 |
 |
| Korean J Intern Med > Volume 10(2); 1995 > Article |
|
Abstract
Objectives:
Interferon is the only established teatment for chronic hepatitis C but the host-dependent or virus-related factors affecting the response rate to interferon therapy are not yet dear. The purpose of this study was to investigate the factors predictive of response to interferon-alfa therapy in chronic hepatitis C.
Methods:
Twenty-five consecutive patients with chronic hepatitis C were randomized to three regimens of interferon-alfa: group A (n=7, 3MU every day for 3 months), group B (n=8, 3MU every other day for 3 months) and group C (n=10, 3MU every other day for 6 months), We quantified serum HC RNA levels by competitive reverse transcription-polymerase chain reaction (RT-PCR)and performed HCV genotyping using type-specific primers deduced from the NS5 region of the HCV genome. We also attempted to identify which demographic, biochemical and histologic factors in addition to virus-related factors would significantly predict beneficial response to interferon by multivariate analysis.
Results:
Sustained responders were 8 (36.4%), nonsustained responders were 2 (9.1%) and nonresponders were 12 (54.5%) of 22 patients who had received complete therapy. The initial HCV RNA level (logarithmic transformed copy numbers per ml of serum)in sustained responders (5.75┬▒0.39) was significantly lower than that of nonsustained responders (6.80┬▒0.71)and nonresponders (6.70┬▒0.52) (p<0.05).
In multivariate multiple logistic regression analysis, the serum HCV RNA level before therapy was only the independent predictor of a sustained response to interferon-alfa therapy (p=0.001).
The hepatitis C virus (HCV) has known to be the major causative agent of post-transfusion hepatitis, since the cloning of the HCV genome was performed1,2). It is reported that about 50% of patients with HCV infection develop chronic hepatitis, and 10ŌĆō25% of these cases will eventually progress to liver cirrhosis of hepatocellular carcinoma3).
Interferon (IFN) is considered the only approved therapy for chronic hepatitis C to date4ŌĆō6), but the large number of relapses after cessation of therapy remains a problem.
Recently, many factors influencing the response to IFN therapy have been reported7ŌĆō12). Among these, the HCV genotype and serum HCV RNA level of viral chracteristics have been recognized more specific than any other predictive factor10ŌĆō12).
The purpose of this study was to evaluate clinical, biochemical and virological factors that would predict response to IFN-alfa therapy by univariate or multivariate analysis.
Twenty five consecutive patients (16 men and 9 women) with chronic hepatitis C, with a mean age of 47 years (range: 23ŌĆō58 years), were included in the study. All had persistently elevated serum alanine aminotransferase (ALT) levels of at least twice the upper normal limit of the normal range for at least 6 months, histological evidence of chronic hepatitis (chronic active hepatitis in 23 patients, chronic persistent hepatitis in 2 patients) and seropositivity for both anti-HCV [second generation enzyme immuno assay (EIA), Abbott Laboratories, North Chicago, IL, USA] and HCV RNA [reverse transcription-polymerase chain reaction (RT-PCR)]. Criteria for exclusion included evidence of infection with hepatitis A or B virus, decompensated liver disease, pregnancy or lactation, the presence of any serious medical or psychiatric illness and evidence of other forms of liver disease. Informed consent for participation was obtained from all patients before treatment.
Clinical and laboratory evaluation were performed monthly before and during treatment and then monthly between 6 and 36 months after treatment was completed.
Patients were randomly assigned to receive recombinant IFN alfa-2a (Intermax alpha; Lucky Biotec. Taejeon, Korea)according to three different protocols: group A (n=7), 3 million units (MU), subcutaneously (s. c.), every day for 3 months; group B (n=8), 3MU, s. c., every other day for 3 months; group C (n=10), 3 MU, s. c., every other day for 6 months.
Serum anti-HCV was tested by a second generation commercial EIA kit and assayed before and at the end of treatment.
Oligonucleotide primers for detection, genotyping and quantitation of HCV RNA were synthesized by a DNA synthesizer (Pharmacia, LKB, Uppsala, Sweden).
