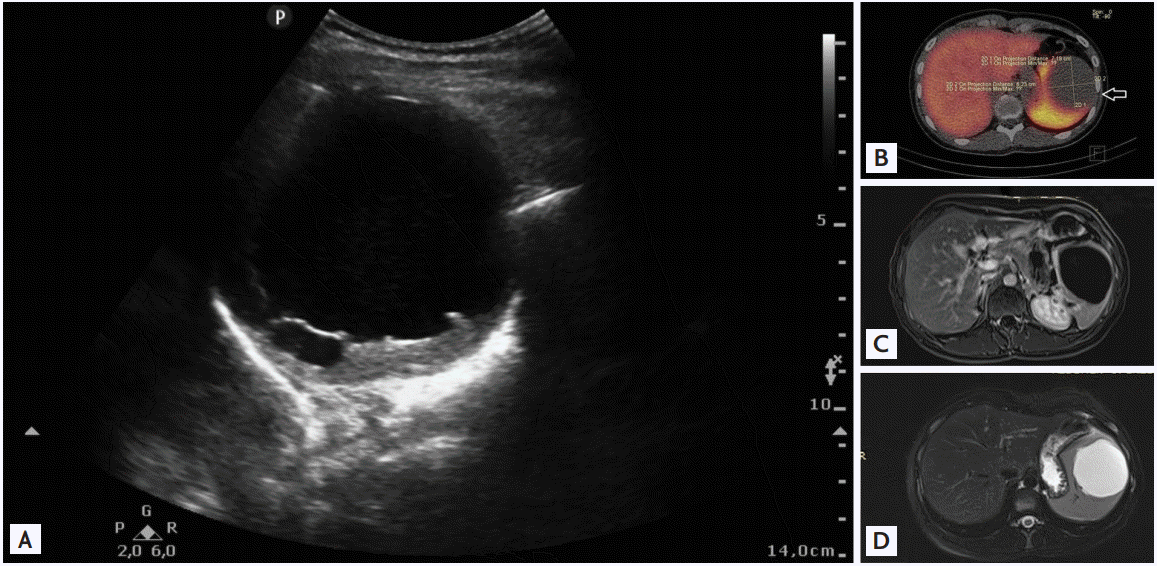
The 25-year old patient, was hospitalized due to the abdomen pain in the left upper quadrant, accompanied by watery diarrhoea, nausea, vomits, periodically occurring fever up to 39┬░C degrees with shivers and the body weight loss (15 kg during 2 months). There was conducted the extensive laboratory diagnostics and there was noted the high level of tumour markers in the plasma: cancer antigen 19.9 (CA19.9) 2,878 U/mL (N < 37 U/mL) and CA-125 95 U/mL (N < 35 U/mL). The results of several tests performed on fecal for parasite eggs and immunological tests of blood infection with hydit (ElisŌĆÖs and Western blotŌĆÖs methods) were negative. Within the diagnostic imaging was performed the ultrasound test of the abdomen, a static scintigraphy of the spleen and the liver with sulphidicid colloidŌĆö99mTc + single-photon emission computed tomography/computed tomography (CT), magnetic resonance of the abdomen and the lesser pelvic with giving the contrast agent (Fig. 1). The ultrasonography (US) revealed typical splenic cystsŌĆÖ features: the complex of homogeneous, anechoic, well separated cysts, with the largest of 90 ├Ś 80 mm, divided with a septum into two chambers. One was filled with homogenous hyperechoic content. In the magnetic resonance imaging (MRI) the cysts were: hypointense on T1-weighted images and hyperintense on T2-weighted images and intensity of the signal was similar to water and with no contrast uptake.
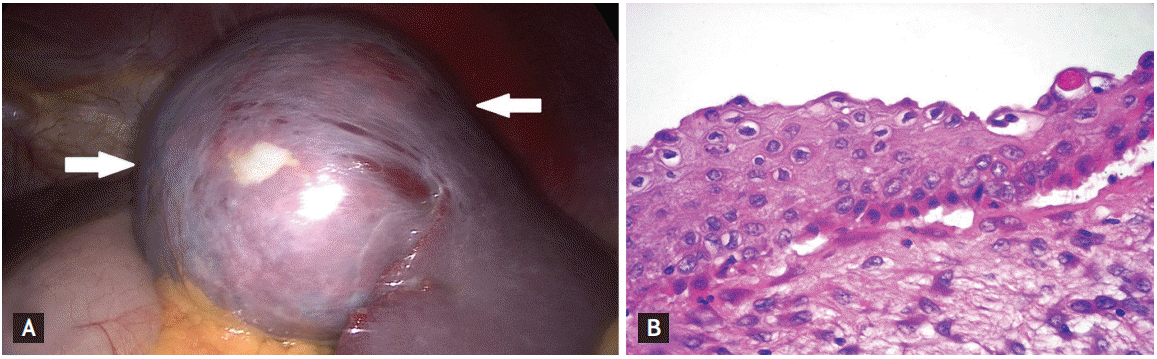
Complaints reported by the patient, weight loss and large sizes and unclear character of the splenic cysts qualified for the laparoscopic splenectomy. The liquid culture from the cysts was negative. A histopathology indicated an epidermoid cyst. A cyst wall composed of a thick layer of fibrous tissue was partly lined by thin multilayered nonkeratinizing squamous epithelium; squamous differentiation was confirmed by strong diffuse cytoplasmic expression of CK5/6 (Fig. 2). The postoperative course was not complicated. During the laboratory control (3 weeks after the surgery) was stated the normalization if the CA-125 level and significant (├Ś20) lowering of the CA19.9 level in plasma.
Coexistence of the increased CA19-9 and CA-125 in plasma with the epidermoid splenic cyst seems to be substantial in the differential diagnostics of the spleen lesions. In the diagnostics are also useful imaging tests like: the US and next CT or MRI. However the essential meaning has the histopathological testŌĆÖs result. In the case of the symptomatic cysts and of the large size (> 5 cm), the chosen treatment is the partial or complete splenectomy.



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print





