Standardized, musculoskeletal ultrasonographic reference values for healthy Korean adults
Article information
Abstract
Background/Aims
To define standard reference values for musculoskeletal ultrasonography (MSUS) in Korea.
Methods
A total of 251 healthy adults were recruited for this study. Ultrasonography was performed by experienced rheumatologists who had undergone four appropriate training programs in Korea. A General Electric LOGIQ electronic ultrasound device fitted with a 12 MHz linear transducer was employed. Mean values ± standard deviations (SDs) were defined as standard reference values. Intraclass correlation coefficients was employed to evaluate the extent of inter- and intraobserver agreement when MSUS measurements were made.
Results
The 251 study participants included 122 males. Mean subject age was 28.6 years. The average bone-to-capsule distance of the right-side second and third metacarpophalangeal (MCP) joints were 0.68 and 0.72 mm respectively, and those of the left-side joints 0.62 and 0.68 mm. The cartilage thicknesses of the right-side second and third MCP joints were 0.55 and 0.55 mm, and those of the left-side joints were 0.55 and 0.56 mm, respectively. The bone-to-capsule distances of the right and left wrists were 0.80 and 0.82 mm. In 12.4% of participants (31/251), the erosion score of the humeral head was 1.71. In the right-side knee joint, mean cartilage thicknesses of the medial and lateral condyles were 1.86 and 2.03 mm in longitudinal scans. High overall interobserver agreement was evident after appropriate training that included instruction on standard MSUS methodology.
Conclusions
We defined standard reference values for MSUS in healthy Korean adults. The reliabilities of interobserver agreements were high after appropriate training program.
INTRODUCTION
Musculoskeletal ultrasonography (MSUS) is an emerging modality used to evaluate cartilage pathology, osteoarthritis (OA), and inflammatory synovitis [1,2]. Reliable application of MSUS requires knowledge of the normal articular anatomy and its variation. Assessment of cartilage thickness is important when distinguishing between normal and pathological conditions, evaluating the severity, monitoring disease progression during long-term follow-up, and assessing the efficacy of disease-modifying OA drugs [3]. As the numbers of clinical trials employing MSUS increase, appropriate assessment of articular cartilage morphology and periarticular status is becoming more important. Although some studies have used MSUS to image both pathological and normal articular lesion, normal reference values for Koreans are not yet available [4,5]. We evaluated various articular lesions of healthy adults to derive standard reference values for healthy Koreans.
METHODS
Subjects
We evaluated 251 healthy volunteers including medical students. All volunteers gave medical histories and underwent physical examinations. We excluded those aged under 20 or over 60 years, and those with any history of inflammatory rheumatic disease, OA, trauma, or surgery on any of the joints investigated. This research complied with the Helsinki Declaration. Informed consent was obtained from all enrolled participants. The same informed consent form (ICF) and study protocol were provided to the independent Institutional Review Boards/Ethics Committees (IRB/EC) at each medical center (AJIRB-MED-OBS-10-190), and each IRB/EC reviewed the appropriateness of the protocol, and benefits to the study participants. Ultimately, the IRB/EC independently approved this study without revision of the ICF or study protocol.
Ultrasonography training program
All examinations were performed using a LOGIQ e-ultrasound machine (General Electric, Munich, Germany) fitted with a 12 MHz linear array transducer. The B-mode transducer frequencies varied by the size of the joint examined. Since the magnifying power of measurement is not specified, the scanner settings were set same for all institutions. Joints to be evaluated were selected based on their clinical significance in rheumatological practice (thus, the hands, wrists, dominant shoulder, and dominant knee) and were evaluated by reference to the standards recommended by the European League Against Rheumatism (EULAR) [4,6]. MSUS was performed by experienced rheumatologists who had undergone four MSUS training programs including education on standard scanning of all active joints [7]. In addition, all evaluators underwent a standardized examination evaluating MSUS knowledge and the skills required to use advanced equipment to obtain high-quality images and reliable scans [7-10]. The curriculum covered the standardized scanning methods for eight peripheral joints (the second and third metacarpophalangeal [MCP] joints; both wrists; the right shoulder; and the right knee) [6]. The courses were run six times in 2009 to 2010. All investigators attended at least four of these compulsory education programs.