HCV RNA was extracted from 100 ╬╝l of serum, as described previously13), and extracted RNA was precipitated with isopropanol and washed with ethanol. The HCV RNA pellet was dissolved in diethylpyrocarbonate-treated distilled water (DEPC-H20) and stored until use. Synthesis of cDNA from HCV RNA samples was carried out at 37┬░C for 1hour with 20 units of Moloney Murine Leukemia Virus reverse transcriptase (MMLV-RT, GIBCO BRL, Gaithersburg, MD. USA). The cDNA product was amplified on two stage PCR. The two sets of primer used for RT-PCR were derived from 5ŌĆ▓-untranslated region (5ŌĆ▓-UTR) of HCV genome14). The sequences were 5ŌĆ▓-CTG TGA GGA ACT ACT GTC TT-3ŌĆ▓ (sense, nucleotides 28 to 47) and 5ŌĆ▓-CTG TGA GGA ACT ACT GTC TT-3ŌĆ▓ (antisense, nucleotides 229 to 248) as an outer primer set, and 5ŌĆ▓-TTC ACG CAG AAA GCG TC TAG-3ŌĆ▓ (sense, nucleotides 46 to 65) and 5ŌĆ▓-GTT GAT CCA AGA AAG GAC CC-3ŌĆ▓ (antisense, nucleotides 171 to 190) as an inner primer set.
After extraction of HCV RNA and synthesis of cDNA as described above, the double stage PCR were performed with the four genotype-specific oligonucleotide primers described by Enomoto et al15). Kato et al.16,17) Chayama et al18) that were deduced from the nucleotide sequences in the NS5 region. The sequences of the universal primers for four genotypes used in the first round PCR were 5ŌĆ▓-TGG GGA TCC CGT ATG ATA CCC GCT GCT TTGA-3ŌĆ▓ (sense, corresponding to nucleotides 8230 to 8260 of HCV-J 16)) and 5ŌĆ▓-GGC GGA ATT CCT GGT CAT AGC CTC CGT GAA-3ŌĆ▓ (antisense, corresponding to nucleotides 8601 to 8630 of HCV-J 16)). The sequences of the primers in the second round PCR for HCV-US, -J, -K2a and -K2b, which are HCV genotypes 1a, 1b, 2a and 2b, respectively, according to the nomenclature of a recently proposed system 19), were 5ŌĆ▓-CGA CAT CCGT ACG GAG GAGG-3ŌĆ▓ (sense) and 5ŌĆ▓-CAG GCT GCC CGG GCC TTG AT-3ŌĆ▓ (antisense) for HCV genotype 1a, 5ŌĆ▓-TGA CAT CCG TGT TGA GGA GT-3ŌĆ▓ (sense)and 5ŌĆ▓-CGG GCC GCA CAG GCC TCC AA-3ŌĆ▓ (antisense) for genotype 1b, 5ŌĆ▓-TAT GTT CAA CAG CAA GGG CCA GA-3ŌĆ▓ (sense) and 5ŌĆ▓-CCT GGT CAT AGC CTC CGT GAA-3ŌĆ▓ (antisense) for genotype 2a, and 5ŌĆ▓-CCT GGT CAT AGC CTC CGT GAA-3ŌĆ▓ (sense) and 5ŌĆ▓-CCTGGTCATAGCCTCCGTGAA - 3ŌĆ▓ (antisense) for genotype 2b.
10╬╝l of synthesized cDNA was amplified on two stage PCR as described previously20). The first PCR was carried out for 35 cycles of three steps, 1 min at 94┬░C, 1 min at 40┬░C and 1min at 72┬░C, respectively, and then 1 ╬╝l of the first PCR products was put into the prepared 4 each genotype specific microtube. The second PCR was carried out for 30 cycles of three steps, 1 min at 94┬░C, 45 seconds at 55┬░C, and 1 min at 72┬░C. The amplified DNA fragments were electrophoresed in 2% agarose gels with ethidium bromide staining and were observed under UV light.
HCV RNA was quantified by a competitive RT-PCR assay using synthetic mutant HCV RNA as an internal template21,22). A mutant RNA was synthesized by means of site-directed mutagenesis and in vitro transcription.
A cDNA included 5ŌĆ▓-UTR of HCV genome from the serum of HCV carrier was cloned into an M13mp18 vector system. After the above the M13mp 18-5ŌĆ▓UTR plasmid was digested with restriction endonucleases, BamHI and Hind III (NEB, USA), and cloned again into pGEM4-z vector (pGEM-5ŌĆ▓UTR). A deletion mutant (pGEM-5ŌĆ▓UTRdel) was made by PCR. A mutant containing 80 base pairs deletion (pGEM-5ŌĆ▓UTRdel)was digested Hind III, which served as templates for T7 RNA polymerase, and then the DNA template was removed using DNase I (Promega, RQ1 RNase free DNase I). The above mutant RNA transcripts were purified by phenol-chloroform extraction and ethanol precipitation and used as internal templates in quantitative competitive PCR. HCV RNA extraction using 50╬╝l of serum was performed as described above.
An equal amount of sample RNA was put into a set into a set of microtubes that already had serially 10-fold diluted mutant RNA.
The sequences of primer used in the first PCR were HCV QC1 5ŌĆ▓-CCA CCA TAG ATC ACT CCC CTGT-3ŌĆ▓ (corresponding position 28 to 48 of HCV-II) as a sense primer and HCVL70, 5ŌĆ▓-TTG AGG TTT AGG ATT CGT GCT CAT-3ŌĆ▓ (corresponding position 343 to 366 of HCV-II) as an antisense primer.
The first PCR was carried out for 40 cycles of steps for 1min at 95┬░C, 1min at 55┬░C and 2min at 72┬░C, and then the second PCR was carried out for 25 cycles of steps for 1min at 94┬░C, 45seconds at 55┬░C and 1min at 72┬░C.
Complete response (CR) was defined as a normalization of serum ALT levels at the end of therapy. A sustained response (SR) was defined as the presence of persistently normal serum ALT levels and negative seroconversion of HCV RNA during the entire follow up (for at least six months) after CR. Nonsustained response (NSR) was of serum ALT levels became elevated again during follow up after CR. Patients were defined as nonresponders (NR) if serum ALT levels were persistently abnormal during or after treatment.
