INTRODUCTION
Thrombotic thrombocytopenic purpura (TTP) is a condition characterized by thrombocytopenia, microangiopathic hemolytic anemia, and less frequently with neurological deficits, renal failure, and fever. TTP is a rare disease, and has been reported to affect only 3.7 persons per one million annually in the United States1). It frequently follows a fatal course; 95% of patients die within three months if not treated2). TTP pathogenesis has been associated with deficiencies in the metalloproteinase, ADAMTS13 (A Desintegrin And Metalloprotease with a ThromboSpondin like domain 13)3). The principal function of ADAMTS13 involves the cleavage of unusually large forms of von Willebrand factor (ULVWF), thereby preventing ULVWF multimers from accumulating in the circulation; platelet aggregation in TTP is thought to be the consequence of the binding of the platelets from ULVWF remaining in the circulation4, 5). Immunoglobulin G (IgG) autoantibodies that block the activity of ADAMTS13 have been detected in patients suffering from TTP; this may account for the impairment of ADMATS13 characteristically observed in cases of TTP6, 7).
Plasma exchange was introduced in the 1980s as a treatment for TTP, and is currently the treatment of choice for the condition2). The principal mechanism of action relevant to plasma exchange in this context is the removal of IgG autoantibodies and accumulating ULVWF, in addition to the replacement of ADMATS13. Although the response rate to plasma exchange has been reported to be as high as 80%, patients refractory to plasma exchange have also been reported2, 8, 9). In plasma exchange-resistant cases, high-dose corticosteroid infusions are often employed as a complement to continuing plasma exchange10). However, it remains unclear as to how to treat patients who are refractory to both plasma exchange and steroid therapy. High dose immunoglobulin infusions have been reported to induce complete remission in these refractory cases9, 11, 12). However, successful treatment via immunoglobulin infusions in cases refractory to both plasma exchange and steroid therapy has not previously been reported in Korea. In this report, we describe a case refractory to both plasma exchange and steroid treatment in which complete remission was achieved as the result of a high-dose immunoglobulin regimen.
CASE REPORT
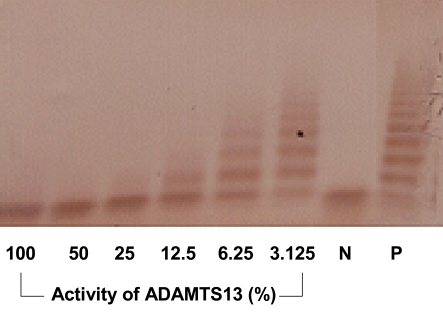
A 29-year-old male presented with disturbed mentality; aphasia had developed one day prior to presentation. The patient had a history of frequent epistaxis over the previous two weeks. The patient was otherwise healthy, with an unremarkable medical history. Upon physical examination, the conjunctivas were anemic, and multiple petechiae were detected on the patient's trunk. The results of the admission blood tests were as follows: hemoglobin (Hb) 7.1 g/dL, white blood cells (WBC) 5,540/uL, platelet (PLT) counts 4,000/uL, reticulocytes 18.9%, and serum LDH 1,655 IU/L. The brain MRI revealed no abnormal findings, such as hemorrhaging or inflammation; an 18-channel EEG revealed moderate to severe cerebral dysfunction. A mild fatty liver and splenomegaly were noted on abdominal US. The peripheral blood smear evidenced normocytic normochromic anemia and severe thrombocytopenia; these findings were compatible with microangiopathic hemolysis including schistocytosis. The results of both direct and indirect Coombs' tests were negative. SDS-agarose gel electrophoresis for ADAMTS 13 indicated that the ADAMTS 13 activity was as low as 0.89% (Reference value: 50~150%, Figure 1).