Bone-to-capsule distance and assessment of hand and wrist cartilage
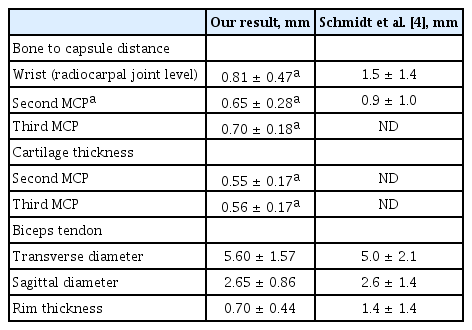
MSUS was performed using a standard scanning method [4-7]. The investigator sat in front of the subject while evaluating the hands and fingers. The subject placed the hand on top of his/her thigh, with supination when a volar scan was conducted and with pronation when the wrist was scanned dorsally. The bone-to-capsule distances of MCP joints were measured at the sharp margins of proximal side in MCP bones (Fig. 1A). The wrist bone-to-capsule distance was measured at the level of the scaphoid bone 1 cm distal to the radiocarpal joint (Fig. 1B) [4]. To evaluate interobserver agreement, the bone-to-capsule distances were also measured on images saved, in a blinded manner, 1 month after all other data had been collected by another investigator.

Methods used for musculoskeletal ultrasonography scanning of the hands and wrists. (A) The bone-to-capsule distance was measured at the sharp margins of proximal lesions in metacarpophalangeal (MCP) bones (arrow). (B) In the wrist, they were measured at the level of the scaphoid bone 1 cm distal from the radiocarpal joint (arrow). (C) The thickness of cartilage in the MCP joint was measured perpendicular to the sharp margin of the proximal lesion in MCP bone (arrow).
Longitudinal, hand articular status was evaluated only at the dorsal aspects of the second and third MCP joints with those joints in maximum flexion. The transducer was held at a 90° angle to the cartilage surface. The thickness of cartilage in the MCP joint was measured perpendicular to the sharp margin of the proximal lesion in MCP bone (Fig. 1C). When it was impossible to derive due to severe loss of cartilage or the sharpness of the cartilage surface, the data were recorded as unmeasurable.
Biceps tendon and humeral joint assessment via MSUS
When the shoulders were evaluated, the subject sat with 90° flexion of the elbow. The investigator checked the biceps tendon in the neutral position, the thickness of cartilage in the humeral head at maximum internal rotation, and infraspinatus tendon status at 60° of internal rotation [4]. The transverse diameter of the biceps (longhead) tendon was defined as the longest diameter in the transverse scan, and the perpendicular transverse diameter was the sagittal diameter of the tendon (Fig. 2A). The extent of the hypoechoic rim around the biceps tendon was measured at the point of maximum tendon diameter in the longitudinal scan (Fig. 2B). The thickness of cartilage in the humeral head was measured perpendicular to the sharp margin of the transverse scan when internal rotation was maximal (Fig. 2C). When it was impossible to measure cartilage thickness because of severe loss of sharpness of the cartilage surface, the data were recorded as unmeasurable. Humeral head erosion was checked under internal rotation, where erosion was defined as disruption of bony surface continuity > 1 mm in diameter evident in two directions of scanning. The diameter of any erosion was recorded as that at the site of maximal erosion (Fig. 2D). The thickness of cartilage in the glenohumeral joint was measured at both the infraspinatus and axillary levels. The thickness below the level of the infraspinatus was checked with the joint at 60° of internal rotation and with the other shoulder restrained (Fig. 2E). The thickness of cartilage in the axillary recess was measured at the middle of the humeral head concavity (Fig. 2F).

Musculoskeletal ultrasonography shoulder evaluation. (A) The biceps (long-head) tendon was measured in the neutral position. The transverse diameter was the longest diameter noted in the transverse scan, and the perpendicular transverse diameter was the sagittal diameter of the tendon (arrows). (B) The hypoechoic rim of the biceps tendon was measured at the point of maximum tendon diameter in the longitudinal scan (arrows). (C) The thickness of cartilage in the humeral head (arrows) was measured perpendicular to the sharp margin of the transverse scan when internal rotation was in play. (D) ‘‘Erosion’’ was defined as a disruption of bone surface continuity of 1 mm or more in the two-scan direction. The erosion diameter was recorded at the site of maximal erosion. (E) The thickness of cartilage in the glenohumeral joint was measured below the infraspinatus (arrows). (F) The thickness of cartilage in the axillary recess was measured at the middle of the humeral head concavity (arrows).