The Chi-square test or FisherŌĆÖs exact test was used for comparison between group frequencies. Univariate and multivariate analysis were used to establish which factors contributed to a sustained response to IFN therapy. We used SPSS (version 6.0) program for statistical analysis of all variables.
The patients included in this study were 25 patients (16 men and 9 women, with a mean age of 47, and an age range of 23 to 58), with seropositive anti-HCV, who had elevated serum ALT levels for at least 6months prior to the study. Four patients had a prior history of blood transfusions and the remainder had HCV infection from unknown causes. Three of the 25 patients had side effects (thrombocytopenia, leukopenia, depression) that led to discontinuation of therapy.
Table 1 shows the demographic, laboratory and histological profiles of the 25 patients before treatment.
The 22 patients who completed IFN therapy were divided into three groups according to their response to administration of IFN: SR, 8 of 22 patients (36.4%); NSR, 2 of 22 patients (9.1%) and NR, 12 of 22 patients (54.5%). No significant differences were seen in age, sex, history of transfusion and mean ALT of the three groups. No demographic or laboratory finding significantly affected the sustained response to IFN as determined by univariate or multivariate analysis.
As regards the relationship between the histological findings and the response to IFN-alfa therapy, for the 21 patients with chronic acive hepatitis (CAH), SR totalled 7 patients (33.3%), NSR totaled (9.5%) and NR totalled 12 patients (57.1 %). The sole patient with chronic persistent hepatistis (CPH) was a SR (Table 1).
The responses according to different IFN-╬▒ regimens were not significantly different in each group (Table 2).
The results of HCV grnotyping shown in Table 3 and Fig. 1. 14 of 22 patients (63.6%) were genotype 1b, 7 of 22 patients (31.8%) were HCV 2a type and 1 patient had an undetermined type. In response to IFN-╬▒ according to HCV genotype, 5 (35.7%), 2 (14.3%) and 7 (50.0%) of 14 patients with HCV 1b type showed SR, NSR and NR, respectively. Of 7 patients with HCV 2a type, 3 (42.9%) and 4(57.1%) had SR and NR, respectively. No significant correlation between response to IFN-╬▒ and genotype was seen.
The quantitation by competitive RT-PCR was performed in all patients and the quantity of serum HCV RNA was determined in all patients, except one patient. Serum HCV RNA levels expressed as log10 (copy numbers of HCV RNA per ml serum) varied from 5.3 to 7.3. In the response to IFN-╬▒ according to serum HCV RNA levels before treatment, patients with SR had significantly lower serum HCV RNA levels (5.75┬▒0.39) than those of patients with NSR or NR (6.80┬▒0.71, 6.70┬▒0.52, respectively) (p<0.05) (Fig. 3).
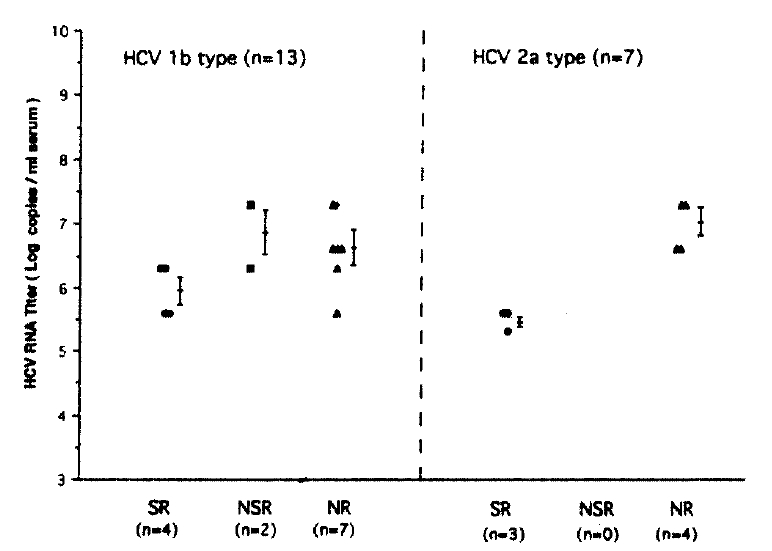
Patients were stratified to genotype 1b and -2a to see which is a more important predicor of response to IFN-╬▒ between serum HCV RNA levels before IFN therapy and genotype. In patients with genotype 1b, serum HCV RNA levels of SR, NSR and NR showed 5.95┬▒0.40, 6.80┬▒0.71 and 6.95┬▒0.40 respectively. In two genotype groups serum, HCV RNA levels of SR were lower than those of patients with NSR or NR. However, there was no statistically significant difference between each group or between genotypes (Fig. 4).
IFN was well tolerated in almost all patients and the side effects were generally not serious and the patients soon recovered. The common side effects were initially transient flu-like syndrome (100%), fatigue (48.0%), hair loss (44.0%), loss of appetite (40.0%), leukopeina (24.0%), thrombocytopenia (20.0%), emotional instability (12.0%) and thromboembolism (4.0%). Three of 25 patients who initially enrolled in the study stopped treatment due to serious side effects of marked thrombocytopenia and leukopenia, derpession and thromboembolism, respectively.
Multiple regression analysis in a stepwise method was performed to identify the variables (demographic, biochemical, histological, HCV genotype and HCV RNA levels) having significant correlation with sustained response to IFN therapy.
Serum HCV RNA level before therapy was only estimated to be independently predictive of a sustained response (p=0.001; 95% confidence intervals, 0.227ŌĆō0.758).
IFN-╬▒ is known as the only established treatment for chronic hepatitis type C. The reason why not all patients respond to IFN therapy is not clear. However, patients characteristics, administration schedule of IFN therapy and molecular biological properties of HCV are thought to be some of the factors influencing the outcome of IFN therapy. Among them, shorter duration of disease, absence of cirrhosis, prolonged therapy with higher doses, a lower histologic activity index (HAI), HCV genotype 2 and lower level of serum HCV RNA have been associated with better response to IFN4,6,11ŌĆō12,23ŌĆō25).