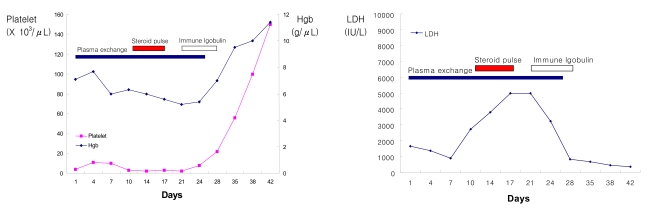
The patient was diagnosed with TTP, and plasma exchange was immediately initiated. However, after 14 days of daily plasma exchange treatments with fresh frozen plasma or cryoprecipitate-depleted plasma, the patient's hematological and cognitive abnormalities remained unimproved: Hb 7.3 g/uL, WBC 4,500/uL, PLT 5,000/uL, and serum LDH 1,665 IU/L. Therefore, the patient was started on a regimen of high-dose methylprednisolone (2 mg/kg) twice daily on Day 10, as a complement to continuing plasma exchange. High-dose steroids were infused intravenously after plasma exchange each day. However, the patient did not respond to this treatment, and the disturbed mentality and thrombocytopenia persisted. We then initiated intravenous infusions of high dose human immunoglobulin (400 mg/kg) on Day 21. After commencing the human immune globulin infusions, the patient's mentality began to show improvements, and the number of PLT increased gradually, up to 100,000/uL (Figure 2). At that point, we discontinued the plasma exchange regimen. The patient's cognitive abilities recovered completely, and the follow-up EEG evidenced no abnormal findings. The patient's hematological findings were normalized as follows: Hb 13.5 g/uL, PLT 234,000/uL, serum LDH 355 IU/L. The patient remains well after 18 months follow-up, with no signs of relapse.
DISCUSSION
Since the introduction of plasma exchange as a treatment, the mean number of plasma exchanges required to induce complete remission for TTP has been reported to be 7 to 16 exchanges13). An initial response is normally observed within the first three days of treatment10). However, 10 to 20 percent of patients evidence a transient, incomplete, or no response to plasma exchange; it is not currently possible to identify poor responders prior to treatment. Thus far, no treatment strategy for TTP refractory to plasma exchange has been established. In cases of poor response or resistance to plasma exchange, several treatment modalities have been recommended.
First, the frequency of plasma exchange can be increased from once daily to twice daily; twice-daily exchanges of one volume of plasma have been demonstrated to constitute a more effective replacement therapy than increasing the volume of a single daily exchange14). However, the economics inherent to such an approach must be considered, as only a limited number of plasma exchanges are covered by Korean medical insurance. Second, the cryosupernatant fraction of the plasma (also known as the cryoprecipitate-depleted plasma) can be employed, rather than fresh frozen plasma; the efficacy of plasma exchange may be attenuated by VWF multimers which normally remain in the fresh frozen plasma. Cryoprecipitate-depleted plasma tends to contain a very low level of VWF, because cryoprecipitate is quite rich in VWF15, 16). However, a randomized, controlled trial identified no difference in efficacy between whole plasma and cryoprecipitate-poor plasma17). In our case, we attempted to use cryoprecipitate-depleted plasma, but effected no improvements in either the neurological or hematological manifestations.
Third, additional immunosuppressive treatments have been shown to elicit successful responses in cases of refractory TTP. These treatments utilize high-dose steroids or other immunosuppressive agents, including cyclophosphamide, vincristine, and cyclosporine. However, there is currently no data from clinical trials to corroborate the efficacy of such treatments14). In the case described herein, we applied high-dose steroids with intravenous infusions of methylprednisolone (125 mg) twice daily while continuing plasma exchanges. However, this treatment failed to improve the patient's condition. Recently, the anti-CD20 monoclonal antibody, rituximab, has been reported to induce complete remission in cases of TTP refractory to plasma exchange18, 19). Weekly infusions of rituximab (375 mg/m2) proved effective in the control of the neurological and hematological manifestations, ostensibly as the result of the depletion of B-lymphocytes, which were generating the IgG autoantibodies. These findings support notion that IgG autoantibodies against ADAMTS13 are important in the management of TTP. In addition, a previous report suggested that high titers of IgG autoantibodies might be associated with resistance to plasma exchange in TTP patients8).
Another possible treatment approach is high-dose immunoglobulin infusions. The rationale for the use of immunoglobulin is based on the fact that immunoglobulin is capable of neutralizing IgG autoantibodies against ADAMTS1320). Although a retrospective study has reported that the application of immunoglobulin had no additional benefits21), many case series reports have noted the efficacy of immunoglobulin in the management of TTP refractory to plasma exchange9, 11, 12). Our experience supports the use of high-dose immunoglobulin infusion as an effective salvage treatment for cases of TTP refractory to plasma exchange.
Plasma exchange should continue to be the first-line treatment for patients diagnosed with TTP. However, appropriate salvage treatment should be considered without delay in cases refractory to both repeated plasma exchange and high-dose steroid therapy. High-dose immunoglobulin infusions may represent a useful treatment option for these refractory cases. In addition, this treatment may facilitate recovery and reduce the plasma exchange requirements. However, further study is warranted to determine the optimal treatment protocols for high-dose immunoglobulin therapy.



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print





