 |
 |
| Korean J Intern Med > Volume 18(1); 2003 > Article |
|
Abstract
Background
We evaluated the efficacy of the cardiopulmonary exercise test as an objective indicator of functional status and as a pre-operative prognostic indicator in patients with mitral regurgitation (MR) and aortic regurgitation (AR).
Methods
Cardiopulmonary exercise tests and echocardiography were performed in 47 patients (MR: 30, AR: 15, MR + AR: 2) before surgery and repeated one year after surgery. We compared the New York Heart Association (NYHA) functional class, peak oxygen consumption rate (VO2peak), exercise duration, left ventricular dimension and ejection fraction, before and after surgery.
Results
Initial VO2peak and exercise duration were significantly different according to NYHA class. A year later, NYHA functional class improved from 2.1±0.1 to 1.4±0.1 (p<0.001). The VO2peak was significantly increased (21.7±1.0 to 23.7±1.0 mL/kg per min, p=0.008) and exercise duration also increased (521.7±35.9 to 623.3±35.7 seconds, p<0.001). When patients were analysed according to their post-operative NYHA functional class, those with class I showed significantly different pre-operative VO2peak (class I: 23.7±1.1, II: 18.3±1.5 mL/kg per min, p=0.005) and exercise durations (class I: 587.5±43.2, II: 415.6±55.7 seconds, p=0.02). Patients with higher pre-operative VO2peak (19.0 mL/kg per min) more frequently became NYHA functional class I than those with a lower pre-operative VO2peak (76.7% vs. 35.3%, p=0.02). But baseline left ventricular dimension and ejection fraction by echocardiography were not different between post-operative class I and II group.
Conclusion
VO2peak and exercise duration are excellent parameters to evaluate the subjective functional class and to predict the post-operative functional class of patients with MR and/or AR. Patients with a pre-operative VO2peak of 19.0 mL/kg per min or more will have a better functional status one year after surgery.
It is often difficult to make decisions on surgery for patients with mitral regurgitation (MR) and aortic regurgitation (AR) because there are no accurate parameters to determine functional status1,2). The functional status is an important prognostic factor because patients with poor pre-operative functional status often show poor post-operative prognosis. In patients with MR and/or AR, pre-operative echocardiographic findings, such as left ventricular dimension (LVD) and ejection fraction (EF), cannot exactly reflect their functional status or symptoms3–6). Even though the cardio pulmonary exercise test is a standard tool to evaluate the patient’s functional status, there are limited reports on the effects of surgical correction of MR and AR on later exercise capacity7–10). We, therefore, evaluated the efficacy of a cardiopulmonary exercise test as an objective parameter of functional status and as a pre-operative prognostic indicator for patients with MR and AR.
Forty-seven patients with severe valvular regurgitation (MR: 30, AR: 15, MR + AR: 2) who received surgery for valvular replacement or valvuloplasty were studied. We excluded any patients who had a component of valvular stenosis, significant respiratory or ischemic heart disease or severe claudication of a lower extremity.
The cardiopulmonary exercise test and echocardiography were performed before and one year after surgery. We compared the patients’ New York Heart Association (NYHA) functional class, peak oxygen consumption rate (VO2peak), exercise duration, LVD and EF, before and after the operations.
An ergometer bicycle (SensorMedics 433DX-D, USA) was used for the exercise test. The use of cardiac drugs (diuretics, digoxin, angiotensin converting enzyme inhibitor, beta-blocker) was permitted. Patients were asked to cycle at a constant rate of 60 r.p.m. We recorded blood pressure and 12-lead electrocardiography every two minutes. The exercise test was stopped if the patients could not continue because of dyspnea or fatigue. Expired gases were analysed on a breath-by-breath basis, using a permanent zirconium oxide electrochemical cell. The gas analyser system was calibrated using a standard gas mixture before each test. After the tests, we recorded exercise durations and calculated VO2peak and ventilatory anaerobic thresholds (AT).