In this study, demographic profiles, biochemical data and histological findings before IFN therapy had no important effect on the response rate to IFN, as reported previously26).
Although the shorter duration of disease is reported to predict a better response to IFN therapy12), we did not include it among possible variables that can influence the response to IFN therapy in this study, because the time of onset of HCV infection or hepatitis could not be fully evaluated by biochemical or virological studies in retrospective analysis.
Although higher initial doses and longer duration of IFN therapy showed higher long-term response rates4,6,12), compared to the standard 24 week, 3 MU TIW treatment schedule, the alternative treatment regimens for beneficial response to IFN have remained unclear. In our study, the sustained response rate according to different regimens of IFN-╬▒ was 42.9% of group A, 40.0% of group B and 30.0% of group C. However, no significant differences were seen in the response rate among these three groups. The response rate at treatment regimens with the same doses but with different durations between group A and C, was higher in group A. Moreover group B, with a regimen of shorter duration, had a better response rate than group C with regimen of longer duration. Thus, further extensive studies will be needed to clarify the relationship between the response rate to IFN and regimens of IFN including, doses and duration.
Sustained loss of serum HCV RNA was observed in the 8 SR but in none of the responders. This showed that HCV might be eradicated in 8 of the 22 patients (36.4%) treated with IFN therapy.
HCV genotype has been known to be associated with the response rate to IFN therapy and generally, genotype III (2a) has a better response to IFN than genotype II (1b)12,24). The reason why the HCV genotype influences the response rate to IFN is still unclear. Some researchers hypothesize it may be associated with the degree of heterogeneity of the hypervariable region (E2/NS1) within the HCV genome27). Our data showed that the sustained response rate was higher in patients with genotype 2a (42.9%) than in those with genotype 1b (35.7%), but this difference is not statistically significant.
We quantified HCV RNA in the sera from patients using a competitive RT-PCR assay with synthetic mutant HCV RNA as an internal template (competitor)21). The advantages of this method, compared to KanekoŌĆÖs method28), are that firstly, conserved 5ŌĆ▓-UTR of HCV genome was used as a template and thus all genotypes of HCV could be detected; secondly, the efficiency of cDNA synthesis by reverse transcriptase could not influence the quantitiation of HCV RNA because synthetic mutant RNA was used as an internal template; and finally, any contamination could be easily found because synthetic mutant RNA was deleted in 80 base pairs of sequences. However, as competitive RT-PCR is a complicated and time consuming method, it is not available for mass clinical samples. Recently, an easier branched DNA signal amplification (bDNA) assay (Chiron, CA, USA) was developed for quantification of HCV RNA. This method will be commonly used in the future.
The initial titer of HCV RNA or HCV genotype by the previous reports25,26) was suggested as the most significant independent predictor of a sustained response to IFN therapy. In this study serum HCV RNA level before treatment was significantly lower in SR than in NSR and NR (P<0.05). These results suggested that interferon-╬▒ is effective for suppressing the replication of HCV. Also, multivariate multiple logistic regression showed that pretreatment HCV RNA level is a most significant independent predictor of a sustained response to IFN.
In the relationship between serum HCV RNA levels before therapy and HCV genotype in three groups, no significant correlation in levels of viremia between each group, or between genotypes, was seen. These results agree with TsubotaŌĆÖs data26).
We conclude that serum HCV RNA level before therapy is the most important factor influencing the long-term response to IFN therapy.
Fig.┬Ā1.
Detection of each HCV genotype by reverse transcription-nested polymerase chain reaction using the genotype specific primers deduced from NS5 region of HCV genome.
The upper portion [A] shows HCV-J (1b) type while the lower portion[B] shows HCV-K2a (2a) type. The letter ŌĆ£LŌĆØ indicates molecular weight size marker (123 bp).

