythrocyte sedimentation rate 42 mm/hour, antinuclear antibody strong positive(1:1280) exhibiting homogenous pattern, anti-dsDNA antibody negative, anti-Sm antibody negative, anti-Ro antibody positive, antihistone antibody positive, antiribosomal P positive, anticardiolipin antibody(IgM and IgG) positive, antiphospholipid antibody positive, direct Coombs’ test positive, C3 16 mg/dL(88–201 mg/dL), C4 <10mg/dL (16–47 mg/dL), C-reactive protein 0.7 mg/dL, serum glucose 486 mg/dL, BUN 37.0 mg/dL, creatinine 2.1 mg/dL, total protein 5.8 gm/dL, albumin 2.3 gm/dL, serum ferritin 1971 ng/dL, aPTT 48.8 second (25.0–40.0 second), VDRL positive, FTA-ABS negative, serum osmolality 305 mOsm/Kg (288–302 mOsm/Kg), urine osmolality 264 mOsm/Kg (300–900 mOsm/Kg), normal serum cortisol and thyroid function tests. Blood and urine cultures resulted in no growths. Urinalysis revealed proteinuria and hematuria. Total 3,242 mg of urine protein was excreted during 24 hours.
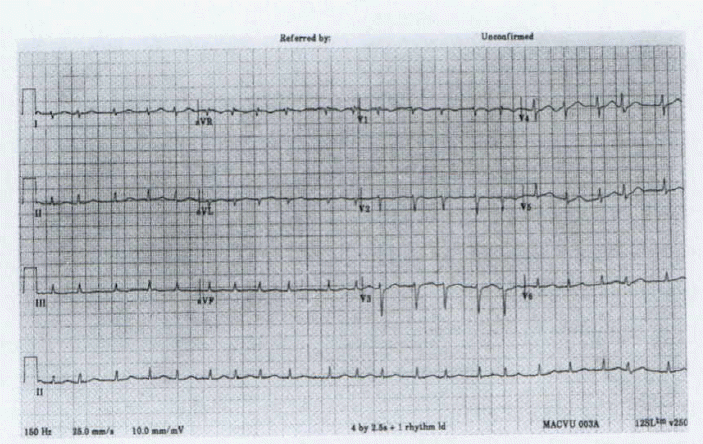
Abdominal ultrasonography showed borderline splenomegaly and increased corticomedullary echogenicity suggesting medical renal disease. Echocardiography showed only minimal pericardial effusion. Brain magnetic resonance image (MRI) and proton magnetic resonance spectroscopy (MRS) were normal. Electrocardiogram that was initially normal showed atrial fibrillation on the second hospital day (figure 2) without Osborne wave, which was subsequently normalized from the next day.
Attempt to elevate her temperature using heating blanket and heating lamp continued from the first hospital day to 11th day when fever reaching 38.3°C developed. From the first hospital day, 1,000 mg/day of pulsed methylprednisolone intravenous injection was done for 5 consecutive days and subsequently high dose prednisolone (60 mg/day) therapy was continued. Then, six cycles of monthly cyclophosphamide pulsed infusion were performed while tapering steroid dosage. Thereafter, her general condition was improved.
Hypothermia is defined as a core body temperature of 35.0°C (95.0°F) or below. It can have several causes and is usually multifactorial in origin. In healthy persons, extreme environmental conditions can cause hypothermia. However, most severe hypothermia occurs in patients with underlying medical conditions that lead to excessive heat loss or inadequate heat production, and both processes are usually involved. Medical conditions that cause hypothermia via inadequate heat production include malnutrition, hypothyroidism, adrenal insufficiency, hepatic failure, diabetic ketoacidosis, sepsis, uremia, hypothalamic dysfunction and some medications3,4).
Our patient had no evidence of medical conditions causing hypothermia. Her lupus activity was considered in flare because of high antinuclear antibody titer, low complement level, severe leukopenia, heavy proteinuria and altered mental state. Because the brain MRI and MRS were normal, but antiribosomal P was expressed positively, it was difficult to discriminate the cause of the patient’s mental change whether it was resulted from hypothermia itself or neurologic manifestation of SLE. Laboratory abnormalities such as hyperglycemia, high serum osmolality, low serum osmolality were considered as the results of hypothermia. Transient electrocardiographic change (atrial fibrillation) was developed on the second hospital day when her temperature maintained between 35.2°C and 35.8°C. We supposed that this arrhythmia was derived from hypothermia because it did not appear after her temperature became normal. Characteristic Osborne wave usually appearing in moderate to severe hypothermia3) was not detected.
Flared SLE manifests general symptoms including fever, arthralgia and myalgia in most cases. Hypothermia associated with SLE has been described in only 4 patients5,6).
In the first report, Kass7) described a 32-year-old man with a generalized rash who developed marked hypothermia (as low as 87.8°F) after the administration of high doses of cortisone. In the second report, Johnson8) described a 38-year-old woman with SLE who was given cortisone. On the second day of treatment her temperature dropped precipitously to 93.4°F. In the third case of hypothermia and SLE reported by Csuka9), a 23-year-old woman is described with various manifestations of SLE. She had the onset of hypothermia below 95°F with depression of mentation and dysarthria at about 24 hours after the initial prednisone dose. The authors postulated a block in the stimulation of her peripheral cold receptors by the diffuse rash that continued to stimulate peripheral warm receptors prohibiting the central recognition of hypothermia. In the last report by Kugler6), an 18-year-old woman with SLE was presented with an exacerbation of polymyositis and neuropsychiatric symptoms. After starting prednisone she became hypothermic for 5 days. All cases occurred within 48 hours after the institution of corticosteroids therapy. In our case, it is uncertain that the corticosteroids therapy would provoke hypothermia because the steroid therapy was initiated more than 48 hours before the onset of hypothermia. What specific role, if any, steroids have in modulating thermoregulation is unclear until now10,11).
In 4 cases of hypothermia associated with SLE, including our patient, neuropsychiatric manifestations, such as basal ganglia signs, cranial neuropathy, psychomotor retardation and disorientation were evident. In neuropsychiatric SLE, a vasculopathy of cerebral blood vessels has traditionally been thought to be the underlying pathology8,12). Based on the postmortem pathology, Johnson8) reported that microvascular pathology in the brain was suggested as an underlying mechanism of the hypothermia. Although all cases were not confirmed by pathology, neuropsychiatric symptoms secondary to microvascular change of the brain may contribute to the development of hypothermia.
In summary, hypothermia may develop as a neuropsychiatric manifestation of SLE and corticosteroids therapy may have a role for hypothermia.
References
1. Hahn BH. Systemic lupus erythematosus. In: Fauci AS, Braunwald E, Isselbach KJ, Wilson JD, Martin JB, Kasper DL, Hauser SL, Longo DL, eds. Harrison’s textbook of medicine. 14th ed. 1874–1880New York: McGraw-Hill, 1998.

