 |
 |
| Korean J Intern Med > Volume 16(4); 2001 > Article |
|
Abstract
Angiomyolipoma is a common tumor of the kidney but has rarely been found in the mediastinum. We report a case of angiomyolipoma of the posterior mediastinum in a 62-year-old woman. She experienced exertional dyspnea and intermittent cough at admission. Computed tomography indicated a tumor located at the left paravertebral and upper posterior mediastinum and MRI imaging demonstrated a mass with low signal intensity in T1-weighted image at T4-5 level. Thoracotomy was done for surgical removal of the tumor and histologic examination revealed a mesenchymal tumor composed of mature fat, capillaries and smooth muscle fibers. The tumor was immunohistochemically positive for CD34 and factor-VIII (for vascular component) smooth muscle actin (for smooth muscle component) and S-100 protein (for fat component). There have been four case reports about mediastinal angiomyolipoma, namely three Japanese cases and one French case. It is suggested that angiomyolipoma could be considered for the differential diagnosis of mediastinal tumors.
Angiomyolipoma, a form of mixed mesenchymal tumor, is a benign neoplasm composed of proliferated blood vessels, smooth muscle and fatty tissue with intermediate and immature cells. It is a fairly common tumor of the kidney but rarely found in the mediastinum. It can also occur in a sporadic form or be associated with tuberous sclerosis1). According to the literature, there have been only four case reports about mediastinal angiomyolipoma, namely three Japanese papers and one French paper2ŌĆō5). We report a case of mediastinal angiomyolipoma successfully removed by thoracotomy.
A 62-year-old woman was admitted to the hospital with a 20-day history of exertional dyspnea. The patient had been well until 20 days earlier, when she experienced exertional dyspnea and intermittent cough. There was no history of diabetes, hypertension, tuberous sclerosis and pulmonary lymphangioleiomatosis. At admission, the patient was ill-looking. On physical examination, her breathing sound was clear but decreased on the left side. Neurologic exmination revealed no abnormal finding. The results of routine hematologic, blood chemical and enzyme tests and the electrocardiographic findings were normal. Radiographs of the chest showed a 4├Ś4 cm-sized, well-defined mass in the left upper paravertebral area along with left pleural effusion. Therapeutic and diagnostic thoracentesis was performed. The effusion was clear in color and lymphocyte-dominant exudate. The cytologic examination was negative for malignant cells and the car cinoembrionic antigen (CEA) level was within normal range. The computed tomographic (CT) scan of the thorax, obtained after the injection of contrast material, showed a 4├Ś3├Ś3cm-sized, well-defined high density posterior mediastinal mass with a suspicious finding of rib destruction (Figure 1). MRI imaging of the thoracic spine revealed a round mass in the posterior mediastinum at T4-5 level with low-signal intensity in T1-weighted image which was well enhanced and with suspicious epidural space-nvasion (Figure 2). Percutaneous transthoracic needle biopsy was performed under fluoroscopic guide. The pathologic findings were highly suggestive for angiomyolipoma. The kidney ultrasonography revealed no abnormal findings. Thoracostomy was done for surgical removal and confirmative diagnosis. Pre-operative bronchoscope finding was normal. Left posterolateral thoracotomy was done via the 4th intercostal space. A 2├Ś3cm-sized globular mass was found which had its base between the 3rd and 4th costovertebral junction with its wide stalk. The 4th intercostal nerve and sympathetic nerve were involved by the tumor, but there was no evidence of epidural or pleural involvement. En bloc excision, including the tumor, the fourth intercostal nerve, sympathetic nerve and bones of the 3rd and 4th costovertebral junction area, was performed.
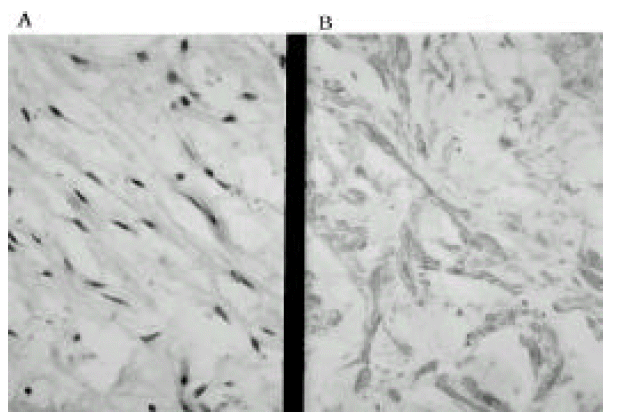
Histologically, the tissue was characterized by mesenchymal cell proliferation, intricately composed of mature fat, capillaries and smooth muscle fibers (Figure 3). In immunohistochemical staining to identify the different components of angiomyolipoma, smooth muscle actin was positive for smooth muscle component (Figure 4A, 4B), CD34 (Figure 5) and factor-VIII for vascular component were positive and S-100 was positive for fat component. Tissue from rib excision was negative for tumor and there was no evidence of malignancy. The histopathologic diagnosis of angiomyoiipoma was made. During the operation, there was no remaining pleural effusion and no gross pathology on the pleural surface. There has been no evidence of recurrence of the tumor or pleural effusion during the three months of follow-up.
