INTRODUCTION
Bisphosphonates are have been used for many years for a variety of conditions including Paget's disease, osteoporosis, multiple myeloma, and hypercalcemia of malignancy. They decrease bone resorption and hypercalcemia and reduce the osteolysis of bone metastasis [1]. A number of randomized clinical trials have shown that they increase bone density and reduce the incidence of fractures in osteoporosis [2]. Although bisphosphonates are generally safe and effective, concerns have been raised about the potential risk of over-suppression of bone turnover during long-term use. Odvina et al. [2] have reported on nine patients who sustained spontaneous non-spinal fractures while on alendronate therapy. Schneider [3] also described a 59-year-old previously healthy woman who experienced two non-traumatic stress fractures of the femur, 4 years apart, while on alendronate therapy. Armamento-Villareal et al. [4] reported a 35-year-old man who, after 6 years of treatment with 10 mg/day alendronate, had a sub-trochanteric fracture of the right femur after mild trauma. A bone biopsy showed a lack of osteoid on trabecular surfaces and an absence of tetracycline labeling, suggesting marked suppression of bone turnover.
Here, we describe a 63-year-old Korean woman who presented with non-traumatic spontaneous diaphyseal fractures of both femurs and delayed fracture healing after 5 years bisphosphonate therapy.
CASE REPORT
A 63-year-old woman was admitted to hospital because of severe pain in both anterior thighs for 5 months. The pain had been aggravating, and she could no longer walk by herself. When she presented with osteoporosis and degenerative arthritis 5 years ago, she started to take alendronate 70 mg/wk, alfacalcidol 0.5 µg/day and calcium citrate 1,900 mg/day. Three years later, she switched to risedronate 35 mg/wk and calcitriol 0.25 µg/day because of dyspepsia. She had total abdominal hysterectomy with bilateral salpingo-oophorectomy 35 years ago due to endometriosis.
At the time of admission, her height was 147 cm, and her weight was 54 kg; these had been 158 cm and 55 kg in her fourth decade. There was no history of any trauma, falling, or medication that predisposed to osteoporosis and fracture. She had no history of smoking and drinking alcohol. Her lifestyle had not been sedentary because she had to work in the fields for her living. Her diet was mainly composed of grains and vegetables. She ate fish once weekly and ate few dairy products. Physical examination revealed blood pressure of 100/80 mmHg, pulse rate of 80 beats/min, respiratory rate of 20 breaths/min, and body temperature was 36.5℃. Cardiac and abdominal examinations were normal. Here walking pattern could not be documented because of her pain. Both upper and lower extremities showed no structural abnormality or muscle weakness. There was kyphosis of her upper back. There was severe tenderness on both distal thighs. Straight leg raising and femoral nerve stretching tests were both negative.
Laboratory tests showed hemoglobin 12.2 g/dL, white blood cell count 4,910/mm2, platelet count 334,000/µL, serum calcium 9.3 mg/dL, serum phosphorus 3.2 mg/dL, total protein 7.5 g/dL, serum albumin 4.7 g/dL, uric acid 5.1 mg/dL, and alkaline phosphatase 72 IU/L. Daily urinary calcium excretion was 369.2 mg (normal, 70 to 180), and daily urinary phosphorous excretion was 959.92 mg (normal, 400 to 1,300). Serum protein electrophoresis showed no abnormality. Serum parathyroid hormone (PTH) was 18.92 pg/mL (normal, 10 to 65), and 25-(OH)-vitamin D, determined by commercially available radioimmunoassay kit (DiaSorin, Stillwater, MN, USA), was 15.33 ng/mL (normal, 9.0 to 37.6). Osteocalcin was 18.93 ng/mL (normal postmenopausal, 19.6 to 41.2), serum C-telopeptide, 0.301 ng/mL (normal postmenopausal, 1.008), and urine N-telopeptide was 55.7 nBCE/mM Cr (normal postmenopausal, 6.0 to 125.72).