2. Gladman DD, Urowitz MB. Systemic lupus erythematosus: Clinical features. In: Klippel JH, Dieppe PA, eds. Rheumatology. 2nd ed. 7.1.1–7.1.18London: Mosby, 1998.
3. Ernest Y. Disorders due to heat and cold. In: Bennett JC, Plum F, eds. Cecil textbook of medicine. 20th ed. 501–503Philadelphia: WB Saunders, 1996.
4. Petty KJ. Hypothermia. In: Fauci AS, Braunwald E, Isselbach KJ, Wilson JD, Martin JB, Kasper DL, Hauser SL, Longo DL, eds. Harrison’s textbook of medicine. 14th ed. 97–99New York: McGraw-Hill, 1998.
5. Buyon JP, Wallace DJ. The endocrine system, use of exogenous estrogens and the urogenital tract. In: Wallace DJ, Hahn BH, eds. Dubois’ lupus erythematosus. 5th ed. 817–834Baltimore: Williams and Wilkins, 1997.
6. Kugler SL, Costakos DT, Aron AM, Spiera H. Hypothermia and systemic lupus erythematosus. J Rheumatol 17:680–6811990.

8. Johnson RT, Richardson EP. The neurological manifestations of systemic lupus erythematosus. Medicine 47:337–3691968.


9. Csuka ME, McCarty DJ. Transient hypothermia after corticosteroids treatment of subcutaneous lupus erythematosus (letter). J Rheumatol 11:112–1131984.

10. Boulant JA, Dean JB. Temperature receptors in the central nervous system. Ann Rev Physiol 48:639–6541986.

-
METRICS

- Related articles
-
The evaluation of cellular immune function in elderly patients with systemic lupus erythematosus



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print