Knee joint assessment via MSUS
The cartilage of the medial and lateral femoral condyles was examined with the subjects in the supine position under maximum flexion of the knee joints. The thickness was the distance from the thin hyperechoic line at the synovial space-cartilage interface to the sharp hyperechoic line at the cartilage-bone interface [11]. The maximal thicknesses of both the medial and lateral femoral condyles were measured in both the suprapatellar transverse axial and longitudinal sagittal planes. In the suprapatellar transverse plane, the thicknesses of the medial and lateral femoral condyles were measured on the transverse line immediately above the patella (Fig. 3A). In the longitudinal plane, the thicknesses were obtained by continuously moving the probe along the midlines of the medial and lateral condyles (Fig. 3B). When it was impossible to obtain measurements due to severe loss of the sharpness of the cartilage surface, the data were recorded as unmeasurable. To evaluate intraobserver agreement, thicknesses were measured (in a blinded manner) from images taken 1 month after all data were collected. The sagittal diameter of the suprapatellar recess was the maximum longitudinal diameter at the midline of the longitudinal suprapatellar scan (Fig. 3C).
Methods used for musculoskeletal ultrasonography scanning of the knee. (A) Suprapatellar transverse scanning (coronal view) of the femoral condyle was performed under maximum flexion of the knee joint with the subject in the supine position. Cartilage thickness was measured at the suprapatellar level at the midpoints of the femoral condyles (arrows). We measured only maximum thicknesses. (B) A longitudinal scan (affording a sagittal view) of the femoral condyle was taken under the same conditions and we measured cartilage thickness at the mid-line of the condyle within a range of aberration of ± 0.5 cm. The probe was placed anteriorly to the condyle and then moved posteriorly along the mid-line of the condyle to detect the weight-bearing area (arrows). (C) The sagittal diameter of the suprapatellar recess was measured at the maximal longitudinal diameter of the midline, longitudinal suprapatellar scan (arrows).
Statistical analysis
Statistical analyses were performed using SPSS version 12 for Windows (SPSS Inc., Chicago, IL, USA) software. Continuous data are expressed as mean ± SD and categorical data are presented as percentages. The extents of interobserver agreement were estimated by calculating intraclass correlation coefficients (ICCs) [12].
RESULTS
A total of 251 healthy volunteers were enrolled (mean age, 28.6 years; 122 male) (Table 1). Eight joints were evaluated by 11 expert rheumatologists using the same standard scanning method. Tables 2-5 show the mean values of measurements. We defined standard reference values as those lying within 2 SDs.
Average of bone-to-capsule distance in the hand and wrist
Table 2 shows the average maximum bone-to-capsule distances of both the second and third MCP joints at the volar proximal aspects of those joints. They were 0.68 ± 0.37 and 0.72 ± 0.19 mm for the right side and 0.62 ± 0.17 and 0.68 ± 0.17 mm for the left side, respectively. The bone-to-capsule wrist measurements were made at the level of the radiocarpal joint. They were 0.80 ± 0.33 for the right and 0.82 ± 0.66 mm for the left side. This distance was much greater in males than in females.
Average hand cartilage thicknesses
The cartilage thicknesses of both MCP joints could be measured in all but one subject. In that subject, it could not be measured because the line at the interface of the synovial space-cartilage could not be delineated at any point on the surface. Table 3 shows the average thicknesses of both the second and third heads of the MCP joints. These were measured from the dorsal aspect with all subjects forming weak fists.
Average biceps tendon measurements and joint anatomy in the right shoulder
The mean transverse and sagittal diameters of the long head of the biceps tendon were 5.60 ± 1.57 and 2.65 ± 0.86 mm, respectively. Table 4 shows the cartilage thicknesses of the humeral head and the glenohumeral joint (both below the infraspinatus and at the level of the axillary recess). We detected humeral head erosion of over 1 mm in 31 subjects (12.4%). The mean erosion score was 1.71. The mean erosion was greater in males than in females (2.00 mm vs. 1.31 mm).
Average thickness of cartilage in the right knee
Knee cartilage thickness was easily measured in our healthy subjects via both suprapatellar transverse and longitudinal MSUS. In the suprapatellar transverse scan, it was usually difficult to delineate the line at the synovial space-cartilage interface; thus, we could not distinguish the maximum from the minimum thickness. Therefore, only the minimum thickness was measured on such scans. However, both the maximum and minimum thicknesses could be measured in longitudinal scans. Hence, the minimum thicknesses measured in the suprapatellar transverse and longitudinal MSUS scans were compared. We checked the minimum thickness of the weight-bearing area in the longitudinal scan. The cartilage thickness in longitudinal MSUS scans was less than that in transverse scans (Table 5).