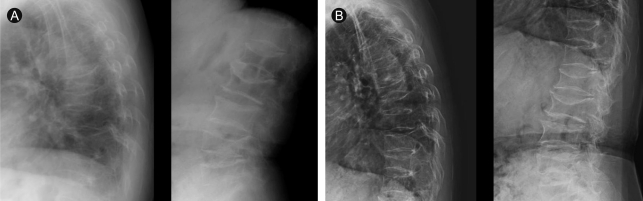
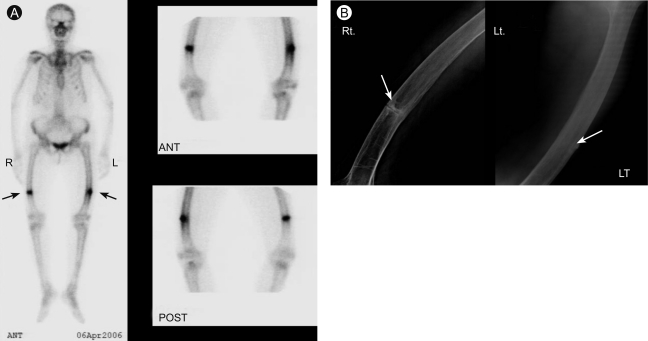
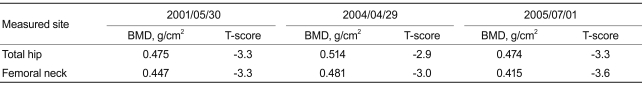
Simple X-rays of the thoracic and lumbar spine showed diffusely decreased vertebral height with osteoporosis and multiple compression fractures of T4, T5, T11, L1, L2, L4, and L5 vertebrae. There was no additional compression spinal fracture compared with X-rays taken 2 years earlier (Fig. 1). The most recent bone mineral density (BMD), measured by dual-energy X-ray absorptiometry (QDR-4500A, Hologic, Waltham, MA, USA), showed a T-score at the third lumbar vertebra of -3.8 and a total hip T-score of -3.3 (Table 1). All of the results showed severe osteoporosis, and no improvement in BMD was seen, despite bisphosphonate treatment. Whole spine magnetic resonance imaging revealed multiple compression fractures in the T4, T5, T11, L1, L2, L4, and L5 vertebral bodies and diffuse disk bulging at L2-3, L3-4, and L4-5, with degenerative changes of facet joints and thickening of ligamentum flavum. There was no definite evidence of thecal sac compression. A whole-body bone scan, which was obtained 2 hours after injecting technetium-99m hydroxymethylene diphosphonate (HDP) intravenously, showed intense uptake at both distal femurs. Simple X-rays also showed fracture lines in both distal femur shafts, compatible with sites of pain (Fig. 2).
After spinal nerve block with walking rehabilitation therapy was done for pain control, pain was not improved. Therefore, we speculated that the delayed fracture healing of both distal femurs due to the long-term bisphosphonates therapy was the main cause of the pain. Bisphosphonate therapy was discontinued. However, the pain continued, and the fracture lines seemed to become aggravated and showed delayed fracture healing. Normally, femoral fracture takes about 6 weeks to be healed completely. However, the patient had surgical internal fixation at both femoral diaphyses because of non-union of the femoral fractures even after 6 months of observation without bisphosphonates (Fig. 3). The elapsed time from the first visit to surgical internal fixation was 7 months. During the operation, severe osteoporotic fracture was noted, but structural displacement was mild. Bone biopsy performed with surgical fixation showed decreased trabecular bone with massive fibrosis in the marrow space.