Mediastinal tumors of mesenchymal origin are rare and, especially, angiomyolipoma of the mediastinum is an extremely rare tumor with only several cases having been described in the literature. In general, angiomyolipoma is a distinctive mesenchymal neoplasm of the kidney. It classically presents with a renal tumor showing a variable combination of mature adipose tissue, abnormal blood vessel and smooth muscle fascicles. Renal angiomyolipoma is a benign tumor that may occur as an isolated phenomenon or as a part of the syndrome associated with tuberous sclerosis. Angiomyolipomas infrequently present in other sites, the more common being perirenal lymph nodes, retroperitoneum, liver and uterus6ŌĆō8). The tumor is named after the microscopic three primary components: blood vessels, clusters of adipocytes and sheets of smooth muscle. Pleomorphism is common and mitotic figures, although rarely seen, can be prominent9). Although there are reports of malignant angiomyolipoma, it is currently believed that extrarenal and lymph node involvement reflects multicentricity rather than metastasis and is not a sufficient criteria for malignancy10ŌĆō11). On CT, the tumor had low density and on sonography, the tumor was highly echogenic due to its fat component. Angiography reveals that the tumor is usually highly vascular. Angiomyolipoma on MRI is characterized by the high signal intensity on nonenhanced T1-weighted images and also high signal in T2-weighted images. Its vascular component appeared well-enhancing. Management of angiomyolipoma is controversial. Small asymptomatic tumor may be conserved with follow-up. When the tumor is large-sized and has a high risk of spontaneous rupture, surgical excision or selective arterial embolization can be a valuable treatment. According to the previously reported cases, transarterial embolization was performed in one case and the other two cases were treated by surgical excision. In this case, the patient was a 62-year-old female, in whom a round mass and pleural effusion were detected on simple plain chest X ray. The CT and MRI finding showed a well-defined posterior mediastinal mass with rib destruction and suspicious epidural space invasion. So, our impression of this tumor was malignant neurogenic tumor which is most commonly found in mediastinum, especially posterior mediastinum, with 25% incidence. However it is suggested that this tumor was angiomyolipoma in fluoroscopy-guided fine-needle biopsy. It was composed of fatty tissue, smooth muscle and vascular tissue. Immunohistochemical staining was done for confirmation of each component and revealed positive stainings for CD34 and factor-VIII (for vascular component), SMA (for smooth muscle component) and S-100 protein (for fat cells). Resection of the tumor with 3rd and 4th rib costovertebral junction was performed by left thoracotomy. The operative finding revealed no evidence of epidural or pleural invasion. Pathology of bone and iung tissue was negative for malignant cells. Resected perihilar lymph node consisted of mature adipose tissue with mesothelial lining. The pleural effusion in this case was exudate and negative for malignant cells. Left lung tissue showed no evidence of lymphangioleiomatosis. Pleural thickening with fibrosis and hemorrhage was found. So, we considered that pleural effusion might be the reactive change to unknown stimulus in this case.
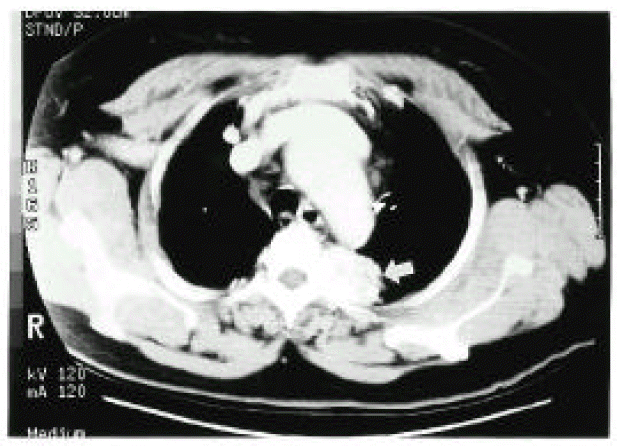
Figure┬Ā1.
The CT scan of the thorax at aortic arch level showed a 4├Ś3├Ś3 cm-sized, well-defined mass in the posterior mediastinum. The mass showed high density with good contrast enhancement (arrow).
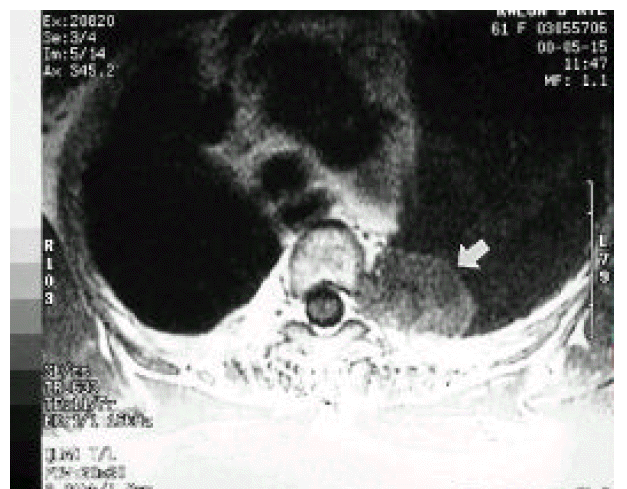
Figure┬Ā2.
MRI imaging of the thoracic spine revealed an ovoid mass in the posterior mediastinum at T4-5 level with low signal intensity in T1-weighted image which is well enhanced after injection of contrast media. Epidural space invasion by the tumor was suspected (arrow).
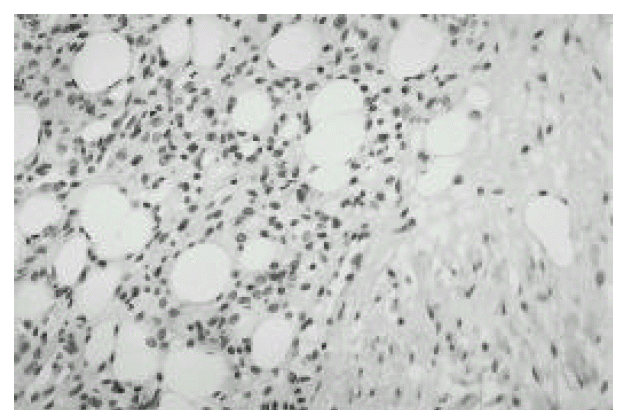
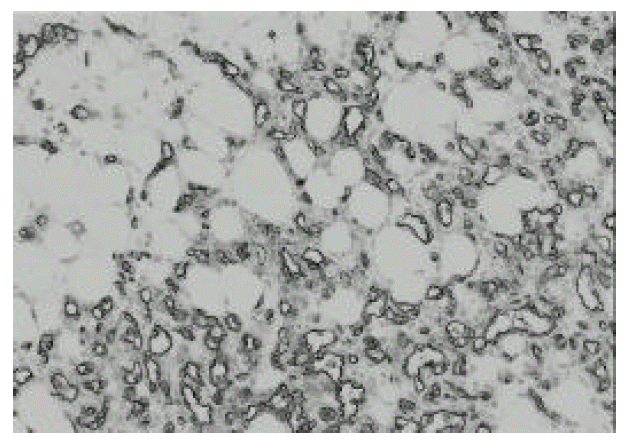
Figure┬Ā3.
Histologic section of the tumor revealed exuberant mesenchymal proliferation which was intricately composed of mature adipocytes, opened or closed capillaries and smooth muscle fibers (H & E, ├Ś100).
REFERENCES
1. Eble J. Angiomyolipoma of kidney. Smin Diagn Pathol 15:21ŌĆō401998.
2. Fukuzawa J, Shimizu T, Sakai E, Ido A, Fujita Y, Tsuji T, Ohki Y, Kimura T, Fujita M, Onodera S. Case report of angiomyolipoma of the posterior mediastinum. Nihon Kyobu Shikkan Gakkai Zasshi 30:464ŌĆō4671992.