Results are expressed as means standard error of mean. To compare NYHA classes, we used the nonparametric Mann-Whitney U-test. Comparisons between pre-operative and post-operative status on exercise tests were performed using Chi-squared or paired or unpaired Student’s t-tests, according to the case. To determine the cut-off value of preoperative VO2peak for post-operative functional class, we used Chi-squared method corrected with Lausen and Schumacher’s method11).
The study included 47 patients: 30 with MR; 15 with AR and two with MR+AR. In echocardiographic evaluation, 30 patients showed degenerative valvular changes, and 14 patients were rheumatic valvular disease. There were 2 patients with ischemic valvular disease and 1 patient with bacterial endocarditis. Ten patients were in NYHA functional class I, 21 in class II and 16 in class III before surgery. Table 1 shows the baseline clinical characteristics of groups according to their NYHA functional class.
Table 2 shows the results of cardiopulmonary exercise tests and echocardiography before surgery. The VO2peak and exercise durations showed significant differences according to NYHA functional class (p<0.001). However, echocardiographic parameters were not different according to the patients’ pre-operative functional status, as LVD and EF were not different among NYHA functional groups. The NYHA functional class of 12 patients were mismatched with groups categorized by pre-operative 95% confidence interval of VO2peak (VO2peak of Class I: 24.5, II: 20.5 and <24.5, III: <20.5 mL/kg per min).
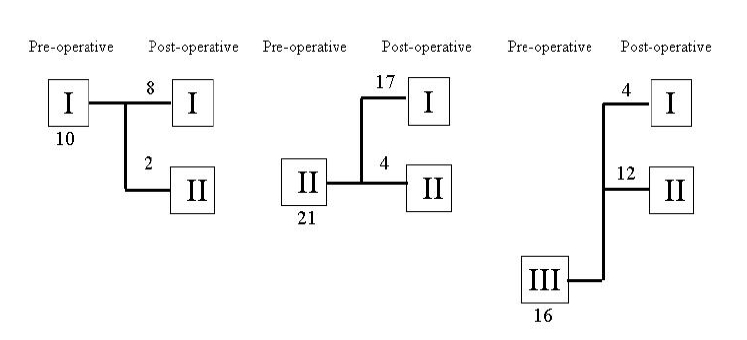
In 47 patients who completed a one-year follow-up after surgery, there was no major adverse clinical events such as death, heart failure, major bleeding due to anticoagulation and embolism. Post-operatively, there was a significant improvement in their NYHA functional class (p<0.001), that is, 29 patients were placed in NYHA functional class I and 18 patients were in class II (Figure 1). The VO2peak increased significantly (p=0.008) and exercise durations also increased (p<0.001). Although systolic and diastolic LVD decreased significantly after surgery (p<0.001), there was no significant change in EF (Table 3).
Of 16 patients categorized as pre-operative NYHA functional class III, all improved to class I (n=4) or II(n=12), post-operatively. When the pre-operative factors determining post-operative NYHA functional class were compared, the pre-operative VO2peak (class I: 23.5±2.8 vs. II: 15.3±1.4 mL/kg per min, p=0.01) and exercise duration (I: 621.5±72.9, vs. II: 304.2±39.0 seconds, p<0.01) were significantly different between post-operative class I and II.
Because pre-operative functional status is an important parameter that determines post-operative prognosis, we divided the patients into two groups according to their initial VO2epeak. The 30 patients with higher pre-operative VO2peak (≥19.0 mL/kg per min) were more frequently categorized as post-operative NYHA functional class I than those with lower pre-operative VO2 peak (76.7% vs. 35.3%, p=0.02) (Figure 2). In 16 patients with NYHA functional class III, there were 6 patients who had higher VO2peak (≥19.0 mL/kg per min), and 4 of these patients were post-operative NYHA functional class I. Table 4 shows the difference in each parameter of cardiopulmonary test and echocardiography according to the value of pre-operative VO2peak.
It is generally accepted that the cardiopulmonary exercise test can predict the patient’s functional status12). However, there has been only limited study about the effects of cardiac surgery on exercise capacity7–10). Our study shows that cardiopulmonary exercise test parameters, especially VO2peak and exercise durations, are highly correlated with the patient’s NYHA class. VO2peak and exercise durations improved in most patients in one year of valve surgery for significant MR and AR. Patients who had high VO2peak values before their operation were categorized as a better post-operative NYHA class, even in those with NYHA class III. This means that the initial NYHA class is not enough to predict post-operative results in some patients. Because NYHA class is a subjective parameter, objective cardiopulmonary testing has an advantage for estimating the patient’s status more accurately. Our results therefore suggest that the cardiopulmonary exercise test is an excellent modality to determine the point of operation, and that a pre-operative cut-off value of the VO2peak of ≥19.0 mL/kg per min may be used to predict the better post-operative status in patients.