DISCUSSION
Alendronate, risedronate, ibandronate, and zoledronate, which are classified as amino-bisphosphonates, have much higher potency because they contain nitrogen in their side chain [1]. However, concerns have been raised about potential risk of over-suppression of bone remodeling during long-term use. Prolonged use of bisphosphonates may suppress bone turnover to the point that micro-damage persists and accumulates. In experimental animals, alendronate has been shown to inhibit normal repair of micro-damage arising from marked suppression of bone turnover, which results in macro-cracks [5]. Chronic over-suppression of bone turnover by bisphosphonates may allow secondary mineralization to continue, resulting in hard, brittle bone with an increased risk for fracture [6]. Other supportive evidence on over-suppression includes several reports of jaw osteonecrosis in patients treated with high doses of bisphosphonates [1]. Recently, Odvina et al. [2] reported nine patients (eight postmenopausal women and one man) who sustained unusual spontaneous non-spinal fractures while on alendronate therapy (10 mg/day or 70 mg/wk) for 3-8 years. Six of the nine patients had delayed or absent fracture healing for 4 months to 2 years during alendronate therapy, and four showed delayed fracture healing for 8-12 months even after discontinuation of alendronate. Although co-administration of estrogen or glucocorticoids appears to be a predisposing factor, this apparent complication also occurred with bisphosphonate monotherapy. All the patients had trabecular bone biopsies. All patients showed markedly suppressed bone formation, with reduced or absent osteoblastic activities.
Our case report described a woman who experienced non-traumatic spontaneous stress fractures while on bisphosphonate therapy and non-union of the femoral shaft fracture despite discontinuation of bisphosphonates. We were able to ensure good adherence to medication by her self-report and serial measurements of urinary N-telopeptide, one of the bone turnover markers, which showed a decrease of 62.5%, from 40.8 to 15.3 nBCE/mM Cr, during the first 3 months after initiation of bisphosphonate therapy and similar levels afterwards. Therefore, this case had the possibility of delayed fracture healing due to suppression of bone turnover by long-term use of bisphosphonates. Other possible causes of insufficiency or pathological fracture include osteoporosis-include osteomalacia, osteogenesis imperfecta, bone tumors (primary or metastatic), and Paget's disease of bone. However, she had no definite clinical and laboratory evidence of such diseases. Bisphosphonates are incorporated into the skeleton without degradation. Therefore, their skeletal half-life is remarkably long. The residual effect on bone density is known to remain for 3 years after drug withdrawal [7], and it is possible that the suppressive effect of bisphosphonates on bone resorption might also be cumulative over time. Therefore, close monitoring and assessment of fracture healing after internal fixation in this patient was mandatory, considering the risk of re-fracture. The fixed pins were maintained, and she showed full union status 6 months after internal fixation.
In this patient, the biochemical markers such as N- and C-telopetides and serum osteocalcin showed normal levels and did not reveal magnitude of the suppression of bone turnover. The case reports of Odvina et al. [2] and Chavassieux et al. [8] have shown similar results. The discordance between the histomorphometric and biochemical markers of bone turnover could be related to the variable degree of suppression at different skeletal sites, as the changes in biochemical markers are more reflective of changes in the whole skeleton [2]. Additionally, this patient showed somewhat elevated daily urinary calcium excretion, with normal serum calcium, phosphorus, and PTH level. The active vitamin D, calcitriol, was thought to be the cause of this hypercalciuria.
Although previous studies have shown the efficacy of bisphosphonates in the first 5 years of therapy in terms of improving bone density and reduced risk of fractures [9], additional studies are needed to determine how long bisphosphonates can safely be given. Recently, Black et al. [10] have compared the effects of discontinuing alendronate treatment after 5 years versus continuing for 10 years. The results confirmed the safety of alendronate for up to 10 years, including no increased fracture risk with long-term use [10]. However, even those who discontinued alendronate after 5 years showed no higher fracture risk, other than for clinical vertebral fractures, compared with those who continued alendronate. These results suggest that discontinuation of alendronate for up to 5 years does not appear to significantly increase fracture risk, except for the patients at very high risk of vertebral fractures. Furthermore, considering some definitive case reports, we must emphasize the need for awareness of recent controversies about the effect of long-term reduction of bone turnover on bone strength, especially the occurrence of awkward fractures at an unexpected site, as in this patient. The benefits of prolonged use of bisphosphonates must be carefully weighed against the potential adverse effects of over-suppression of bone metabolism.




 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print