Fig.┬Ā2.
Quantitation of HCV RNA by competitive polymerase chain reaction using the internal template, which was synthesized by site-directed mutagenesis and in vitro transcription, as control.
The upper bands (268 bp) indicate amplified DNA fragments derived from target HCV RNA, and the lower band (188 bp) indicate those from the internal template as competitor. At the equivalent point of signal intensities between the two bands, the amounts of target HCV RNA are the same as the copy numbers of the internal templates. The arrow on the lower portion indicates the point of titration of HCV RNA (4├Ś104 copies/ml serum). The numbers above the oblique arrows on the upper portion are the copies of the internal templates. The letter ŌĆ£LŌĆØ indicates molecular weight size marker (123bp).
CNC: negative control used in cDNA synthesis
PNC: negative control used in PCR process
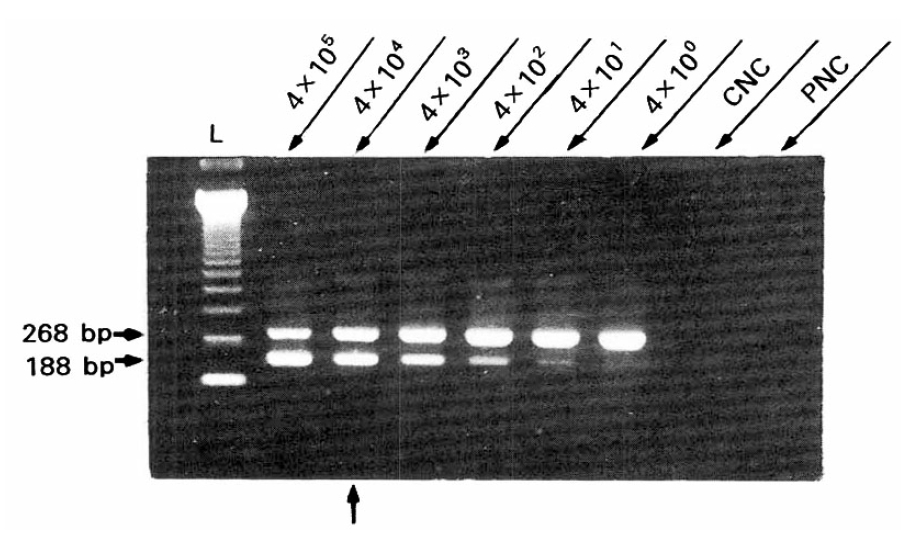
Fig.┬Ā3.
Comparisons of circulation HCV RNA quantity in each response group before IFN therapy. SR (ŌĆó), stustained responder; NSR (Ō¢¬), nonsustained responders; NR (Ō¢┤), nonresponders.
Bars express mean┬▒S.D. Logarithms of serum HCV RNA quantity (mean┬▒S.D) were 5.75┬▒0.39 in SR, 6.80┬▒0.71 in NSR and 6.70┬▒0.52 in NR. Significant differences in serum HCV RNA quantity were seen between SR, and NSR and NR (p<0.05).
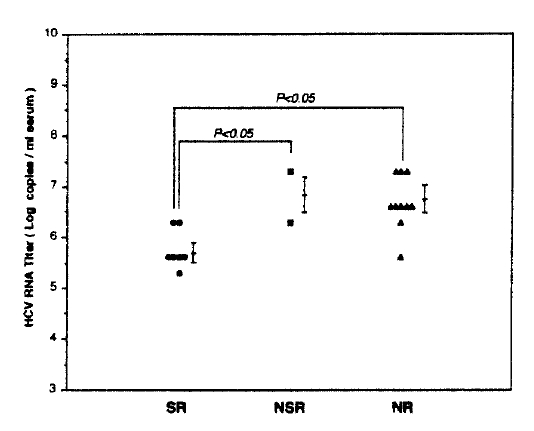
Fig.┬Ā4.
Correlations between serum HCV RNA levels and HCV genotypes in three response groups before IFN therapy. SR (ŌĆó), sustained responder; NSR (Ō¢¬), nonsustained responders; NR (Ō¢┤), nonresponders. No significant correlations in serum HCV RNA levels between each group or between genotypes were seen.
Table┬Ā1.
Demographic, Biochemical and Histological Features of Three Responders bofore IFN-╬▒ Therapy (N=22)*
| Characteristics | Sustained responders | Non-sustained responders | Non-responders |