In one study carried out seven months after mitral valve surgery for severe chronic MR, although the patients’ NYHA functional class improved, exercise performance parameters, such as VO2peak and exercise duration, did not improve13). To explain this difference from our study, some points should be considered. The cardiopulmonary exercise test can be affected by many factors other than cardiac function, such as pulmonary and peripheral factors, skeletal muscle changes and alterations in blood flow distribution14–17). Improvement in these factors needs an adequate time of recovery to show significant changes in VO2peak and exercise duration. Thus, seven months may be too short to reveal any change in a patient’s exercise capacity. Because the patients in our study repeated their cardiopulmonary exercise tests one year after their operation, there may have been enough time to demonstrate improvements.
Although echocardiographic ejection fraction, end-systolic diameter and dP/dt are important parameters used to make a decision to perform cardiac surgery in patients with MR or AR3–6,18), such findings taken in the resting state do not always correlate with the patient’s functional status. To reveal the exact functional status of patients, it is important to consider both the resting state of the patients and their exercise status18–21). The cardiopulmonary exercise test demonstrates integrated cardiopulmonary functional potential, so it has advantages to reflect the real functional status of patients22–24).
In cases of left ventricular volume overload due to valvular regurgitation, patients with left ventricular systolic dysfunction have poorer prognosis after valvular operations1,2,25), so it is reasonable to perform such operations before the dysfunction develops26,27). However it is very difficult to predict the timing of left ventricular systolic dysfunction and the timing of the operation. In such a situation, it is thought that the cardiopulmonary exercise testing can be used to predict the timing of the operation. We found that patients who had lower pre-operative VO2peak had poorer functional status than those with higher pre-operative VO2peak when evaluated one year after surgery.
However, our study population was too small to calculate the exact cut-off value of VO2peak, so a large prospective study would be needed to define the correct relationship between pre-operative VO2peak and post-operative functional status. Another limitation is that we included both MR and AR in terms of left ventricular volume overload in spite of some differences in the hemodynamics of these two diseases26). In a further study, it is required to evaluate the effects of cardiopulmonary test in MR or AR alone. And the difference between operative methods of MR patients, such as mitral valve repair and mitral valve replacement, is an important parameter to affect the prognosis of post-operative prognosis, so it also should be considered in the next study.
Functional capacities, such as VO2peak and exercise duration, are excellent parameters to evaluate the subjective functional class and estimate the post-operative functional class of the patients with MR and/or AR. We found that patients who had pre-operative VO2peak of 19.0 mL/kg per min or greater showed better functional status one year after surgery. So, a large prospective trial will be necessary to determine an accurate cut-off value of the VO2peak for adequate timing of surgery.
Figure 2.
Comparison of the patients’ NYHA functional classes after operation according to their pre-operative VO2peak level. The patients with higher pre-operative VO2peak (≥19.0 mL/kg/min) were more frequently categorized as post-operative NYHA functional class I than those with lower pre-operative VO2peak (p=0.02).
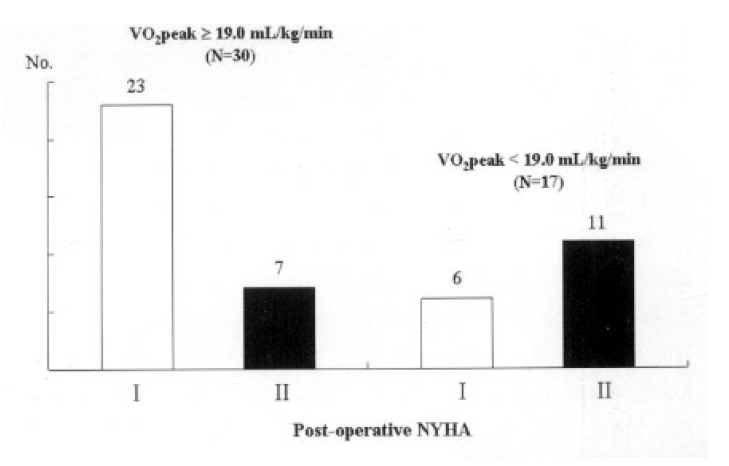
Table 1.
Baseline clinical characteristics
Table 2.
Findings of cardiopulmonary exercise test and echocardiography according to patients’ NYHA functional class
Table 3.
Effects of surgery functional capacity and echocardiographic parameters in patients undergoing mitral and/or aortic valve surgery
Table 4.
Comparison of parameters of cardiopulmonary test and echocardiography between 2 groups divided by pre-operative VO2peak
REFERENCES
1. Quinones MA. Management of mitral regurgitation. Optimal timing for surgery. Cardiol Clin 16:421–4351998.


