Abdominal paracentesis is a treatment or diagnostic option for patients with liver disease. Usually the procedure is minimally invasive, because a small gauge needle is used. Patients with acute or chronic liver disease tend to have severe coagulopathy, and for this reason, hemorrhage after abdominal paracentesis is a critical complication in these patients. The inferior epigastric artery is the most common bleeding vessel followed by the mesenteric varix. However, bleeding from other vessels is rare, and multiple vascular bleedings are extremely rare. We present a case of multiple vascular bleeding complications after abdominal paracentesis in which transarterial embolization was required.
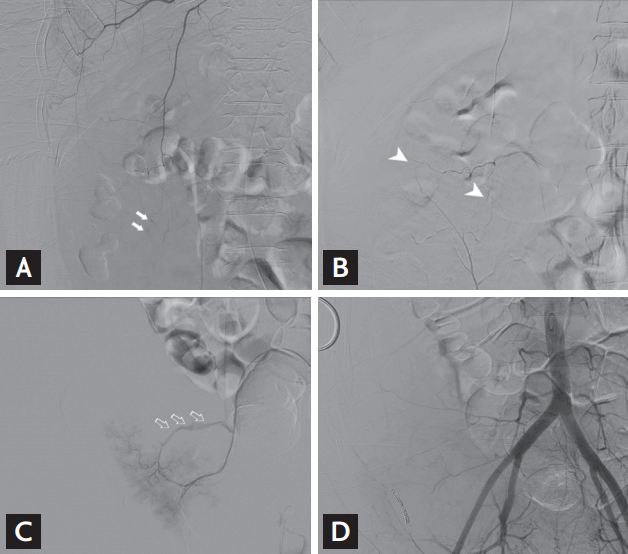
After paracentesis, abdominal wall hematoma occurred in a 49-year-old patient with cirrhosis and ascites. On a computed tomography (CT) scan, a huge hyperdense mass with multiple pseudoaneurysms (arrows), compatible with hematoma, was observed in the right abdominal wall (Fig. 1A and 1B). Right external iliac angiography visualized pseudoaneurysms at the right inferior gastric and lateral circumflex iliac arteries (Fig. 1D), which was confirmed by maximal intensity projection CT images (Fig. 1C). Laboratory findings showed anemia induced by massive bleeding, hemoglobin level (7.4 g/dL) with prothrombin time prolongation. The patient was treated by percutaneous transarterial embolization. Internal mammary artery angiography showed multiple punctate ongoing hemorrhagic foci at the superior epigastric artery (Fig. 2A), which is the terminal branch of the internal mammary artery. The superior epigastric artery was anastomosed with the inferior epigastric artery, which is extremely rare in case of vascular bleeding (Fig. 2B). Branches of the superior gluteal artery showed ongoing large amounts of hemorrhage (Fig. 2C). These vessels were all treated with micro coils and particles, and final angiography showed no ongoing hemorrhagic focus and well embolized arteries (Fig. 2D).
Abdominal paracentesis is a common procedure in patients with liver disease, and thus, the possibility of complications is easily overlooked. To reduce the risk of complications, it is important bleeding tendency be checked before the procedure and that vessels passing through the abdominal wall be avoided by using ultrasound.
Written informed consents were obtained.




 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print