|---|---|---|---|
| Demography | |||
| ŌĆāŌĆāNo. of Patients | 8 | 2 | 12 |
| ŌĆāŌĆāMean age (yr)a | 46 (27ŌĆō63) | 56 (55ŌĆō57) | 44 (23ŌĆō56) |
| ŌĆāŌĆāSex (M/F) | 4/4 | 2/0 | 9/3 |
| ŌĆāŌĆāHistory of transfusion | 1 | 0 | 2 |
| Laboratory findings before therapyb | |||
| ŌĆāŌĆāALT (IU/L) | 208.9┬▒115.4 | 131.0┬▒4.2 | 143.8┬▒68.8 |
| ŌĆāŌĆāAST (IU/L) | 151.4┬▒103.5 | 72.0┬▒19.8 | 95.8┬▒74.7 |
| ŌĆāŌĆāAlk. Phos. (IU/L) | 257.1┬▒66.0 | 148.5┬▒17.7 | 224.1┬▒77.2 |
| ŌĆāŌĆār-GTP (IU/L) | 58.9┬▒29.8 | 39.0┬▒5.7 | 54.8┬▒26.4 |
| ŌĆāŌĆāPlatelet (109/L) | 192.8┬▒93.3 | 225.0┬▒162.6 | 162.8┬▒68.6 |
| Histologic findings | |||
| ŌĆāŌĆāCHA (n=21) | 7 | 2 | 12 |
| ŌĆāŌĆāCPH (n=1) | 1 | 0 | 0 |
Table┬Ā2.
Responses According to Different Regimens of IFN-╬▒ (%)
| Regimen | Sustained responders | Non-sustained responders | Non-responders |
|---|---|---|---|
| Group A (n=7) | 3 (42.9) | 0 (0) | 4 (57.1) |
| Group B (n=5) | 2 (40.0) | 1 (20.0) | 2 (40.0) |
| Group C (n=10) | 3 (30.0) | 1 (10.0) | 6 (60.0) |
Table┬Ā3.
Virological Characteristics of Three Responders Treated IFN-╬▒ Therapy
| Characteristics | Sustained responders | Non-sustained responders | Non-responders |
|---|---|---|---|
| Serum HCV RNA Positivity before therapy (%) | |||
| 8 (100) | 2 (100) | 12 (100) | |
| HCV Genotypea (%) | |||
| ŌĆāŌĆāType 1a (n=0) | 0 (0) | 0 (0) | 0 (0) |
| ŌĆāŌĆāType 1b (n=14) | 5 (35.7) | 2 (14.3) | 7 (50.0) |
| ŌĆāŌĆāType 2a (n=7) | 3 (42.9) | 0 (0) | 4 (57.1) |
| ŌĆāŌĆāType 2b (n=0) | 0 (0) | 0 (0) | 0 (0) |
| ŌĆāŌĆāUndetermined (n=1) | 0 (0) | 0 (0) | 1 (100) |
| Serum HCV RNA level before therapy (logcopies/ml)b | |||
| 5.76┬▒0.39c | 6.8┬▒0.71 | 6.70┬▒0.40 | |
REFERENCES
1. Choo QL, Kuo G, Weiner AJ, Overby LR, Bradley DW, Houghton M. Isolation of cDNA done dervied from a blood-borne non-A, non-B viral hepatitis genome. Science 1989;244:359.