2. Bonow RO. Chronic aortic regurgitation. Role of medical therapy and optimal timing for surgery. Cardiol Clin 16:449–4611998.


3. Enriquez-Sarano M, Tajik AJ, Schaff HV, Orszulak TA, Bailey KR, Frye RL. Echocardiographic prediction of survival after surgical correction of organic mitral regurgitation. Circulation 90:830–8371994.


4. Enriquez-Sarano M, Schaff HV, Orszulak TA, Bailey KR, Tajik AJ, Frye RL. Congestive heart failure after surgical correction of mitral regurgitation. A long-term study. Circulation 92:2496–25031995.


5. Bonow RO. Radionuclide angiography in the management of asymptomatic aortic regurgitation. Circulation 84(3 Suppl):1296–13021991.


6. Bonow RO, Dodd JT, Maron BJ, O’Gara PT, White GG, Mclntosh CL, Clark RE, Epstein SE. Long-term serial changes in left ventricular function and reversal of ventricular dilatation after valve replacement for chronic aortic regurgitation. Circulation 78:1108–11201988.


7. Nakamura M, Chiba M, Ueshima K, Arakawa N, Yoshida H, Makita S, Kawazoe K, Hiramori K. Effects of mitral and/or aortic valve replacement or repair on endothelium-dependent peripheral vasorelaxation and its relation to improvement in exercise capacity. Am J Cardiol 77:98–1021996.


8. Gohlke-Barwolf C, Gohlke H, Samek L, Peters K, Betz P, Eschenbruch E, Roskamm H. Exercise tolerance and working capacity after valve replacement. J Heart Valve Dis 1:189–1951992.

9. ul Haque ME, Sasaki S, Kuroda H, Ishiguro S, Ogino K, Kobayashi T, Mori T, Mashiba H. Hemodynamic changes during dynamic exercise in patients after mitral valve replacement for chronic mitral regurgitation. Indian Heart J 44:379–3851992.

10. Carstens V, Behrenbeck DW, Hilger HH. Exercise capacity before and after cardiac valve surgery. Cardiology 70:41–491983.


11. Lausen B, Schumacher M. Evaluating the effect of optimized cutoff values in the assessement of prognostic factors. Computational Statistics and Data Analysis 21:307–3261996.

12. Williams SG, Cooke GA, Wright DJ, Parsons WJ, Riley RL, Marshall P, Tan LB. Peak exercise cardiac power output; a direct indicator of cardiac function strongly predictive of prognosis in chronic heart failure. Eur Heart J 22:1496–15032001.


13. Le Tourneau T, de Groote P, Millaire A. Effect of mitral valve surgery on exercise capacity, ventricular ejection fraction and neurohormonal activation in patients with severe mitral regurgitation. J Am Coll Cardiol 36:2263–22692000.


14. Mancini DM, Henson D, LaManca J, Levine S. Respiratory muscle function and dyspnea in patients with chronic congestive heart failure. Circulation 86:909–9181992.


15. Wilson JR, Martin JL, Schwartz D, Ferraro N. Exercise intolerance in patients with chronic heart failure: role of impaired nutritive flow to skeletal muscle. Circulation 69:1079–10871984.


17. Hsia CC. Coordinated adaptation of oxygen transport in cardiopulmonary disease. Circulation 104:963–9692001.


18. Leung DY, Griffin BP, Stewart WJ, Cosgrove DM 3rd, Thomas JD, Marwick TH. Left ventricular function after valve repair for chronic mitral regurgitation: predictive value of preoperative assessment of contractile reserve by exercise echocardiography. J Am Coll Cardiol 28:1198–12051996.


19. Leung DY, Griffin BP, Snader CE, Luthern L, Thomas JD, Marwick TH. Determinants of functional capacity in chronic mitral regurgitation unassociated with coronary artery disease or left ventricular dysfunction. Am J Cardiol 79:914–9201997.


20. Lavie CJ, Lam JB, Gibbons RJ. Effects of exercise on left ventricular volume and output changes in severe mitral regurgitation. A radionuclide angiographic study. Chest 96:1086–10911989.


21. Tischler MD, Battle RW, Ashikaga T, Niggel J, Rowen M, LeWinter MM. Effects of exercise on left ventricular performance determined by echocardiography in chronic, severe mitral regurgitation secondary to mitral valve prolapse. Am J Cardiol 77:397–4021996.


23. Morris CK, Ueshima K, Kawaguchi T, Hideg A, Froelicher VF. The prognostic value of exercise capacity: a review of the literature. Am Heart J 122:1423–14311991.


24. Vanhees L, Fagard R, Thijs L, Staessen J, Amery A. Prognostic significance of peak exercise capacity in patients with coronary artery disease. J Am Coll Cardiol 23:358–3631994.


25. Starling MR, Kirsh MM, Montgomery DG, Gross MD. Impaired left ventricular contractile function in patients with long-term mitral regurgitation and normal ejection traction. J Am Coll Cardiol 22:239–2501993.


26. Bonow RO, Carabello B, de Leon AC Jr, Edmunds LH Jr, Fedderly BJ, Freed MD, Gaasch WH, McKay CR, Nishimura RA, O’Gara PT, O’Rourke RA, Rahimtoola SH, Ritchie JL, Cheitlin MD, Eagle KA, Gardner TJ, Garson A Jr, Gibbons RJ, Russell RO, Ryan TJ, Smith SC Jr. Guidelines for the management of patients with valvular heart disease: executive summary A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee on Management of Patients with Valvular Heart Disease). Circulation 98:1949–19841998.





 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print