3. Hayashi K, Yamamoto M, Nishimura H, Inou N. Angiomyolipoma of the anterior mediastinum; a case report. Nippon Kyobu Geka Gakkai Zasshi 42:584ŌĆō5871994.

4. Watanabe S, Sato H, Tawaraya K, Tsubota M, Endo M, Seki M. A case of mediastinal angiomyolipoma. Nippon Kyobu Geka Gakkai Zasshi 45:1889ŌĆō18921997.

5. Bertrand G, Bidabe M, George P, Dubin P, Touzard C. Angiomyolipoma of the central mediastinum. An apparently undescribed entity. Ann Chir 38:679ŌĆō6811984.

6. Ditonno P, Smith R, Koyle M, Hannah J, Belldegrun A. Extrarenal angiomyolipomas of the perinephric space. J Urol 147:447ŌĆō5501992.


7. Terris B, Flejou JF, Picot R, Belghiti J, Henin D. Hepatic angiomyoiipoma: a report of four cases with immunohistochemical and DNA-flow cytometric studies. Arch Pathol Lab Med 120:68ŌĆō721996.

8. Tsui W, Colombari R, Portmann B, Bonetti F, Thung S, Ferrell L, Nakanuma Y, Snover D, Bioulac-Sage P, Dhillon A. Hepatic angiomyolipoma: a clinicopathological study of 30 cases and delineation of unusual morphologic variants. Am J Surg Pathol 23:34ŌĆō481999.


9. Colvin R, Dickersin G. Pathology of renal tumors. In: Skinner DG, deKernion JB, eds. Genitourinary cancer. Philadelphia: W.B. Saunders, 1978;84.



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print