2. Alter HJ, Purcell RH, Shin JW, Melpolder JC, Houghton M, Choo QL, Kuo G. Detection of antibody to hepatitis C virus in prospectively followed transfusion recipients with acute and chronic non-A, non-B hepatitis. N Engl J Med 1989;321:1494.


3. Esteban JI, Viladomiu L, Gonzalez A, Hernandez JM, Roget M, Vargas V, Genesca J, Buti M, Guardia J, Houghton M, Choo QL, Kuo G. Hepatitis C virus antibody among risk groups in Spain. Lancet 1989;ii:294.

4. Hoofnagle JH, Mullen KD, Jones DB, Rustgi V, Di Bisceglie A, Peters M, Waggoner JG, Park Y, Jones EA. Treatment of chronic non-A, non-B hepatitis with recombinant human alpha interferon. N Engl J Med 1986;315:1575.


5. Di Bisceglie AM, Martin P, Dassianides C, Lisker-Melman M, Murray L, Waggoner J, Goodman Z, Banks SM, Hoofnagle JH. Recombinant interferon-alfa therapy for chronic hepatitis C: A randomized, double-blind, placebo-controlled trial. N Engl J Med 1989;321:1506.


6. Davis GL, Balart LA, Schiff ER, Lindsay K, Bodenheimer HC, Perrillo RP, Carey W, Jacobson IM, Payne J, Dienstag JL, Vanthiel DH, Tanburro C, Lefkowitch J, Albrecht J, Meschievitz C, Ortego TJ, Gibas A. Treatment chronic hepatitis C with recombinant interferon alfa: A multicenter randomized, controlled trial. N Engl J Med 1989;321:1501.


7. Shindo M, Di Bisceglie AM, Cheung L, Wai-Kuo Shin JW, Cristiano K, Feinstone SM, Hoofnagle JH. Decrease in serum hepatitis C viral RNA during alpha-interferon therapy for chronic hepatitis C. Ann Intern Med 1991;115:700.


8. Kobayashi Y, Watanabe S, Konishi M, Yokoi M, Ikoma J, Kakehashi R, Kojima Y, Suzuki S. Detection of hepatitis C virus RNA by nested polymerase chain reaction in sera of patients with chronic non-A, non-B hepatitis treated with interferon. J Hepatol 1992;16:138.


9. Bosch O, Tapia L, Quiroga JA, Carreno V. An escalating dose regimen of recombinant interferon-alpha 2a in the treatment of chronic hepatitis C. J Hepatol 1993;17:146.