Interobserver agreement when measuring bone-tocapsule distance and cartilage thickness
There overall interobserver agreements for both the bone-to-capsule distance in the MCP joints and the thickness of cartilage in the right knee joint were high (Table 6). The ICCs ranged from 0.667 to 0.971.
DISCUSSION
MSUS is becoming an essential rheumatological tool and the technique is developing rapidly worldwide [2,6,13]. MSUS is an easily accessible diagnostic tool and a therapeutic option in patients with inflammatory arthritis including rheumatoid arthritis (RA) and OA [14,15]. Although most articular fluid is distributed throughout the joint recesses, the joint spaces between the articular surfaces are relatively small in healthy people [3]. High-resolution ultrasonography allows one to assess fine details in anatomical structures [5]. The practice of MSUS is associated with several important issues including basic technical requirements, scanning techniques, clinical applications, training, and future investigations. As many difficulties may be encountered when interpreting images, both a thorough study of normal anatomy and a standardized method of evaluation are essential components of rheumatology training curricula [4,9]. Only a few studies have published standard reference values for select anatomical joint regions [4,9]. Relatively little is known about standard reference values in Asians, including Koreans. Racial differences in standard reference values are to be expected. We sought to define standard reference values (means with SDs) in normal Koreans; these may be useful when MSUS is applied in other countries.
We defined bone-to-capsule reference distances for the second and third MCPs, both radiocarpal joints, and the right glenohumeral joint. The values were lower in females than in males, and all values were somewhat lower than those of Westerners. Compared with previous studies [4], our results showed that the bone-tocapsule distance and the cartilage thickness of the wrist and MCP joint were slightly less and the diameter of the biceps tendon was somewhat thicker (Table 7). Similar trends were evident in terms of the cartilage thicknesses of the right humeral head and the right medial and lateral condyles. The relatively low body mass index of Koreans compared to Westerners may explain these differences. The thickness of cartilage in femoral condyles has been used both for early diagnosis of knee OA and for the assessment of therapeutic efficacy [16,17]. MSUS permits easy measurement of femoral cartilage thickness in normal individuals but not at the sites of cartilage lesions in OA patients, where the cartilage–soft tissue interface becomes less clear. Cartilage thickness can be measured in both the longitudinal sagittal and the suprapatellar transverse planes in healthy subjects. In addition, longitudinal MSUS scans can be used to evaluate the weight-bearing area at the posterior side of the medial condyle; this is an important region in the context of cartilage damage in OA patients [11]. We also found that a minimal hypoechoic rim around the biceps long-head tendon, and erosions of the dominant (right) humeral head (12.5% of subjects; mean 1.71 mm) were not uncommon in healthy subjects. It is important to set the boundaries of normal MSUS limits to prevent the misinterpretation of data. Tendon and articular abnormalities must be clearly defined [4].
After optimal education as suggested by the EULAR recommendations, good interobserver agreement can be achieved when articular cartilage is evaluated via MSUS [8,9]. Although MSUS depends heavily on examiner skill, both accuracy and reliability increase when examiners follow identical protocols. Meticulous standardization of MSUS knowledge and skills enhances the reliability of large multicenter studies [2]. Our data suggest that weighting may be necessary to enhance among-technician agreement in terms of hand bone-to-capsule distance and tendon pathology. This is the first Korean study to systematically evaluate the need for normal references of MSUS with education. However, other joint structures should be evaluated in healthy subjects. The mean age of enrolled healthy volunteers is slightly young. The cartilage thickness will be decreased with aging. The onset age of RA or OA is much older than the mean age of healthy volunteers in this study. Despite these limitations, we have determined reference values for the joints that are most relevant in clinical practice.
In conclusion, this is the first study to define standard MSUS reference values in healthy Koreans, providing basic data for further clinical investigations. It is important to educate rheumatologists who differ in terms of expertise.
KEY MESSAGE
1. We defined standard reference values for musculoskeletal ultrasonography in healthy Korean adults, providing basic data for further clinical investigations.
2. The reliabilities of both intra- and interobserver agreements were high after appropriate training program.
Notes
The authors would like to thanks Abbvie Korea and Eisai Korea for renting ultrasound machine, but Abbvie Korea and Eisai Korea were not involved in the development or review of the manuscript with the authors.
Acknowledgements
This study was supported by the fund of Soonchunhyang University.