10. Kanai K, Kako M, Okamoto H. HCV genotypes in chronic hepatitis C and response to interferon. Lancet 1992;339:1543.

11. Lau JYN, Davis GL, Kniffen J, Qian KP, Urdea MS, Chan CS, Mizokami M, Neuwald PD, Wilber JC. Significance of serum hepatitis C virus RNA levels in chronic hepatitis C. Lancet 1993;341:1501.


12. Yoshioka K, Kakumu S, Wakita T, Ishikawa T, Itoh Y, Takayanagi M, Higashi Y, Shibata M, Morishima MT. Detection of hepatitis C virus by polymerase chain reaction and response to interferon alfa therapy: relationship to genotypes of hepatitis C virus. Hepatology 1992;16:293.


13. Kato N, Ohkoshi E, Shimotohno K. Japanese isolates of non-A, non-B hepatitis viral genome show the sequence variation from other original isolate in the USA. Proc Jpn Acad 1989;65:219.

14. Okamoto H, Okada S, Sugiyama Y, Tanaka T, Sugai Y, Akahane Y, Machida A, Mishiro S, Yoshizawa H, Miyakawa Y, Mayumi M. Detection of hepatitis C virus RNA by a two-stage ploymerase chain reaction with two pairs of primers deduced from 5ŌĆ▓ -noncoding region. Japan J Exp Med 1990;60:215.
15. Enomoto N, Takada A, Nakao T, Data T. There are two major types of hepatitis C virus in Japan. Biochem Biophys Res Commun 1990;170:1021.


16. Kato N, Hijikata M, Ootsuyama Y, Nakagawa M, Ohkoshi S, Sugimura T, Shimotohno K. Molecular cloning of the human hepatitis C virus genome from Japanese patients with non-A, non-B hepatitis. Proc Natl Acad Sci USA 1990;87:9524.



17. Kato N, Ootsuyama Y, Ohkoshi S, Nakazawa T, Mori S, Hijikata M, Shimotohno K. Distribution of plural HCV types in Japan. Biochem Biophys Res Commun 1991;181:279.


18. Chayama K, Tsubota A, Arase Y, Saitoh S, Koida I, Ikeda K, Matsumoto T, Kobayashi M, Iwasaki S, Koyama S, Morinage T, Kumada H. Genotypic subtyping of hepatitis C virus. J Gastroenterol Hepatol 1993;8:150.


19. Simmonds P, Alberti A, Bonino F, Alter HJ, Bradley DW, Brechot C, Chan SW, Chayama K, Chen DS, et al. A proposed system for the nomenclature for genotypes of hepatitis C virus. Hepatology 1994;19:1321.


20. Yoon SK, Park YM, Chung KW, Kim BS, Kim WY, Chang SK, Cho MJ. Molecular typing of hepatitis C virus genome from sera and liver tissues of patients with anti-HCV positive chronic liver disease. Kor J Int Med 1993;8(2):66.



21. Piatak M Jr, Saag MS, Yang LC, Clark SJ, Kappes JC, Luk KC, Hahn BH, Shaw GM, Lifson JD. High levels of HIV-1 in plasma during all stages of infection determined by competitive PCR. Science 1993;259:1749.


22. Choo SH, So HS, Cho JM, Ryu WS. Association of hepatitis C virus particles with immunoglobulin: A mechanism for persisitent infection (manuscripti in submission).
23. Causse X, Godinot H, Chevallier M, Chossegros P, Zoulim F, Ouzan D, Heyraud JP, Fontanges T, Albrecht J, Meschievitz C. Comparison of 1 or 3 MU of interferon alfa-2b and placebo in patients with chronic non-A, non-B hepatits. Gastroenterology 1991;101:497.


24. Takada N, Takase S, Enomoto N, Takada A, Date T. Clinical backgrounds of the patients having different types of hepatitis C virus genomes. J hepatol 1992;14:35.


25. Hagiwara H, Hayashi N, Mita E, Takehara T, Kasahara A, Fusamoto H, Kamada T. Quantitative analysis of hepatitis C virus RNA in serum during interferon alfa therapy. Gastroenterology 1993;104:877.


26. Tsubota A, Chayama K, Ikeda K, Yasuji A, Koida I, Saitoh S, Hashimoto M, Iwasaki S, Kobayashi M, Hiromitsu K. Factors predictive of response to interferon-alpha therapy in hepatitis C virus infection. Hepatology 1994;19:1088.





 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print



